Many countries around the world are currently implementing a lockdown (or considering it) of most economic activities to contain the spread of the COVID-19 epidemic. In the countries that have put one in place, the debate is now turning to when and how to get out of the lockdown, so the economy can restart. In this column, I use basic economic principles to think about the trade-offs involved – a ‘Lockdown 101’ discussion.
The main takeaways of my analysis are:
- At the peak of a serious epidemic, a near-full lockdown is better than nothing in unprepared countries. However, the lockdown should not be long-lasting, with its duration being determined by its marginal (health) benefits and (economic) costs.
- Activities to be suspended in the lockdown should be ordered from those that yield higher health benefits and impose lower economic costs to those that have the opposite effect; in serious cases, as with COVID-19, initially a large number of activities will need to be suspended in unprepared countries.
- The optimal extent of lockdown measures changes over time and eventually decreases, but does not drop to zero quickly.
- Better health measures to cope with the epidemic allow for more lenient lockdown policies.
- Measures that ease the economic pain during the lockdown pave the way for stricter lockdown policies.
- The economic and health costs of the epidemic will be much higher for developing economies than for rich ones, even though it is generally ambiguous which should have stricter lockdown policies.
The desirability of a full lockdown
On the one hand, a lockdown brings health benefits for the society as it contains the spread of the virus, reducing the number of infections and allowing the health system to treat those infected (as well as those that require health services unrelated to the epidemic) better. On the other hand, a lockdown hurts the economy, because it prevents mutually beneficial economic activities that would otherwise take place.
If the question were simply whether a government should implement a lockdown or not, we would need to compare the benefits and costs. Importantly, these change over time. At the peak of an epidemic, stopping human interaction has a very large health benefit, as it halts contagion (completely, in the case of a perfect enforcement) and prevents additional pressure on an overloaded heath system. After the lockdown is in place for a while, however, these benefits fall as the health situation becomes more manageable.1 That is, the marginal health benefit (MHB) of a lockdown decreases with its duration.
At the same time, the economic cost of a lockdown increases over time. As Baldwin (2020) puts it, we are used to having (partial) lockdowns during weekends and national holidays, but those have little cost because we know they last just a few days. However, maintaining a lockdown for a longer period imposes increasing costs on society, as firms go bankrupt, individuals are laid off and, ultimately, consumption levels (and welfare) drop sharply and continuously. That is, the marginal economic cost (MEC) of a lockdown increases with its duration.
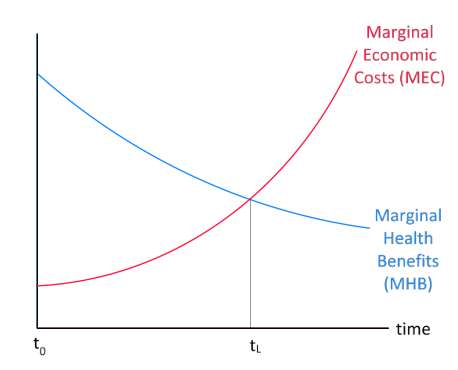
Figure 1 illustrates this point. During regular times, MHB < MEC at t0, and therefore nobody discusses lockdowns. However, at the peak of an epidemic for which countries were ill-prepared to handle, as now with covid-19, MHB > MEC at t0, so implementing a lockdown (L) is initially better than not implementing it. That changes with time, however, as the health situation becomes more manageable and the economic situation more costly. Eventually (period tL in the figure), it becomes better to lift the lockdown and restore economic activities.2
Figure 1 Optimal duration of a full-lockdown policy
My first conclusion is therefore very simple: at the peak of an epidemic, a full (or near-full) lockdown is better than nothing in countries that were unprepared for it. However, the lockdown should not be long-lasting, and its duration should be determined by its marginal (health) benefits and (economic) costs.
This is, however, too simplistic, because it presents the problem as dichotomous: either have a lockdown or don’t. As with the vast majority of public policies, the optimal policy is often interior, not at the corner.
The optimal level of lockdown over time
Let us consider, then, the possibility of partial lockdowns. That is, consider a variable l that goes from 0 (no restrictions on economic activities, as in, say, 2019) to L (full lockdown, where people do not interact with each other outside their homes and almost all economic activities stop). Then, instead of considering the benefits and costs of a full lockdown over time, let us consider the benefits of costs of different degrees of lockdowns at specific points in time.
