In the face of ageing populations, developed countries are actively considering policies aimed at encouraging older people to work for longer. Many are increasing the age at which people can start claiming state-funded pensions. These policies have been shown to be effective at increasing employment rates (Mastrobuoni 2009, Staubli and Zweimuller 2013, Cribb et al. 2013, Atalay and Barrett 2015). However, one concern often raised is whether such policies are fair, given that some may be too unhealthy to continue working for any longer while waiting to receive their pension (DWP 2010). It is important, therefore, to investigate the extent to which ill-health limits the ability of older people to work.
As people get older they tend, on average, to be less healthy and to work less, but this evidence alone is not sufficient, since there are many other factors that also affect the labour force participation of older age groups, and also much heterogeneity within age groups. Instead, we need to understand how health affects individuals’ work capacity. By focusing here on health, our objective is not to diminish the importance of other factors, nor to draw conclusions about how much people should work (since many will prefer to retire, regardless of their health), but rather to suggest how much they could work given their health. We do this by investigating and describing the extent to which other people (with levels of health that are comparable to those of currently-older people) are, or have been observed, working.
We describe below two alternative approaches to try to estimate whether there appears to be potential – on the grounds of health alone – to increase employment rates among older people in England (Banks et al. 2016). This is relevant and topical in the UK – in light of the recently announced independent review of future increases in the state pension age by John Cridland (DWP 2016) – but also in many other advanced, ageing economies.
Each of the two approaches we present endeavours to estimate a ‘counterfactual’ employment rate for currently-older people. This counterfactual is intended to demonstrate the level of employment that would be seen among the group if health were the only factor affecting their employment rate. Each counterfactual is constructed using employment rates seen among another group of people who are in similar health – either those observed in earlier years or those observed in the same year but at a younger age.
Both approaches assume that work itself has no effect on health. This is a potentially important concern and the results discussed below should be interpreted with this caveat in mind.
Did similarly healthy people work more or less in the past?
The first approach (following Banks et al. 2012 and Milligan and Wise 2012) compares employment rates of currently older people to the employment rates of people deemed to have the same level of health in an earlier year. If the former is lower than the latter, we conclude that there is ‘additional work capacity’ among the currently older population.
The measure of ‘health’ we use in this approach is the one-year mortality rate for people of a given age and sex. The strength of this measure of health is that it is readily available and defined in the same way for long time periods. A weakness is that this health measure may not be a particularly relevant one for determining whether or not someone is able to do paid work. It also assumes that the impact of health on work capacity has not varied over time.
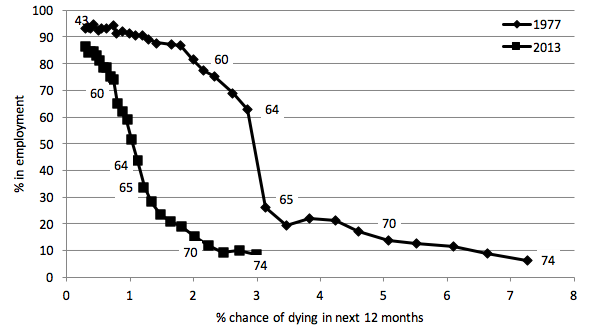
Figure 1 shows the relationship between one-year mortality rates (on the horizontal axis) and employment rates (on the vertical axis) for men at different points in time (shown by the two lines). Each of the marked dots corresponds to a different age group. The vertical gap between the lines shows that similarly-healthy men (as measured by their one-year mortality) had a much higher employment rate in 1977 than they did in 2013.
For example, men aged 64 in 2013 had a 1.1% chance of dying in the next year, which was similar to the probability of mortality for men aged 54 in 1977. But men aged 64 in 2013 had an employment rate of 44%, compared to 90% among men aged 54 in 1977. This suggests (perhaps) that men aged 64 in 2013 had additional work capacity of 46 percentage points.
