Physicians tend to enjoy good physical health. The typical physician exercises more, is less likely to smoke, and is less likely to be obese than his or her non-physician counterpart (Nelson et al. 1994, Frank et al. 1998, Abramson et al. 2000, John and Hanke 2003, Smith and Leggat 2007, Leuven et al. 2013). In the US, physicians live an average of two years longer than other professionals, and almost three years longer than members of the general population (Frank et al. 2000).
Although physically healthy, there is evidence that physicians disproportionately suffer from mental health problems and substance use disorder (SUD). More than 20% of physicians are depressed or exhibit symptoms of depression (Mata et al. 2015, Rotenstein et al. 2018, eTable 24); 10–15% of physicians will misuse alcohol or prescription drugs during their career (Baldisseri 2007, Vayr et al. 2019); and at least a third of physicians describe themselves as suffering from ‘job burnout’ (Drummond 2015), a syndrome closely linked to depression and SUDs (Bianchi et al. 2015, Schonfeld and Bianchi 2016, Wurm et al. 2016, Stageberg et al. 2020). Compounding these problems, physicians are often reluctant to seek psychologic help, perhaps out of shame or fear of losing their license (Dyrbye et al. 2017, Tay et al. 2018, Weiner 2020, Belluz 2021).
Could becoming a physician lead, in a causal sense, to mental health problems and SUDs? Answering this question is important from a policy perspective. If, for instance, easy access to prescription drugs, the rigors of residency, and the threat of frivolous malpractice claims are encouraging physicians to abuse substances, then there are concrete steps that can be taken to shield them. Several US states (including New Jersey, New York, and Pennsylvania) have recently prohibited COVID-19 patients from filing medical malpractice lawsuits against their physicians (Caruso 2020). If, on the other hand, physicians are somehow predisposed to SUDs – if, for instance, their drug abuse is entirely explained by personality or other individual-level traits – then protecting them against malpractice claims will do nothing to solve the problem.
In a recent paper (Anderson et al. 2021), we explore the effect of becoming a physician on antidepressant use and the use of other prescription drugs such as anxiolytics, sedatives, and opioids. Anxiolytics and sedatives include a range of benzodiazepines (e.g. Xanax and Versed) that are popular among physicians seeking self-treatment (Moberly 2014, Khan et al. 2019). Similar to Oxycodone and other prescription opioids, benzodiazepines are addictive and come with an extremely high potential for abuse (American Addiction Centers 2021).
Our data are from the Netherlands, where the number of students admitted to medical school is tightly regulated: applicants outnumber available slots, and acceptance to medical school is determined at random, based on the results of an annual admissions lottery. Following Leuven et al. (2013), Ketel et al. (2016), and Artmann et al. (2021), we use the outcomes from these annual admissions lotteries as an instrumental variable (IV), allowing us to credibly distinguish the effect of becoming a physician from the effects of difficult-to-observe individual-level traits such as intelligence, personality, and perseverance, all of which are potentially correlated with the decision to become a physician, mental health, and substance use (Ashby et al. 2006, White et al. 2012, Lo and Abbott 2013, Karpinski et al. 2018, Leung et al. 2019, Eley et al. 2020).
Data on lottery outcomes for 27,464 medical school applicants were obtained from the Dienst Uitvoering Onderwijs, a Dutch governmental organisation under the Ministry of Education. We observe the outcomes of all medical school lotteries conducted between 1987 and 1999. (After 1999, the national lottery was replaced with a decentralised selection system that gave medical schools more control over the admissions process.) Data on each applicant’s prescription drug use for the period 2006–2018 came from the Dutch prescription reimbursement database, provided by Statistics Netherlands.
