The Covid crisis has revealed the weaknesses of the US social system compared to European social systems: in particular its inability to offer adequate protection to individuals against the risk of falling sick or falling into poverty (Aghion et al. 2020). Moreover, it also brought to light the mismanagement of the pandemic by the current administration, as exemplified by negligence in realising the danger of the virus, pushing for excessively fast reopening of the economy, and resistance against mask wearing and generalised testing. Nonetheless, together with Congress, the same administration has pursued a determined and aggressive strategy to ensure US leadership in vaccine R&D and to secure supplies of future vaccines to US citizens.
Although the European Commission recently took the lead in negotiating advance purchase agreements with vaccine manufacturers on behalf of the 27 member states and decided to provide loans to European biotechs engaged in vaccine development through the European Investment Bank, it has fallen short in matching the US effort to incentivise vaccine innovation – not only because of a lower level of financial investment, but also an inability to ensure coordination across member states as well as across the different funding schemes for research and innovation in healthcare (reflecting the more decentralised nature of R&D and health policies in Europe).
This is problematic because the best way to get one’s economy back on track is to eliminate the virus. And, next to non-pharmaceutical measures (masks, social distancing, etc.), this means treatments and, first and foremost, vaccines. Naturally, a strategy that is too aggressive poses risks as well (e.g. conflict of interest from vaccine developers and reluctance in getting vaccinated).1
General considerations
Regarding Covid-19 vaccines, it is useful to distinguish two phases: vaccine development, and the securing of vaccine supplies once a vaccine has been found and authorised. Both are needed to bring vaccines to the patient (then one should still convince, or ‘force’, people to get vaccinated).
Intuitively, contributing to vaccine development looks like a ‘benevolent’ action, since the whole world should benefit from the arrival of one, or several, Covid vaccines. Instead, securing vaccine supplies in advance for one’s citizens seems more ‘selfish’, especially if limited supply means denying vaccines to other countries’ citizens. Nevertheless, advanced contracts for delivery will encourage private entities to energetically pursue vaccine development – the two are intertwined.
More generally, when considering innovation for a ‘global product’, it is natural to wonder about the ‘optimal’ degree of competition and coordination to rapidly identify successful vaccines. In fact, we observe an interesting mix of coordination and competition in the search for vaccines. Although political authorities in China were denying the upcoming disaster, Chinese scientists have been very open about their research results, which benefited the world research community. The first vaccines that will become available could be rapidly developed because Chinese scientists published the genetic sequence of the virus as soon as it was deciphered. On the other hand, universities and private firms, large and small, have been competing aggressively to ‘be the first’ in the race for a vaccine, including in terms of raising funds from private and state sources.
From the perspective of world welfare, the cooperation/open science part is of course good. As for the competition on vaccine development, things are more subtle: on the one hand, more financial effort overall is a good idea to accelerate innovation for such a costly disease (just think of the cost of a lockdown). On the other hand, should we worry about money ‘wasted’ in funding more than 100 vaccine projects, including advance building of production facilities? As discussed by Bolton-Farrell (1990), in “times of war”, speed is essential, and more coordination is preferable to “fine-tuning for the most efficient option” if such an optimal solution comes later. We can, however, safely conclude that speed will not be hampered, given the rush we observe (if anything, the risk is more about ‘cutting corners’ in excessively fast approval of vaccines which might not be safe and effective enough).
The US versus the EU
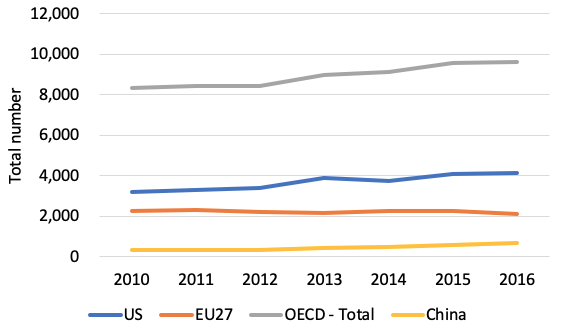
The US is a clear leader in biotech innovation (Figure 1 and Table 1). Moreover, it does have an articulated US-centric Covid strategy – Operation Warp Speed (OWS) – which builds on an understanding of the complementarity between vaccine development and securing advanced supplies, thereby bringing together the negotiations with private entities on the two phases, while relying on the combined expertise and financial weight of existing federal instruments, in particular the National Institutes of Health (NIH) and the Biomedical Advanced Research and Development Authority (BARDA). This gives the US a first-mover advantage.
Figure 1 Biotechnology patents
Source: Authors’ calculations using OECD data. Reference country: Inventor’s country of residence. Reference date: priority date.
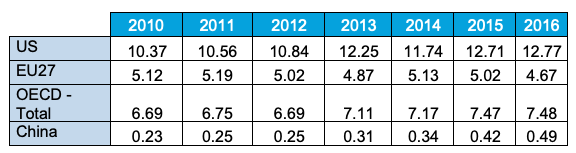
Table 1 Biotechnology patents (per 1 million inhabitants)
Source: Authors’ calculations using OECD data.