When l is very close to zero, the health benefits from increasing l are greatest, because it would have the greatest impact on reducing contagion. Once l gets very close to L, however, the additional health benefits from increasing l are small, as there are already very few people interacting with each other and the virus is spreading at a very low rate. Hence, the MHB decreases with l.
Conversely, when l is very close to zero, the economic costs of increasing l are small, because it will not disrupt any key activity. However, as l gets very close to L, the additional economic costs from increasing l are huge, because some essential economic activities will need to be shut. Hence, the MEC increases with l.
Implicit in the discussion above about how the MHB and MEC change with l is the assumption that there is an optimal order for activities as l moves from 0 to L. This is key: a progressive lockdown must first affect the activities that generate least economic costs and most health benefits. Obviously, designing a perfect ordering is a daunting activity, especially because societies have very little experience in doing this. Nevertheless, it is relatively easy to place several activities near the two extremes.
For example, office work that can be carried out online should be one of the first, because it imposes very small economic costs and generates some health benefit as people do not mingle in the office. Large sports events would also be one of the first, because preventing them generates large health benefits, even if the economic costs are not negligible. Moreover, the activities involving those in the risk group (for COVID-19, the elderly and those with co-morbidities) should be the first to be averted. Near the other extreme we should have activities for which their prohibition would cause large economic costs and small health benefits (e.g. trash collection, news provision, grocery stores and, most obviously, health services, which would cause a negative MHB).
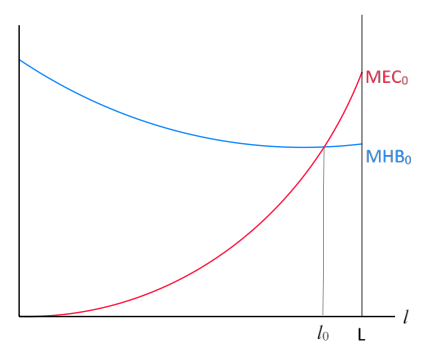
Figure 2 illustrates this discussion at the peak of the epidemic crisis. At that moment, the case for an almost-complete lockdown is strong, in line with what the previous dichotomous analysis suggests. Even then, a full lockdown would not be optimal, as we want to keep essential services and production of essential products (food, medicines) active. However, the optimal l is probably fairly high initially, as the figure indicates (l0).
My second conclusion is therefore also very simple: the activities to be suspended should be ordered from those that yield higher health benefits and impose lower economic costs to those that have the opposite effect; the optimal level of lockdown then equalises marginal health benefit to marginal economic cost.
Figure 2 Optimal lockdown policy tends to be severe at the peak of the pandemic
Typically, the solution will be interior during an epidemic, reflecting the suspension of some activities. When an epidemic is very serious and governments were unprepared to deal with it, as with COVID-19, initially a large number of activities will need to be suspended, including some that cause significant economic harm.
Now, as l0 remains in place for a while, the curves change, as suggested by Figure 1. In particular, the MEC curve will shift up for any level of l. At the same time, as the epidemic is better controlled, the MHB curve should shift down. However, in its early stages that curve could be going up for ‘exogenous’ reasons – that is, either following the contagion dynamics of the epidemic or because the health system is collapsing and dramatically needs some relief.
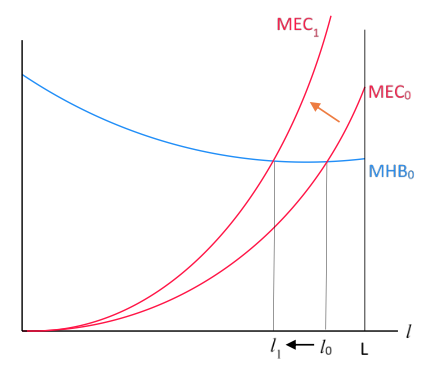
Figure 3 illustrates those changes. For the sake of clarity, it simply assumes that l0 is such that it just offsets those exogenous forces at first, so that the MHB remains unchanged in the next period. In that case, because of the shift in the MEC curve, the new level of the optimal l, l1, is lower than l0. That is, because economic costs increase over time, restrictions on economic activity should be relaxed somewhat (say, some retailing stores employing low-income workers may be allowed to reopen).
This does not need to be the case. If the exogenous dynamics of the epidemic is such that the MHB curve moves up very quickly, the optimal policy may be an even stricter lockdown in period 1 than in period 0. However, epidemics eventually run their courses and come to an end, even if left untreated. Thus, the MHB curve will eventually shift down, and the more severe the initial lockdown, the more quickly this will happen. This implies that the optimal l will eventually fall, with economic restrictions being lifted.