Becoming a physician and antidepressant use
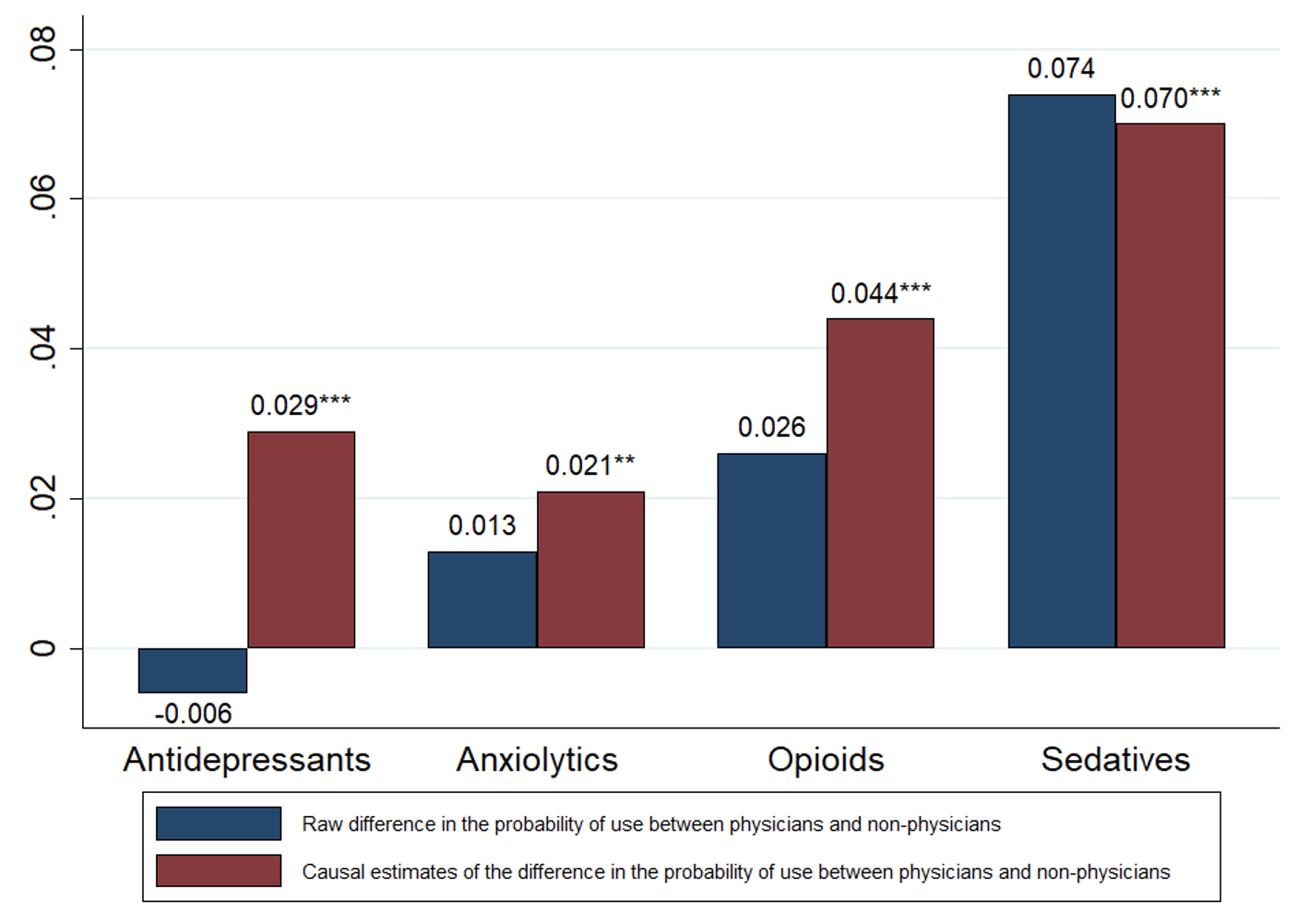
Our IV estimates indicate that applicants induced into becoming physicians by winning the admissions lottery are more likely to use prescription antidepressants than those who lose the lottery and go into a different profession. Specifically, we find that becoming a physician leads to a 0.029 increase in the probability of having been prescribed an antidepressant during the period 2006–2018, which represents 23% increase relative to the sample mean (Figure 1).