Repeating this process for each age group from age 55 to age 74, we estimate that 86% of men aged 55–74 in 2013 had the capacity to work, based on their health. However, only 43% of them were working – suggesting that there was additional work capacity of around 43 percentage points. Carrying out a similar exercise for women we estimate that additional work capacity for women aged 55–74 was 12 percentage points.1
The estimated amount of additional work capacity calculated depends on which year we compare to. If we were to compare 2013 instead to a more recent year, we would conclude that there was a smaller amount of additional work capacity. However, whichever past year is chosen, we always conclude – using this method – that there is some additional work capacity. And the rate at which the work capacity changes according to the comparison year can be interpreted as the degree to which increases in work have failed to ‘keep up’ with increases in health. For men, work capacity has increased with each additional comparison year over the past thirty-five years, suggesting work continually fails to keep up with health improvements. In contrast, although earlier trends were similar, increases in work have broadly kept up with improvements in health since 2001 for women (see Figure 11 of Banks et al. 2016).
Figure 1. Relationship between one-year mortality rate and employment rate over time (men)
Notes: Each line shows the relationship between one-year mortality rate (on the horizontal axis) and employment rate (on the vertical axis) for men of different ages in 1977 and 2013. Each dot marked on the lines corresponds to a different age group.
Source: Figure 9 of Banks et al. 2016.
How much more do similarly healthy young people work?
A second approach (building on an estimation strategy suggested by Cutler et al. 2011) measures additional work capacity as the difference between the employment rate of older people and that of similarly healthy younger people observed at the same point in time. A strength of this approach is that we are able to include a rich set of indicators of health and disability that may impact on work capacity. This includes doctor diagnoses of numerous health conditions, difficulties with mobility and activities of daily living, depressive symptoms, smoking behaviour, and body mass index. A weakness is that it assumes any impacts of health on work capacity do not vary by age.
To construct a counterfactual employment rate for older people, we estimate the relationship (separately by sex) between a detailed set of measures of individuals’ health and their employment, among a sample of people in their early 50s. This estimated relationship between health and employment is then used to predict the work capacity of those aged 55–74, based on their health. In doing so, we are assuming that a given type of health condition affects capacity to work in the same way for (say) a 50 year-old man as for a 70 year-old man.
The health of the older group is on average worse than that of those in their early fifties. Therefore, predicted work capacity among those aged 55–74 (79% for men and 73% for women) is lower than that for those aged 50–54. However, it is still significantly above the employment rate actually observed among those aged 55–74 (44% and 34%, respectively). Among men aged 55–74 these estimates suggest additional work capacity of 35 percentage points. Among women aged 55–74 the estimates suggest additional work capacity of 39 percentage points.
Implications for policy
Both the methods we use suggest that there is significant additional work capacity at older ages among both men and women in the UK. For many, the lack of employment at older ages does not appear to be a consequence of poor health alone. Therefore, policymakers wanting to increase employment rates of older people should strive to tackle other barriers to employment. Of course, this is not to say that all those whose health means that they could work should work – some may well prefer to choose to retire.
But our estimates do suggest that there is a significant minority – never less than 14% – of those aged 55–74 for whom health does indeed limit their capacity to work. Therefore, as governments seek to raise pension ages further, they will need to ensure that adequate provisions are in place for those older people who are not able to support themselves financially in the absence of access to state-funded pensions.
Authors' note: This column was written when Gemma Tetlow was programme director of the IFS' work on pensions, saving and public finances.
References
Atalay, K and G Barrett (2015) “The impact of age pension eligibility on retirement and program dependence: Evidence from an Australian experiment”, The Review of Economics and Statistics, 97(1): 71–87.
Banks, J, C Emmerson and G Tetlow (2016) “Health capacity to work at older ages: Evidence from the United Kingdom”, NBER Working Paper No 21980.
Cribb, J, C Emmerson and G Tetlow (2013) “Incentives, shocks or signals: Labour supply effects of increasing the female state pension age in the UK”, IFS Working Paper, W13/03.
DWP (2010) When should the state pension age increase to 66?, UK Department for Work and Pensions.
DWP (2016) “State pension age independent review: terms of reference”, UK Department for Work and Pensions.
Mastrobuoni, G (2009) “Labor supply effects of the recent Social Security benefit cuts: Empirical estimates using cohort discontinuities”, Journal of Public Economics, 93(11–12): 1224–33.
Staubli, S and J Zweimüller (2013) “Does raising the early retirement age increase employment of older workers?”, Journal of Public Economics, 108: 17–32.
Endnotes
1 Since older women in earlier years were considerably less likely to work for reasons other than health this estimate is almost certainly an underestimate.