Nevertheless, it will typically take time to bring l back to zero. This reinforces the point that the solution is not dichotomous. Suspension of some economic activities is optimal until the epidemic is completely controlled. And the optimal time-path is typically smooth and long-lasting, with restrictions being lifted over time.
This also has implications for the dynamics of the epidemic: the goal of the restrictions on economic (and social) activities is not to eliminate the epidemic quickly, but to keep its health costs aligned with the economic costs of the restrictions. Thus, increases in cases, as has recently happened in some Asian countries that appeared to have the epidemic under control, are not a reason to think that ‘their system is not working’. Instead, that is a consequence of an optimal monitoring of the epidemic, which should not aim to eliminate it at once.
Figure 3 Optimal lockdown policy becomes more lenient over time
My third conclusion is, therefore, more subtle: the optimal extent of lockdown changes over time and eventually decreases, but does not drop to zero quickly. Instead, it manages the health–economics trade-off over time.
A caveat is in order here. The problem is inherently dynamic, since the position of the two curves in a point in time depends on the policy of the previous period. What Figures 2 and 3 do, by illustrating different points in time, is mimic those dynamics. It is obviously incomplete and inaccurate, but hopefully enough to drive home the qualitative message that a truly dynamic model would deliver.
Finally, let me make some additional key observations on the levels of the MHB and MEC curves. First, on the policies that affect the two curves. And second, on the characteristics of an economy that affect the two curves.
Policies that keep the MHB and MEC curves low
Rightly so, much of the current debate is about the best health policies to contain the spread of the epidemic and prevent collapses in health systems. These include keeping vulnerable people isolated, widespread testing and subsequent monitoring, with isolation also of those who test positive and of their contacts (and of the contacts of their contacts), building of hospital beds, production of medical equipment to treat the ill, and so on. Despite the direct economic costs of such measures, they pale next to the economic costs of lockdowns.
In my setup, health measures to contain the spread of the virus and better prepare the health system to cope with the ill can be interpreted as policies that push the MHB curve down. Clearly, if the MHB curve shifts down, it will, at any point in time, reduce the severity of the optimal lockdown. Thus, not only will the measures bring about a direct health benefit, they also allow for an indirect economic benefit by permitting a more lenient lockdown policy (and yes, they also require a direct economic cost to be put in place).
Thus, my fourth conclusion is that better health measures to fight the epidemic allow for a more lenient lockdown policy, therefore curbing their economic costs.
The part of the of the current debate that is not on health policies is on the best economic policies during the crisis. Most go in the direction of, in the words of Baldwin and Weder di Mauro (2020a), “keeping the lights on” until the epidemic is controlled. This include policies to preserve employment, to avoid bankruptcies, to expand credit to firms and consumers, and so on.3 Typically, they aim to (1) prevent current disruptions in the economic system from becoming permanent, and to (2) mitigate the welfare cost to the most vulnerable ones.
In my setup, those policies can be interpreted as measures that push down the MEC curve, as they make a lockdown less painful in the short run and lower its long-run deleterious effects. Clearly, if the MEC curve shifts down, it will, at any point in time, increase the severity of the optimal lockdown. Thus, by easing their costs, those policies allow for stricter lockdowns, which will help contain the epidemic more quickly and effectively (and yes, they also require a direct economic cost to be put in place).
Thus, my fifth conclusion is that measures that ease the economic pain during the fight against the epidemic pave the way for stricter lockdown policies, thus bringing larger health benefits.
Country characteristics that affect the MHB and MEC curves
The MEC and MHB curves vary significantly across regions/countries depending on their socioeconomic characteristics.
Starting with the MHB curve, it can be very different depending on cultural traits and the demographics of the country, even for a given stage of the epidemic. For example, if it is common for different generations to live together, or if the elderly share of the population is high, then the MHB curve will be relatively high – compare, say, Italy with Germany. This implies that, for otherwise similar countries in terms of development, one with a high share of elderly who tend to live with younger relatives (Italy) will need stricter lockdown policies than another with the opposite characteristics (Germany).
Probably even more critical is the structure of the health system of the country. So far much of the focus remains on rich countries, which have relatively solid health systems in place. In developing countries, however, much less strain to the system is required to make it collapse. Therefore, the MHB curve tends to be much higher in developing economies than in rich ones. That, in itself, would push for stricter lockdown policies.