Figure 1 Prescription drug use among physicians vs non-physicians: Pooled sample
Notes: The sample is composed of 27,464 first-time medical school applicants in the Netherlands. Prescription drug use is for the period 2006–2018. Causal (i.e. IV) estimates are based on a regression model in which becoming a physician is instrumented using medical school lottery outcomes. IV estimates of the effect of becoming a physician control for gender, age at first lottery, lottery category fixed effects, year-of-first-lottery fixed effects, and lottery category by year-of-first-lottery fixed effects. *Statistically significant at 10% level, ** at 5% level, *** at 1% level.
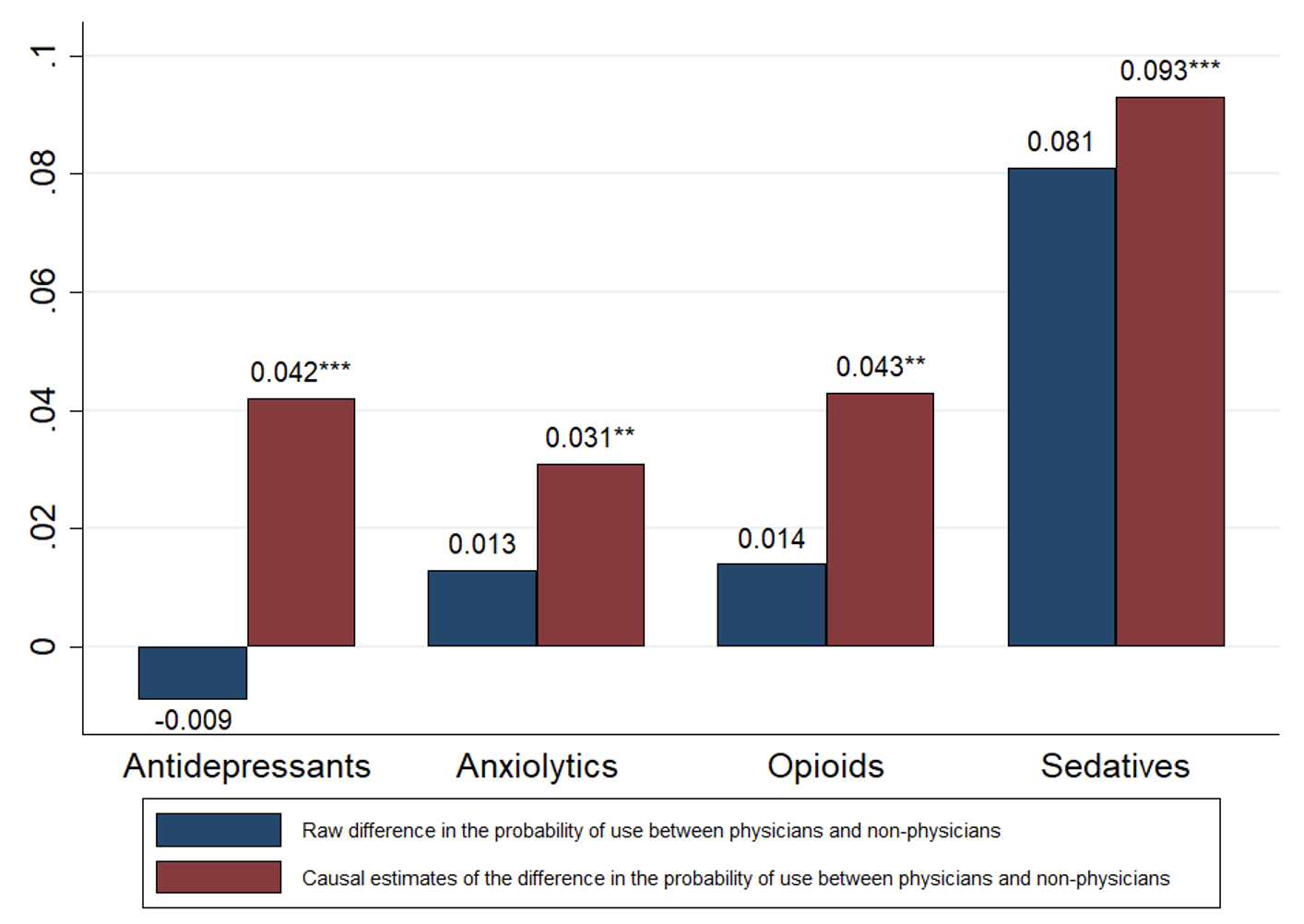
The medical literature describes female physicians as being at elevated risk for substance use disorder and depression (Oreskovich et al. 2015, Guille et al. 2017) and estimates from meta-analyses show that female physicians commit suicide at much higher rates than male physicians (Schernhammer and Colditz 2004, Duarte et al. 2020). When we split our sample by gender, becoming a physician leads to a 0.042 increase in the probability of having been prescribed an antidepressant among female applicants (Figure 2). Although also positive, the corresponding IV estimate for male applicants is much smaller and is nowhere near statistically significant at conventional levels (Figure 3).
