There is growing interest among governments in leveraging private insurers to improve the efficiency and quality of the healthcare system. In Israel, Switzerland, and the Netherlands, for example, universal healthcare is already delivered by private insurers regulated by the government. In almost all other EU countries, private insurance operates alongside the statutory coverage, offering additional benefits and enhanced service quality.
Through the adoption of the Affordable Care Act, the US has expanded insurance through subsidised private insurance and implemented pay-for-performance (known as ‘P4P’) in insurance markets. As health spending continues to rise globally, pay-for-performance can be an attractive policy tool for promoting high-quality services at lower costs (Accenture 2012). By linking payments to service quality, pay-for-performance can increase the cost-effectiveness of health spending and encourage investments in quality.
Improved service quality, however, is not equally accessible to all consumers. In the healthcare sector, there are concerns that pay-for-performance weakens the finances of poor-performing hospitals in low-income areas, ultimately hurting the quality of care to minority and indigent patients (Karve et al. 2008, Joynt et al. 2011).
This efficiency-equity trade-off is of particular interest in health insurance markets, where the selection of healthy enrollees has been documented across contexts and already is a critical issue for access to care. In Germany, for example, insurers discriminate on the geography of insurance applicants to select low-cost enrollees (Bauhoff 2012). Policy attempts to counter the selection incentives have not been fruitful. Linking payments to the predicted costs of enrollees did not eliminate selection: insurers responded by favouring enrollees cheaper than their predicted costs (Brown et al. 2014) and by top-coding diagnoses to inflate the cost prediction (Geruso and Layton 2018).
In recent work (Fioretti and Wang 2019), we present the first evidence on the efficiency and equity consequences of pay-for-performance in private insurance. Drawing from the introduction of pay-for-performance in US Medicare – the health insurance programme for those above the age of 65 – we examine how insurers respond to the payment incentives and the effect of insurer responses on insurance quality and consumer access.
We found that after the payment reform, high-quality insurers selected healthier enrollees by transferring insurance benefits from sicker to healthier enrollees, but the reform did not improve financial protection or the health outcomes of an average enrollee. The selection practices shifted the distribution of high-quality insurance to the healthiest counties, worsening the regional disparities in healthcare access. Sicker enrollees in the riskiest counties were most hurt by the payment reform.
Payment reform in Medicare Advantage
Medicare beneficiaries can opt in to the private version of Medicare called Medicare Advantage, where Medicare services are contracted out to private insurers. Since 2009, insurers receive a quality rating – from 2 to 5 stars – based on enrollee health outcomes, customer service, and managed care processes. The outcome measures focus on chronic conditions such as diabetes and hypertension and constitute half of the overall rating. Enrollees compare the quality rating in addition to premiums and benefits at the time of enrolment.
Subsidies to insurers were linked to their quality rating in 2012. The financial incentives are intended to increase investments in quality and to focus health spending on high-value services with better benefits to enrollees. However, difficulty with measuring service quality can result in misaligned incentives. If patients with more severe conditions tend to lower the quality rating, avoiding sicker patients could be profitable (Dranove 2003). In this case, bonus payments could incentivise selection activities rather than actual improvements in quality.
We distinguish contracts by pre-reform quality ratings and document the selection responses to bonus payments and the consequences of selection based on a difference-in-differences design.
Main findings
We establish three main findings. First, high-quality insurance contracts improved the risk pool of enrollees after the payment reform. Figure 1 compares the distribution of risk scores before and after the policy.
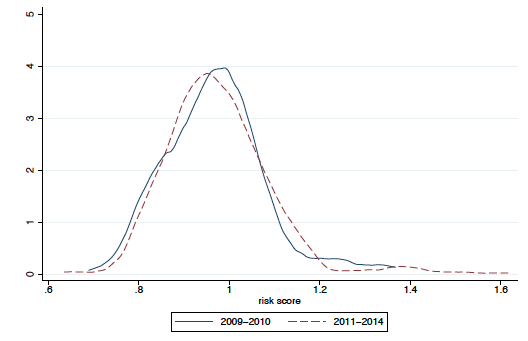
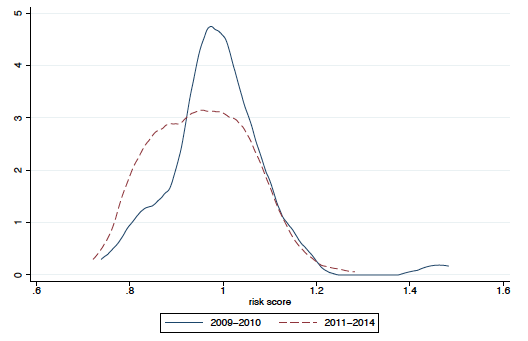
Figure 1 Density of risk scores in high- and low-quality insurance, before (2009-2010) and after (2011-2014) payment reform
a) Low-quality insurance
b) High-quality insurance
Notes: Risk scores shifted to the lower percentiles in high-quality insurance, but not in low-quality insurance.
In high-quality contracts, risk scores decreased significantly in the lower percentiles (panel b). We do not see similar changes in low-quality contracts (panel a). Among high-quality contracts, the drop in risk score is concentrated in those already serving healthier populations before the payment reform.
Second, high-quality insurers selected healthier enrollees by lowering premiums in healthier counties and by increasing premiums by a similar amount in riskier counties. Figure 2 shows the premium differences for prescription drug coverage across counties with different population risk.
