Communicable diseases have been an unwelcome companion of humanity throughout history, with epidemic outbreaks at times threatening its very existence. Accordingly, societies have experimented with different mitigation measures to stem the spread of diseases: from the quarantines of medieval Venice against the plague (Centers for Disease Control 2020) to the cordons sanitaires of 1821, designed to stop yellow fever from spreading from Spain to France.
When regions are connected, behaviour and policy in any one territory are influenced by other connected territories, either because of physical proximity or because people commute or move from one region to the other. Holtz et al. (2020) quantify this type of interdependence in the US: they find that behaviour and policy in a given state are affected significantly by changes in policy in other states.
In recent times, it has been recognised that spontaneous behaviour change and policy interventions that modify behaviour interact in a two-way fashion with disease dynamics. This recognition has ushered in a new era of formal analysis and policy design to rationally manage epidemic outbreaks (Giannitsarou and Toxvaerd 2020).
Research in this field is built on two central premises. First, it recognises that people’s behaviour – what they do and don’t do – influences how diseases spread and that the presence of disease in the population also influences people’s incentives to change behaviour.
Second, an optimal policy must explicitly account for how different interventions influence the spread of the disease in the future; policy cannot be simply adaptive but must recognise the trade-offs inherent in changing the path of the epidemic. As a result, we now better understand how to manage diseases over time, tailoring mitigation measures to different stages of the epidemic and accounting for the costs and benefits of different interventions.
Yet despite this progress, fundamental aspects of disease management remain relatively unexplored – for infections must be managed not just over time but also within and across regions and countries. In other words, disease dynamics are spatio-temporal in nature and policy must therefore grapple with how best to control epidemic outbreaks as they spread across territories and between regions and countries.
This raises a new set of questions that speak directly to optimal policy design but which have, until recently, been treated only implicitly by policymakers. There are three questions that the policymaker must consider when designing optimal mitigation measures:
- What are the effects of geographical integration on disease dynamics and what is the value of segregating territories through measures such as travel restrictions?
- How important is it to coordinate policy across jurisdictions, such as different states or neighbouring countries?
- How important is it to target mitigation policies to local geographical conditions?
These questions are of direct and immediate policy relevance. In the EU, national governments formulate policies independently, although they are often closely interconnected either through shared borders or mutual travel flows (Burlig et al. 2021). In the UK, health policy is delegated to the devolved administrations; for example, Scotland and England each implement their own measures (Hallas et al. 2020). Last, in the US, lockdown measures are determined at the state level and, in some instances, even at the sub-state level (see Tatlow et al. 2021 and Crucini and O’Flaherty 2021).
This type of delegation creates the potential for mis-coordinating policies across interdependent territories, perhaps most clearly seen at the national level. The recent report of the Lancet COVID-19 Commission concluded that
Coordination among governments was inadequate on policies to contain the pandemic, including travel protocols to slow the global transmission of the virus [and] public health and social measures ..., despite the very high interdependence among countries (Sachs et al. 2022).
Within jurisdictions, geographical targeting of policies becomes pertinent. For example, the UK operated a tier system at the local authority level (Department of Health and Social Care 2020), whereby those regions with particularly high COVID-19 prevalence were singled out for stricter mitigation measures (UK Cabinet Office 2020). Germany’s policy of ‘hotspot regulation’ was similar in nature (Deutschland.de 2022).
The value of geographically targeting COVID-19 mitigation measures was studied by Wrigley-Field et al. (2021) in the context of vaccination (see also Long et al. 2021 for a study of the effects of geographically targeted lockdowns on inter-region mobility patterns).
How then should policymakers address such issues when designing and implementing mitigation measures? In recent research (Hoover and Toxvaerd 2022), we consider these questions in a fully integrated economic-epidemic model of disease dynamics that can be controlled through regional lockdowns.