Figure 2 Prescription drug use among physicians vs non-physicians: Sample restricted to female applicants
Notes: The sample is composed of 15,896 female first-time medical school applicants in the Netherlands. Prescription drug use is for the period 2006–2018. Causal (i.e. IV) estimates are based on a regression model in which becoming a physician is instrumented using medical school lottery outcomes. IV estimates of the effect of becoming a physician control for age at first lottery, lottery category fixed effects, year-of-first-lottery fixed effects, and lottery category by year-of-first-lottery fixed effects. *Statistically significant at 10% level, ** at 5% level, *** at 1% level.
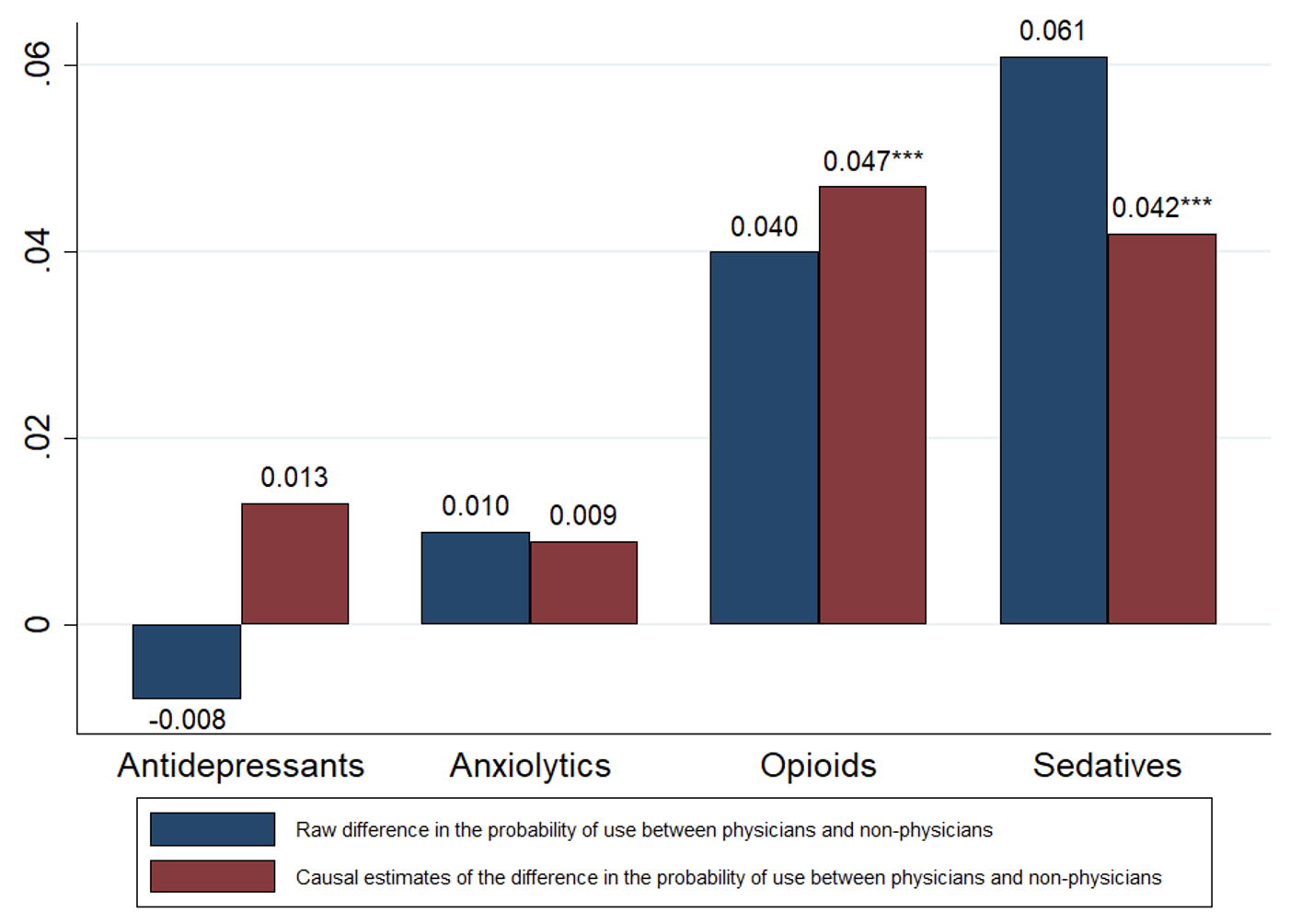
Figure 3 Prescription drug use among physicians vs non-physicians: Sample restricted to male applicants
Notes: The sample is composed of 11,568 male first-time medical school applicants in the Netherlands. Prescription drug use is for the period 2006–2018. Causal (i.e. IV) estimates are based on a regression model in which becoming a physician is instrumented using medical school lottery outcomes. IV estimates of the effect of becoming a physician control for age at first lottery, lottery category fixed effects, year-of-first-lottery fixed effects, and lottery category by year-of-first-lottery fixed effects. *Statistically significant at 10% level, ** at 5% level, *** at 1% level.
Becoming a physician and the use of anxiolytics, opioids, and sedatives
Why does becoming a physician increase antidepressant use among female medical school applicants? It is possible that there is something intrinsic to the profession that causes poor mental health and antidepressant use. However, our IV estimates provide evidence that becoming a physician increases the use of types of other prescription drugs, not just antidepressants. In our pooled sample (i.e. the sample composed of both male and female applicants), becoming a physician leads to a 0.021 increase in the probability of having been prescribed an