The economic risk of an epidemic is very distinct from the its health (morbidity and mortality) risk. In fact, the two risks – the economic and public health – can be uncorrelated with each other. Some countries and regions that do not experience much morbidity and mortality may suffer very adverse economic consequences, while the opposite is also possible. As such, it is crucial not to focus only on ‘confirmed’ cases, ‘possible’ cases, and direct mortality when evaluating an epidemic’s economic impact.
Epidemics always arise out of a natural pathogen, but the pathogen by itself does not create the epidemic and definitely not its economic consequences. For that, the pathogen must encounter a society, people, and an economy that is both exposed and vulnerable to it.
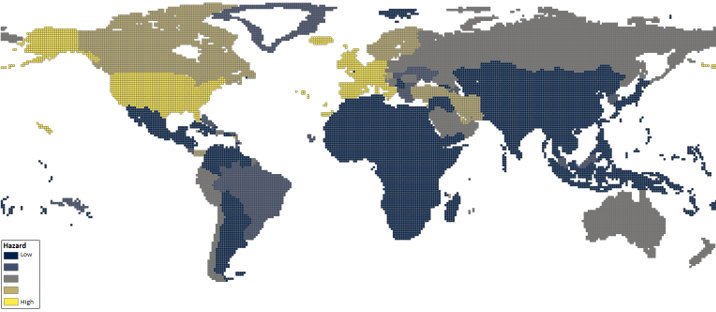
Generally, the framework that assesses disaster risk is constructed around four concepts: hazard, exposure, vulnerability, and resilience. It is the interaction of these four that leads to economic consequences. The hazard is the natural trigger that is the initial cause of the shock, in this case the SARS-Cov-2 virus. The economic risk, however, is determined not only by the virus, but also exposure to it, vulnerability to it, and the resilience of the economy that experiences it.
Resilience, in this framework, is conceptualised as the ability of the economy to bounce back given the magnitude of the shock (generated by the intersection of the hazard, exposure, and vulnerability). The degree of resilience in an economy is its capacity to recover, and is thus determined by the speed at which the recovery process occurs, and when the system reverts back to its pre-shock level (Hallegatte 2014, UNDRR 2017). Prager et al. (2017) observe that resilience policies are often not likely during the rapid phase of the spread of the epidemic. In the COVID-19 case, however, many governments are using extensive fiscal spending and lending programs to prepare the economy for the recovery period while the epidemic is still ongoing. The ability to implement such programs, as determined by both financial and institutional capacity, is therefore an important determinant of economic resilience.
It is thus almost inevitable that the economic risk will have a very different spatial variability than the spread of the virus itself.
Given the paucity of data on previous epidemic cases in the recent past, and the unprecedented nature of this event, our aim here is not to precisely measure the likely consequence of this pandemic, but rather to comparatively evaluate where the economic risk of COVID-19 is currently concentrated using several alternative algorithms.
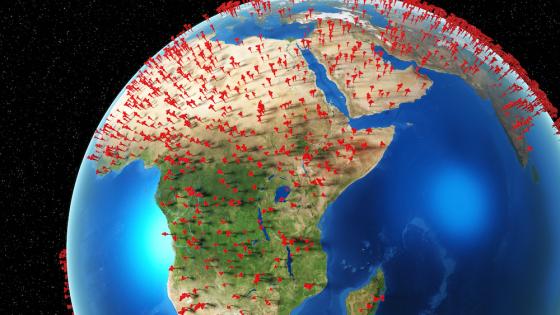
In a previous paper (Noy et al. 2019), we aimed to measure the economic risk of a generic epidemic. Here, we focus on COVID-19 (Figure 1). This virus perfectly fits the pattern of a zoonotic pathogen emerging from the interaction of a wild animal population with a food market that epidemiologists have been warning about (e.g. Allen et al. 2017). However, the economic characteristics of this unprecedented event are different (for example, the total collapse of the international tourism is unique) and we therefore modified our risk measurement to fit this new experience.
Figure 1 COVID-19 hazard map (ratio of confirmed cases to population)
Notes: Data updated: 20 April 2020.
In order to obtain a measure of economic risk, at the level of a one-degree grid cell, we model the risk associated with the economic impact of epidemics as a linear combination of the hazard, the local economy’s exposure and vulnerability to it, minus the economy’s resilience or ability to bounce back. We collect a large group of sub-national and national measures from recent years to proxy for exposure, vulnerability, and economic resilience. The selection of variables is based on the literature measuring disaster risk, as reviewed in Yonson and Noy (2018), and on the current experience of COVID-19. The details are available in Noy et al. (2020).