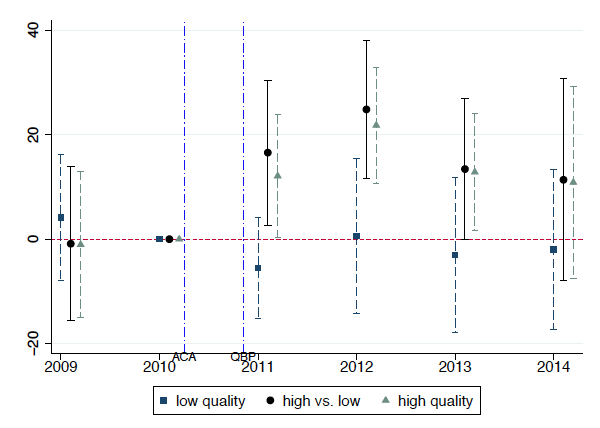
Figure 2 Premium differences across county risk scores by insurance quality
Notes: The dotted lines on the left plot the premium differences for prescription drug coverage across county risk scores in low-quality insurance. The dotted lines on the right plot the premium differences across county risk scores in high-quality insurance. The solid lines in between plot the differential change in high-quality premiums across county risk scores. We focus on counties in the lower and upper 15% risk tails of an insurance contract’s service area.
For low-quality insurance, premium differences did not increase after the payment reform. High-quality insurers, in contrast, raised premiums significantly in the riskiest counties covered by the insurance. For an average enrollee, however, insurance benefits (premiums) did not increase (decrease) more in high-quality insurance. This implies that high-quality insurers selected healthier individuals by shifting benefits from sicker to healthier enrollees. As the supply of high-quality insurance shifted to the healthiest counties, access to high-quality insurance decreased in the riskiest counties.
Third, we use premium differences to correct for the risk-composition change in high-quality insurance and quantify the extent of selection in the quality measures and bonus payments. Selection explains over 70% of the health-rating gains of high-quality insurers. Adjusted for risk, health outcomes did not improve more for high-quality insurance. We calculate risk-adjusted bonus payments by removing the selection gains on the quality rating.
Figure 3 shows the changes in bonus payments by the initial star rating. Among selecting insurers, around 15% of the bonus payments rewarded selection rather than quality. For marginally high-quality insurers (3.5–4.0 stars), selection kept insurers eligible for higher bonus rates and inflated bonus payouts by over 30%.
Figure 3 Effect of selection on bonus payments
Notes: The figure plots the changes in bonus payments after removing the selection gains on the quality rating. We show changes by the initial star rating of insurance plans, both for an average plan receiving the star rating (unweighted) and an average enrollee in those plans (weighted). We focus on high-quality insurance already serving healthy counties prior to the reform.
Several aspects of the quality rating contribute to the selection responses. Among all sub-measures forming the final quality rating, health-outcome measures are the most heavily weighted, accounting for 50% of the final rating linked to payments. The financial return to gaming these measures is high. Most health-outcome measures concern the management of chronic conditions such as diabetes and hypertension and reward insurers based on the percent of patients testing below certain medical thresholds. These measures are sensitive to the case-mix of health conditions. We show that selecting healthier enrollees improved health measures but not the actual health of enrollees. Correcting for selected risk types can more accurately reflect insurance quality, encourage investments in quality, and allow for broader access to high-quality insurance.
Lessons for policy
We draw two general lessons for policy from our analysis. First, ratings of service quality are endogenous to the consumer types serviced by firms. Bias due to the selected consumer base can lead to inefficient spending on low-value services. In value-based purchases in healthcare, given the focus on health outcomes as a key element of service value, adjusting for differences in the case-mix of health conditions is critical for the success of the payment model.
Second, policy efforts to improve the quality of social services can have unintended consequences on access. Performance-based incentives particularly hurt the vulnerable population more in need of high-quality services. Similar concerns emerge in the allocation of research (Stern 2016) and education resources (Chetty and Friedman 2011), where the payment system tends to worsen the inequality in public funding. Both efficiency and equity implications should be carefully considered to get pay-for-performance to perform.
References
Accenture (2012), “Delivering public service for the future: Navigating the shifts”.
Bauhoff, S (2012), “Do health plans risk-select? An audit study on Germany’s social health insurance”, Journal of Public Economics 96(9-10): 750–9.
Brown, J, M Duggan, I Kuziemko and W Woolston (2014), “How does risk selection respond to risk adjustment? New evidence from the Medicare Advantage program”, American Economic Review 104 (10): 3335–64.
Chetty, R, and J N Friedman (2011), “Does local tax financing of public schools perpetuate inequality?”, National Tax Association Proceedings, 103rd Annual Conference on Taxation, 112–18.
Dranove, D, D Kessler, M McClellan and M Satterthwaite (2003), “Is more information better? The effects of ‘report cards’ on health care providers”, Journal of Political Economy 111(3): 555–88.
Fioretti, M, and H Wang (2019), “Subsidizing inequality: Performance pay and risk selection in Medicare”, Sciences Po Economics Discussion Paper 2019-15.
Geruso, M, and T Layton (2015), “Upcoding: Evidence from Medicare on squishy risk adjustment”, NBER Working Paper w21222.
Joynt, K E, and A K Jha (2011), “Who has higher readmission rates for heart failure, and why? Implications for efforts to improve care using financial incentives”, Circulation: Cardiovascular Quality and Outcomes 4(1): 53–9.
Karve, A M, F-S Ou, B L Lytle and E D Peterson (2008), “Potential unintended financial consequences of pay-for-performance on the quality of care for minority patients”, American Heart Journal 155(3): 571–6.
Stern, N (2016), “Building on success and learning from experience: An independent review of the Research Excellence Framework”.