anxiolytic (Figure 1). This estimate is 20% of the sample mean and is, in fact, more than large enough to explain the unadjusted (i.e. ‘raw’) gap in anxiolytic use between physicians and non-physicians. Becoming a physician is also associated with a 0.044 increase in the probability of having been prescribed an opioid (which is 25% of the sample mean), and a 0.070 increase in the probability of having been prescribed a sedative (which is 61% of the sample mean). Again, these IV estimates can explain the entire unadjusted gaps between physicians and non-physicians.
Among female applicants, becoming a physician leads to a 0.031 increase in the probability of having been prescribed an anxiolytic, or 27% of the mean (Figure 2). Female applicants who were induced into becoming a physician by winning the lottery were also more likely to use prescription opioids and much more likely to use prescription sedatives than their counterparts who lost the lottery and went into another profession. Restricting the sample to male applicants produces positive, but considerably smaller, IV estimates for anxiolytics and sedatives (Figure 3). Among male applicants, becoming a physician is associated with a 0.047 increase in the probability of having been prescribed an opioid (or 28% of the mean), which is comparable to the estimated effect among female applicants.
Summing up
We view the sizeable increases in the use of anxiolytics (e.g. Xanax), opioids (e.g. Oxycodone), and sedatives (e.g. Versed) among physicians in our sample as particularly worrisome. These drugs are highly addictive and there is descriptive evidence that they are often abused by physicians (Merlo and Gold 2008, Oaklander 2015, Moberly 2014, Khan et al. 2019). Although we cannot distinguish legitimate use from misuse in our data, it is clear that Dutch physicians are especially prone to using prescription drugs and that this phenomenon is entirely explained by their choice of profession as opposed to their personality or other difficult-to-observe individual-level traits.