We use principal component analysis to compute a standardised index for each grid cell’s exposure, vulnerability, and resilience. Using the first component of the exposure, vulnerability, and resilience indices, in addition to the number of confirmed cases of COVID-19, we compute a risk index in relation to the economic risk of epidemics. In our simplest specifications, we assume equal weights (Figure 2). In an alternative algorithm, we assume that the hazard is identical for all countries. In the last iteration, we estimate the optimal weight for each component of the index using a measure of past economic risk of communicable diseases in each country. This last measure is constructed from information about Disability Adjusted Life Years (DALY) associated with communicable diseases in each country.
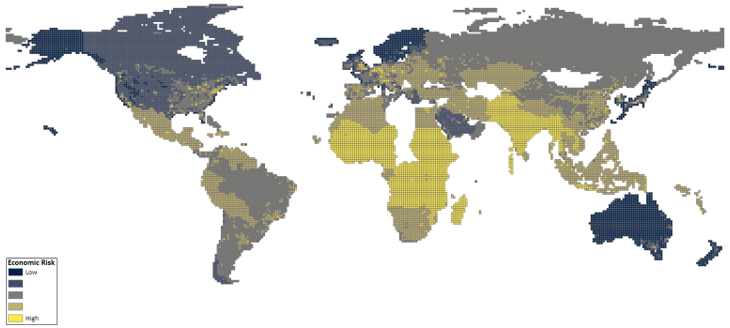
We find that the economic risk of epidemics is especially high in most of Africa, South Asia, Iran, and much of Southeast Asia (Figure 2). The economic risk is high in Africa and South Asia, as these are the most vulnerable areas with low income and healthcare quality. Resilience, intentionally or otherwise, plays a role in reducing the economic risk from epidemics. For example, in the Southern Cone countries (Argentina, Uruguay, and Chile) the resilience is higher than neighbourhood countries due to less fractionalised societies (lower ethnic and linguistic disparity) and higher incomes. Meanwhile, Saudi Arabia and Russia have lower economic risks because their domestic economies hardly rely on any tourism at all.
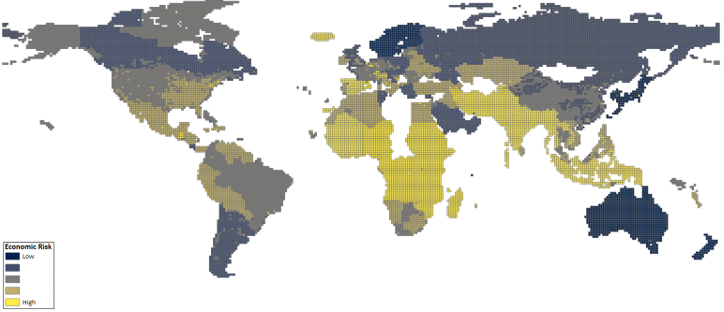
Figure 2 Economic risk of COVID-19 (equal weights)
Notes: Economic risk of COVID-19 measured with equal weights and the number of confirmed COVID-19 cases as of 20 April 2020.
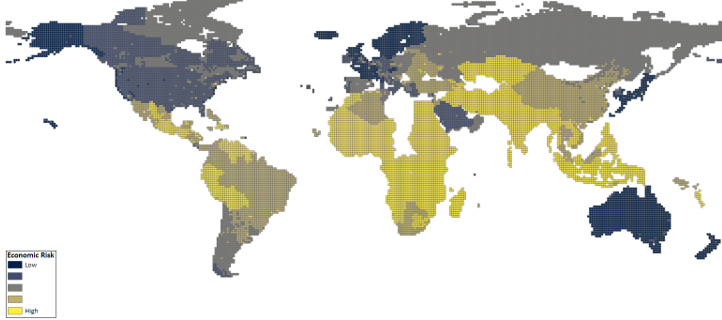
In Figure 3, we assume that the hazard (the presence of the virus) is identical in all countries. This can be motivated either by the expectation that eventually, the spread of the virus will reach epidemic levels in all countries (and that anyway the number of cases is probably mis-measured). Besides some expected differences, however, the results presented in Figure 3 (uniform spread of the virus) and Figure 2 (hazard based on the recent spread of the virus) are very similar. The only distinctive difference is that the countries of Southern Europe that have very high official infection rates (e.g. Italy and Spain) are assessed to be at a comparably lower risk in Figure 3 (when we assume a uniform level of the hazard). Meanwhile, the risk is higher in most of Latin America (except for the Southern Cone countries).