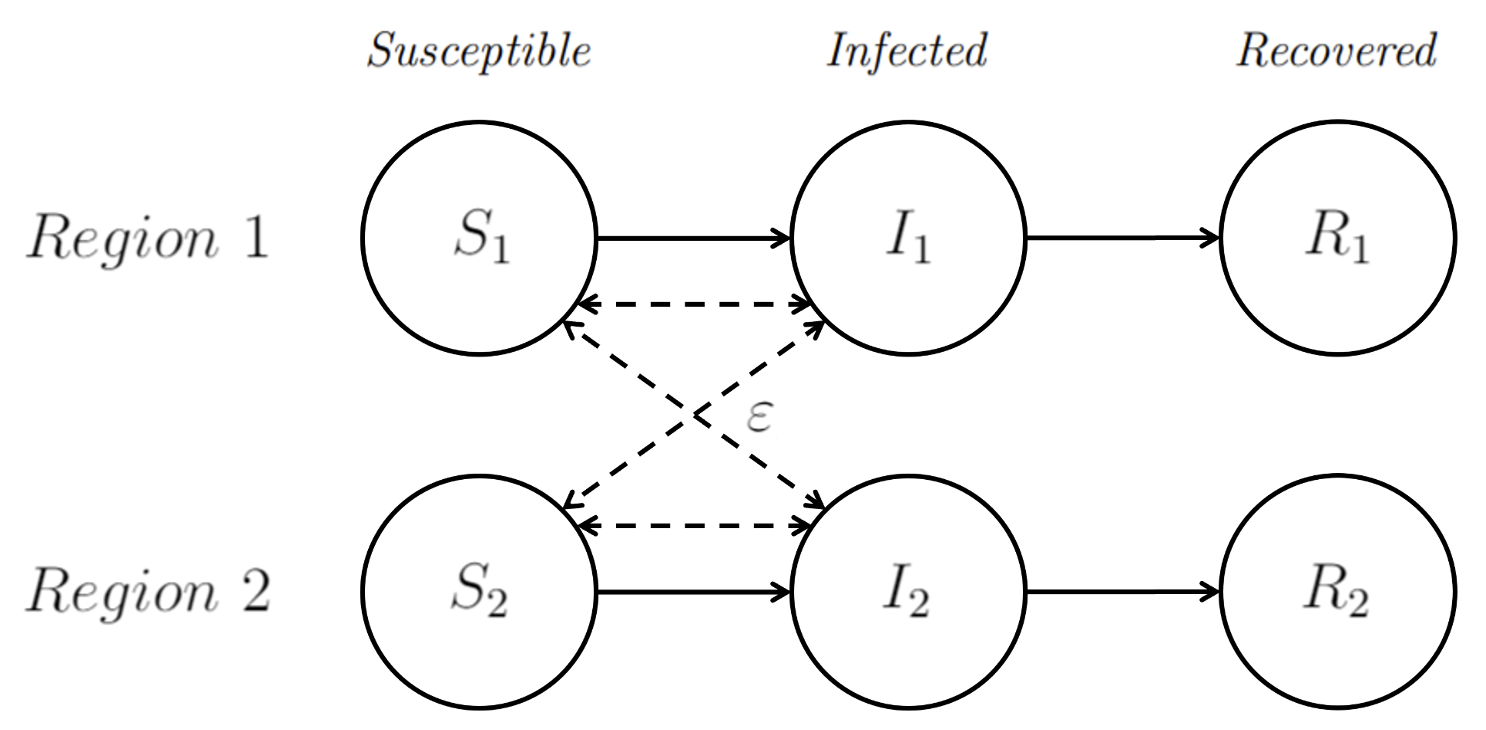
The model is depicted in Figure 1 and is based on a spatial SIR framework, where people live in two interconnected regions. We allow for the movement of people between regions, which introduces a channel for cross-regional infection. We capture the strength of interconnection between regions by a parameter ε.
Figure 1 Flow diagram of disease compartment transitions in the two-region SIR model
Notes: Dashed lines denote disease-transmitting contact structure.