References
Abramson, S, J Stein, M Schaufele, E Frates and S Rogan (2000), “Personal Exercise Habits and Counseling Practices of Primary Care Physicians: A National Survey”, Clinical Journal of Sport Medicine, 10(1): 40–48.
American Addiction Centers (2021), “Benzodiazepine Addiction: Symptoms & Signs of Dependence”, 20 December.
Anderson, D M, R Diris, R Montizaan and D I Rees (2021), “The Effects of Becoming a Physician on Prescription Drug Use and Mental Health Treatment”, IZA DP No. 14890.
Artmann, E, H Oosterbeek and B van der Klaauw (2021), “Do Doctors Improve the Health Care of Their Parents? Evidence from Admission Lotteries”, American Economic Journal: Applied Economics, forthcoming.
Ashby, J S, K G Rice and J L Martin (2006), “Perfectionism, Shame, and Depressive Symptoms”, Journal of Counseling and Development, 84(2): 148–156.
Baldisseri, M (2007), “Impaired Healthcare Profession”, Critical Care Medicine, 35(2 Suppl.): S106–S116.
Bianchi, R, I S Schonfeld and E Laurent (2015), “Burnout–Depression Overlap: A Review”, Clinical Psychology Review, 36: 28–41.
Belluz, J (2021), “The Doctors are Not All Right”, Vox.com, 23 June.
Caruso, S (2020), “Wolf Signs Executive Order Shielding Some Healthcare workers against Malpractice Claims during Pandemic”, Pennsylvania Capital Star, 6 May.
Drummond, D (2015), “Physician Burnout: Its Origin, Symptoms, and Five Main Causes”, Family Practice Management, 22(5): 42–47.
Duarte, D, M M El-Hagrassy, T C e Couto, W Gurgel, F Fregni and H Correa (2020), “Male and Female Physician Suicidality: A Systematic Review and Meta-analysis”, JAMA Psychiatry, 77(6): 587–597.
Dyrbye, L, C West, C Sinsky, L Goeders, D Satele and T Shanafelt (2017), “Medical Licensure Questions and Physician Reluctance to Seek Care for Mental Health Conditions”, Mayo Clinic Proceedings, 92(10): 1486–1493.
Eley, D S, V Bansal and J Leung (2020), “Perfectionism as a Mediator of Psychological Distress: Implications for Addressing Underlying Vulnerabilities to the Mental Health of Medical Students”, Medical Teacher, 42(11): 1301–1307.
Frank, E, H Biola and C Burnett (2000), “Mortality Rates and Causes Among U.S. Physicians”, American Journal of Preventative Medicine, 19(3): 155–159.
Frank, E, D Brogan, A Mokdad, E Simoes, H Kahn and R Greenberg (1998), “Health-Related Behaviors of Women Physicians vs. Other Women in the United States”, Archives of Internal Medicine, 158(4): 342–348.
Guille, C, E Frank, Z Zhao, D A Kalmbach, P J Nietert, D A Mata and S Sen (2017), “Work-Family Conflict and the Sex Difference in Depression Among Training Physicians”, JAMA Internal Medicine, 177(12): 1766–1772.
John, U and M Hanke (2003), “Tobacco-Smoking Prevalence among Physicians and Nurses in Countries with Different Tobacco-Control Activities”, European Journal of Cancer Prevention, 12(3): 235–237.
Karpinski, R, A K Kolba, N Tetreault and T Borowski (2018), “High Intelligence: A Risk Factor for Psychological and Physiological Overexcitabilities”, Intelligence, 66: 8–23.
Ketel, N, E Leuven, H Oosterbeek and B van der Klaauw (2016), “The Returns to Medical School: Evidence from Admission Lotteries”, American Economic Journal: Applied Economics, 8(2): 225–254.