Figure 3 Economic risk of COVID-19 (equal weights, equal hazard)
Notes: Economic risk of COVID-19 using equal weights but with the hazard calibrated so all countries have an equal hazard (all are susceptible to COVID-19).
Our third alternative index relies on a less ad-hoc weighting scheme based on the Disability-Adjusted Life Years measure of communicable disease burden. Weights for each of the four components are derived by OLS regressions with the country-level DALYs as the dependent variable. As before, the areas facing highest economic risks from the pandemic remain in Sub-Saharan Africa and South Asia. But much of Central Asia, and South East Asia are considered less risky with this approach, as are some other areas that are relatively poor, but not too densely populated (as is Central America, for example).
Figure 4 Economic risk of COVID-19 (DALY-weighted index)
The economic consequences of an epidemic, like any other natural hazard shock, can be delineated into direct damages and indirect losses (Noy 2016). If measured through the standard statistical tools used by governments to evaluate the cost of life (the Value of Statistical Life), the direct damages of COVID-19 due to illness and mortality are probably much smaller than the indirect losses brought about by the massive crisis engendered by the pandemic. This is especially true now for countries in which the epidemic has not yet spread indiscriminately, but that are very exposed to the global shock it created (for example, in tourism-dependent economies in the global South).
As public health systems have improved over the past century, this pandemic’s health impacts are unlikely to be of the magnitude of the 1918-19 Influenza pandemic, though it may still be of catastrophic scale. However, what remains salient, maybe even more than in 1918-19, is the current pandemic’s economic consequences. The exposure, vulnerability, and resilience to these economic consequences were not ameliorated as much when public health systems developed throughout the last century. On the contrary, globalisation of trade, increased tourism and labour flows, and the more recent advent of social media, are all likely to have amplified behavioural responses and generated additional vulnerabilities for the world economy, thus potentially exacerbating the economic losses. Philipson (2000) observed that when private behaviour is strongly prevalence-elastic, the main economic cost of a disease outbreak is likely to arise out of preventative actions rather than directly from infections. This was true for SARS in 2003 (Noy and Shields 2019) and is much truer for COVID-19.
To summarise, what is most apparent from our analysis is that the economic risk from COVID-19 is not located in Northern Italy or New York City. Rather, the highest economic risks are in countries and regions that do not get much global attention even in normal times and get even less in the midst of the frantic reporting on the pandemic’s spread now. This is unfortunate, as ultimately, the economic costs will be borne there, away from the public eye.
References
Allen, T, K A Murray, C Zambrana-Torrelio, S S Morse, C Rondinini, M Di Marco, N Breit, K J Olival and P Daszak (2017), “Global hotspots and correlates of emerging zoonotic diseases”, Nature communications 8(1), 1124.
Hallegatte, S (2014), “Economic Resilience: Definition and Measurement”, World Bank Policy Research Working Paper 6852.
Noy, I (2016), “Tropical storms: The socio-economics of cyclones”, Nature Climate Change 6(4), 343.
Noy, I, N Doan, B Ferrarini and D Park (2019), “Measuring the Economic Risk of Epidemics”, CESifo Working Paper 8016.
Noy, I, N Doan, B Ferrarini and D Park (2020), “Measuring the Economic Risk of COVID-19”, Covid Economics 3: 103-118.
Noy, I and S Shields (2019), “The 2003 Severe Acute Respiratory Syndrome Epidemic: A Retroactive Examination of Economic Costs”, Asian Development Bank Working Paper.
Perrings, C, C Castillo-Chavez, G Chowell, P Daszak, E P Fenichel, D Finnoff, R D Horan, A M Kilpatrick, A P Kinzig and N V Kuminoff (2014), “Merging economics and epidemiology to improve the prediction and management of infectious disease”, EcoHealth 11(4): 464-475.
Philipson, T (2000), “Economic epidemiology and infectious diseases”, Handbook of health economics 1: 1761-1799.
Prager, F, D Wei and A Rose (2017), “Total economic consequences of an influenza outbreak in the United States”, Risk Analysis 37(1): 4-19.
UNDRR (2017), “Terminology on Disaster Risk Reduction”, United Nations Office for Disaster Risk Reduction.
Yonson, R and I Noy (2018), “Economic Vulnerability and Resilience to Natural Hazards: Concepts and Measurements”, Sustainability 10, 2850.