Notes: Reference country: Inventor’s country of residence. Reference date: priority date.
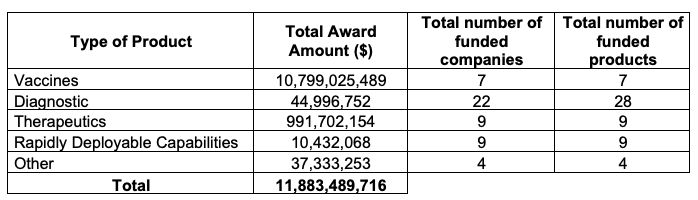
Congress has allocated almost $10 billion to OWS, of which more than $6.5 billion was allocated to BARDA and $3 billion for NIH research. In practice, during this pandemic, BARDA is providing funding to develop, among others, vaccines and treatments to fight Covid. So far, BARDA has distributed more than $11 billion among more than 40 companies to fund the development of vaccines, diagnostic, therapeutics, rapidly deployable capabilities, and others (Table 2).2
Table 2 BARDA’s Covid-19 medical countermeasure portfolio
Source: Authors’ calculations based on https://medicalcountermeasures.gov/app/barda/coronavirus/COVID19.aspx.
The EU, instead, has pursued a less coherent strategy overall, and with fewer financial resources directly invested in candidate vaccines (European Commission 2020). Indeed, it is more ‘benevolent’ than the US in terms of vaccine development, pushing for worldwide cooperation, but with limited funding commitment (Tables 3 and 4). In fact, the EU makes constant international cooperation efforts, as the Coronavirus Global Response exemplifies. This global action raised almost €16 billion from countries worldwide; the US did not contribute. The EU also contributes through the Coalition for Epidemic Preparedness Innovations (CEPI),3 an innovative partnership between public, private, civil and philanthropic organisations. Additionally, the ACT-Accelerator has one vaccine pillar, COVAX, of which CEPI is co-leader together with Gavi and WHO. However, in spite of these international cooperation efforts, the EU is ‘EU-centric’ when trying to secure vaccine supplies for its member states and citizens. This does not sufficiently exploit the complementarity involved in the process, which adds to the problematic complexity of funding sources (within the European budget, EIB, member states, etc).
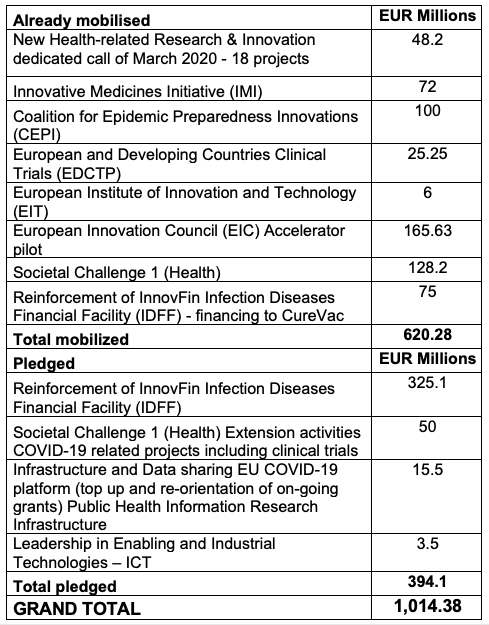
Table 3 Coronavirus global response: Horizon 2020 pledge
Source: https://ec.europa.eu/info/research-and-innovation/research-area/health-research-and-innovation/coronavirus-research-and-innovation/financing-innovation_en, last access 24 August 2020.
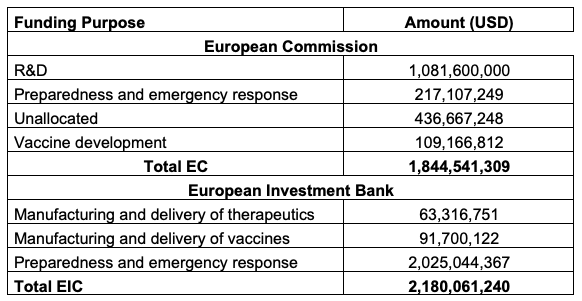
Table 4 Funding from the European Commission and the European Investment Bank
Source: Authors’ calculations using data from the COVID-19 Health Funding Tracker, from The Economist.
