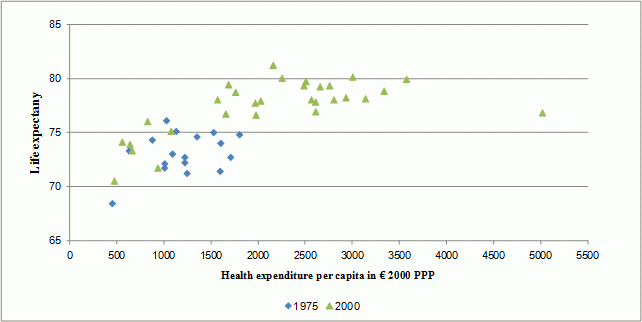
The share of older people in the population is growing faster than that of any other age group, both as a result of longer lives and a lower birth rate. But the effect of population ageing on health and healthcare is far from straightforward. Figure 1 plots life expectancy against health expenditure for 30 OECD countries in 1970 and 2005. The positive correlation is evident, although it is less distinctive at high levels of healthcare expenditure. In fact, some studies already find that age does not explain healthcare expenditures when distance to death, income, or life expectancy is controlled for (Zweifel et al. 1999; Hall and Jones 2007; Shang and Goldman 2007). More generally, expected cumulative health expenditure for healthy elderly individuals are similar to those for less healthy individuals of all ages. This evidence suggests the existence of a “red herring”.
Figure 1. Per capita health expenditure and life-expectancy in OECD countries
Source: OECD Health Data 2008
What if ageing takes place simultaneously with improvements in health status?
Inevitably, any attempt to measure the impact of ageing on healthcare use and expenditure requires some assumptions on health and life expectancy of future cohorts. For instance, if longevity results from improvements in health status and lower (or rather depressed) mortality, then the effect of ageing on health expenditure will be overestimated. The latter can also be due to improvements in medical technology. Indeed, we show that the advancement of medical technology for the treatment of individuals older than 55 years has contributed between 17.7% (Spain) and 38.3% (Switzerland) to the increase of men’s life expectancy between 1950 and 1975. In the last quarter of the past century, the gains in life-years of older men contributed between 60% (Germany) and 72% (UK) to the total increase in life expectancy (Breyer et al 2010).
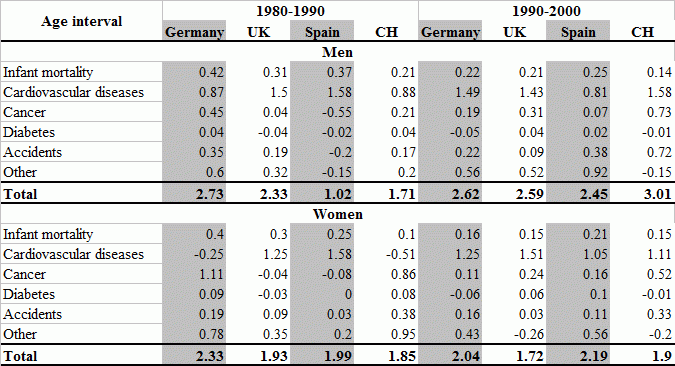
Table 1 displays the gains in life expectancy by gender between 1980 and 2000 (Breyer et al. 2010). Importantly, it shows that the largest single contributor to higher life expectancy is the reduction in mortality from heart disease and stroke. The latter added between one and three years to life expectancy, with higher gains for men than for women and in the 1990s as compared to the 1980s. The large life-year gains of the very old are to a great extent due to advancements in treating heart attacks and strokes. This highlights the importance of health treatment and new technologies in the development of life expectancy.
Table 1. Gain in life expectancy in years by death causes, men, 1980-2000
Sources: European Mortality Database, WHO (Germany, Spain), federal offices of statistics (Germany and Switzerland)
In addition to the compression of mortality, a second important way ageing can improve health status is by reducing the onset of disability in old age (compression of morbidity). That is, cumulative lifetime disability arguably declines if primary prevention measures postpone the onset of chronic illness (Fries 1980). However, as we report in Breyer et al. (2010), evidence on this is mixed and reveals declines in disability rates among elderly people only in Denmark, Finland, Italy, the Netherlands, and the US. In contrast, Belgium, Japan, and Sweden report an increasing disability rate, while Australia and Canada report a stable rate.
So is there a red herring?
Evidence suggests that neglecting time to death in the regression model leads to a15% overestimation of the Medicare expenditure increase (Stearns and Norton 2004), 10% in the Netherlands (Polder et al. 2006) and 20% in Germany (Breyer and Felder 2006). However, even though the red herring effect exists, ageing seems to explain only 0.5%-0.7% of annual health expenditure growth (Steinmann et al. 2007). On the whole, technological progress in medicine is the most important factor in explaining the growth of healthcare expenditure, although we also find that the rise in longevity leads to further demand for life-prolonging medical care. Moreover, as ever more people reach a very high age (beyond 85), the percentage requiring long-term care in their last years of life increases. On the whole, there is thus a small positive effect of ageing on per-capita health expenditure, which several studies estimate to be in the order of an annual growth rate of 1.5%.
What are the policy implications?
The fixation of policymakers on ageing seems to suggest that higher healthcare expenditure is inevitable, in fact diverting attention from the real causes of growth of the healthcare sector. These include failures in insurance markets, technological progress in medicine combined with a secular rise in income, and distorted incentives in reimbursing both patients and doctors. Blaming population ageing distracts from the decisions that really ought to be made, such as devising appropriate incentives for curbing excessive provision of publicly financed healthcare and evaluating the social value of new medical technologies.
References
Breyer, F, and S Felder (2006), “Life Expectancy and Health Care Expenditures: A new Calculation for Germany using the Costs of Dying”, Health Policy, 75(2):178-186.
Breyer, F, J Costa-Font, and S Felder (2010), “Ageing, health, and health care”, Oxford Review of Economic Policy.
Hall, RE, and CI Jones (2007), “The Value of Life and the Rise in Health Spending”, The Quarterly Journal of Economics, 122(1):39-72.
Polder, JJ, JJ Barendregt, and H van Oers (2006), “Health care costs in the last year of life--the Dutch experience”, Social Science and Medicine, 63(7):1720-1731.
Steinmann, L, H Telser, and P Zweifel (2007), “Aging and Future Health Care Expenditure: a Consistent Approach”, Forum for Health Economics & Policy, 10(2):1-30.
Zweifel P, S Felder, and M Meier (1999), “Ageing of Population and Health Care Expenditure: A Red Herring?”, Health Economics, 8(6):485-496.