We must also look, however, look at how levels of development affect the MEC curve. It will be relatively low where individuals have access to liquid savings and the government can, directly and indirectly (through incentives for the private sector), keep incomes and payments flowing, limiting bankruptcies and layoffs during the peak of the crisis. On the other hand, in countries where few households have savings, the informal sector (which tends to be more affected) is large, and the government is unable to provide much help to keep incomes and payments flowing, the MEC will be much higher.
Taken together, we have that both curves will be higher in developing countries. The impact on the optimal lockdown policy is therefore ambiguous. It will depend on how good/bad the health system is relative to the economic system. In places where the health system is better equipped to cope with the epidemic than the economic system is to cope with the restriction of activities, a more lenient lockdown would be advisable. The opposite would be true otherwise.
Now, what is clear is that, for developing countries, both the economic and health costs of the epidemic will much higher than for rich countries. The curves will intersect at a higher level both because the economy is ill-suited to sustain a lockdown and because the health system is ill-suited to deal with an epidemic. The optimal lockdown policy trades off those two costs optimally, but the outcome is nevertheless dire. The drama we have seen in Europe and in the US may be dwarfed by what is about to happen in poorer countries affected by the epidemic.
Thus, my sixth and final conclusion is that it is generally ambiguous whether the optimal lockdown policy should be stricter in rich or in developing economies. But it is unambiguous that the latter will suffer more, economically and health-wise, with the pandemic.
Conclusions
The debate about the desirability of an economic lockdown to deal with the covid-19 pandemic is often dichotomic: have it or not. That is misleading. The optimal lockdown policy is very likely an intermediate one. For countries caught off guard with the current epidemic (with is most countries, except for some in Asia), a severe form of lockdown is optimal when the epidemic takes hold of the country. After an initial period, that policy should become more lenient, but should remain in place for as long as the epidemic poses a threat to the health system, although in increasingly milder forms. That is, a return to the 2019 level of economic freedom will probably take several months. The last restrictions to be lifted should be on the activities that cause little harm if performed remotely and those that would cause most harm by allowing a wider spread of the virus.
Importantly, the level of the lockdown, its duration, and the underlying economic and health costs depend critically on the measures that improve the capacity of the health system to cope with the epidemic (testing, isolating the vulnerable, etc.) and the capacity of the economic system to navigate through a period of suspended economic activities without compromising its structure. Naturally, to provide precise answers to those questions we need a quantitative model, as in Atkeson (2020) or Eichenbaum et al. (2020), for example. Nevertheless, my qualitative conclusions may be useful as a guideline for future models and, more importantly, for current policymakers that need to make decisions before those models are fully developed.
Author’s note: I want to thank, without implicating, several colleagues for interesting, lively discussions on the topic and useful suggestions for this column.
References
Atkeson, A (2020), “What will be the economic impact of COVID-19 in the US? Rough estimates of disease scenarios.” Mimeo.
Baldwin, R (2020), “The supply side matters: Guns versus butter, COVID-style”, VoxEU.org, 22 March.
Baldwin, R and B Weder di Mauro (2020a), “Introduction,” in Baldwin, R and B Weder di Mauro (eds.), Economics in the Time of COVID-19, a VoxEU.org eBook, CEPR Press.
Baldwin, R and B Weder di Mauro (eds) (2020b), Economics in the Time of COVID-19, a VoxEU.org eBook, CEPR Press.
Eichenbaum, M, S Rebelo and M Trabandt (2020), “The macroeconomics of epidemics.” Mimeo.
Hall, R and C Jones (2007). “The Value of Life and the Rise in Health Spending”, Quarterly Journal of Economics 122(1): 39-72.
Endnotes
1 A large literature calculates the statistical value of a life (e.g. Hall and Jones 2007).
2 Enforcement of a lockdown is also likely to decrease with its duration. This tends to lower both its economic costs and its health benefits, with an ambiguous effect on its optimal duration.
3 See the collection of articles in Baldwin and Weder di Mauro (2020b) for a variety of such proposals.
4 Here I am neglecting the possibility that a warmer climate may make the COVID-19 epidemic weaker, since that is yet unproved. If so, the MHB curve for developing countries with warmer temperatures would be lower, implying weaker lockdown policies and lower overall health and economic costs.