Khan, A A, I U Din, A N Khan, I Khan, H Hanif and H Nawaz (2019), “Benzodiazepine Use among Resident Doctors in Tertiary Care Hospital”, Journal of Ayub Medical College, 31(4): 553–557.
Leuven, E, H Oosterbeek and I de Wolf (2013), “The Effects of Medical School on Health Outcomes: Evidence from Admission Lotteries”, Journal of Health Economics, 32(4): 698–707.
Lo, A and M J Abbott (2013), “Review of the Theoretical, Empirical, and Clinical Status of Adaptive and Maladaptive Perfectionism”, Behaviour Change, 30(2): 96–116
Leung, J, C R Cloninger, B Hong, K Cloninger and D Eley (2019), “Temperament and Character Profiles of Medical Students Associated with Tolerance of Ambiguity and Perfectionism”, PeerJ, 7: e7109.
Mata, D A, M A Ramos, N Bansal, R Khan, C Guille, E Di Angelantonio and S Sen (2015), “Prevalence of Depression and Depressive Symptoms Among Resident Physicians: A Systematic Review and Meta-analysis”, JAMA, 314(22): 2373–2383.
Merlo, L and M Gold (2008), “Prescription Opioid Abuse and Dependence among Physicians: Hypotheses and Treatment”, Harvard Review of Psychiatry, 16(3): 181–194.
Nelson, D, G Giovino, S Emont, R Brackbill, L Cameron, J Peddicord and P Mowery (1994), “Trends in Cigarette Smoking among US Physicians and Nurses”, JAMA, 271(16): 1273–1275.
Oaklander, M (2015), “Doctors on Life Support”, Time, 27 August 27.
Oreskovich M R, T Shanafelt, L N Dyrbye, L Tan, W Sotile, D Satele, C P West, J Sloan and S Boone (2015), “The Prevalence of Substance Use Disorders in American Physicians”, American Journal on Addictions, 24(1): 30–38.
Rotenstein, L S, M Torre, M A Ramos, R C Rosales, C Guille, S Sen and D A Mata (2018), “Prevalence of Burnout Among Physicians: A Systematic Review”, JAMA, 320(11): 1131–1150.
Schernhammer, E and G A Coldtiz (2004), “Suicide Rates among Physicians: A Quantitative and Gender Assessment (Meta-Analysis)”, American Journal of Psychiatry, 161(12): 2295–302.
Schonfeld, I and R Bianchi (2016), “Burnout and Depression: Two Entities or One?”, Journal of Clinical Psychology, 72(1): 22–37.
Smith, D and P Leggat (2007), “An International Review of Tobacco Smoking in the Medical Profession: 1974–2004”, BMC Public Health, 7: Article 115.
Stageberg, E L, A L Stark and K M Moore (2020), “Rates of Burnout, Depression, Suicide, and Substance Use Disorders”, Burnout in Women Physicians, Cham, Switzerland: Springer.
Tay, S, K Alcock and K Scior (2018), “Mental Health Problems Among Clinical Psychologists: Stigma and its Impact on Disclosure and Help-Seeking”, Journal of Clinical Psychology, 74(9): 1545–1555.
Vayr, F, F Herin, B Jullian, J M Soulat and N Franchitto (2019), “Barriers to Seeking Help for Physicians with Substance Use Disorder: A Review”, Drug and Alcohol Dependence, 199: 116–121.
Weiner, S (2020), “Doctors Forgo Mental Health Care During Pandemic Over Concerns about Licensing, Stigma”, Association of American Medical Colleges, 10 December.
White, J, C Gale and G D Batty (2012), “Intelligence Quotient in Childhood and the Risk of Illegal Drug Use in Middle-Age: The 1958 National Child Development Survey”, Annals of Epidemiology, 22(9): 654–657.
Wurm, W, K Vogel, A Holl, C Ebner, D Bayer, S Mörkl, I-S Szilagyi, E Hotter, H-P Kapfhammer and P Hofmann (2016), “Depression-Burnout Overlap in Physicians”, PLoS ONE, 11(3): e0149913.