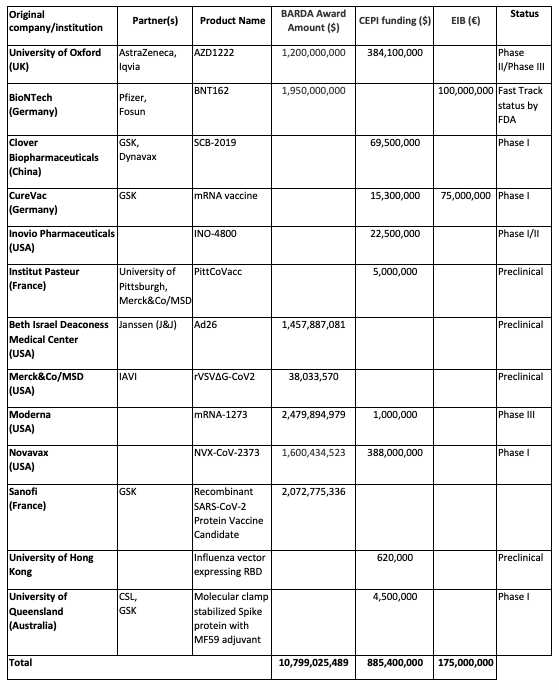
Currently, there are more than 130 candidate vaccines in preclinical evaluation and 30 candidate vaccines in clinical evaluation. Among these 30 candidates, 13 receive support from BARDA, CEPI and/or the EU/EIB (Table 5). Three receive support from both BARDA and CEPI (University of Oxford, Moderna and Novavax), one receives support from both CEPI and the EIB (CureVac), and one from BARDA and EIB (BioNTech). BARDA provides consistently higher funding amounts.
Table 5 Partnerships to develop vaccines against Covid-19: BARDA, CEPI and EU (through EIB)
Source: Authors’ calculations based on BARDA, CEPI and Global Response Europe.
A renewed EU support strategy to the development and commercialisation of innovative technologies could be extended to other areas, for example, defence-related technologies, on the model of the Defense Advanced Research Projects Agency (DARPA) in the US. Interestingly, the latter has been instrumental in a number of non-defence innovations as well. Note that we are not talking here about a renewed industrial policy amounting to ‘picking one winner’ but funding several competing vaccines. The DARPA model is one that mixes top-down and bottom-up: government funds are devoted to financing competing teams that work on making new ‘tough technologies’ become operational. Once selected by the government, team leaders have full autonomy in deciding on how to organise the research process and whom to involve in that process. The various teams will typically compete not only within Europe, but also on a more global scale, with the US, but also China and possibly Russia. So, this is about competition-friendly industrial policy, as advocated in Aghion et al. (2015).
How would a European BARDA work? While there are a number of institutional specifications to address, let us just make two remarks. First, this is an area where joining forces with Britain makes sense, given its (academic and industrial) expertise (the same is true for defence). Second, one wants of course to identify the optimal trade-off between scale and adaptiveness/flexibility, since speed is often key. This would plead for an open ‘coalition of the willing’, which can possibly build on insights from EU success stories (like the European Research Council, which includes non-EU partners) but should clearly avoid rigidities (e.g. juste retour, seven-year budgets) enforced by (near) unanimity voting rules.
Competition between Europe and the US would accelerate vaccine development and supply, which can be good for the world as a whole. Naturally, ‘pressure’ on pharmaceutical companies to avoid excessive profits, as well as sufficient international (public and private) aid to ensure global access, will be very important.
To sum up, in order to strengthen European industries leadership in vaccine research and innovation, we recommend the creation of a European BARDA to which EU member-states plus the UK would be welcome to participate on a voluntary basis. Although the BARDA model should be adapted to ensure a decision process that is science-based and transparent, we suggest that the launch of a BARDA-type initiative should be considered in the forthcoming Horizon Europe framework programme for Research and Innovation. The strategy we suggest would be complementary to Europe’s other assets when facing epidemiological shocks, namely an evidence-based sanitary policy and a social model that can mitigate such shocks.
References
Aghion, P, J Cai, M Dewatripont, L Du, A Harrison and P Legros (2015), “Industrial Policy and Competition”, American Economic Journal: Macroeconomics 7: 1-32.
Aghion, P, H Maghin and A Sapir (2020), “Covid and the nature of capitalism”, VoxEU.org, 25 June.
Bolton, P and J Farrell (1990), “Decentralization, Duplication and Delay,” Journal of Political Economy 98: 803-826.
New York Times (2020a), “Corporate Insiders Pocket $1 Billion in Rush for Coronavirus Vaccine“, 25 July.
New York Times (2020b), “Scientists Worry About Political Influence Over Coronavirus Vaccine Project“, 2 August.
European Commission (2020), “EU Strategy for COVID-19 vaccines”, 17 June.
U.S. Department of Health and Human Services (2020), “Explaining Operation Warp Speed”.
Endnotes
1 Vaccine developers have a conflict of interest since more optimistic announcements help them attract more funding for vaccine development and advance production facilities or, worse, opportunities to cash in on optimally timed stock sales (New York Times 2020a). Another risk is that this strategy might lead to reluctance in getting vaccinated against Covid, adding to the vaccine hesitancy problem which is already high in the US (New York Times 2020b).
2 Operation Warp Speed also coordinates other initiatives such as the NIH’s Accelerating COVID-19 Therapeutic Interventions and Vaccines (ACTIV) public-private partnership (of which the European Medicines Agency is also a partner) and the NIH’s Rapid Acceleration of Diagnostics (RADx) initiative.
3 From a total of $1,280,588,290 for vaccine development for CEPI, the European Commission contributed with $109.2 million. The top contributors are the UK ($270 million), Norway ($213.5 million), Germany ($160.4 million), Saudi Arabia ($150 million) and Japan ($134 million), followed by the European Commission (source: The Covid-19 Health Funding Tracker from The Economist).