Our model considers the implementation of economically costly mitigation measures that suppress the spread of the disease. These measures give rise to delicate intertemporal trade-offs with both health and socioeconomic costs. We characterise the optimal mitigation strategies and corresponding outcomes under three policy settings, which allows us to speak to the three policy questions posed above:
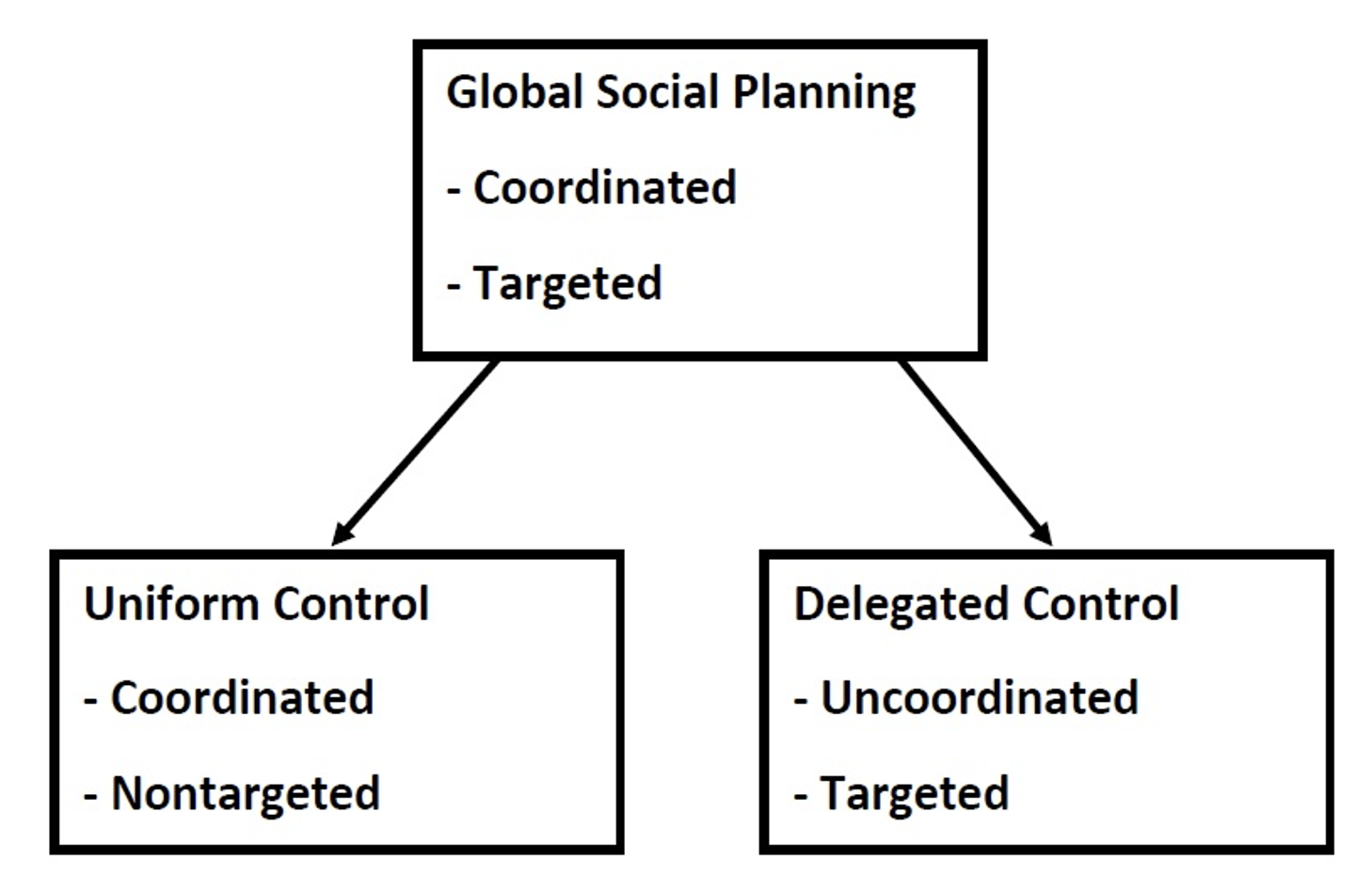
- global social planning: measures are fully coordinated across regions and targeted to local conditions to maximise overall welfare
- uniform control: measures are coordinated but not targeted locally
- delegated control: measures are targeted locally but not coordinated across regions
Comparing policies and outcomes under these three settings allows us to disentangle the different effects. This is illustrated in Figure 2.
Figure 2 Different policy settings and their properties
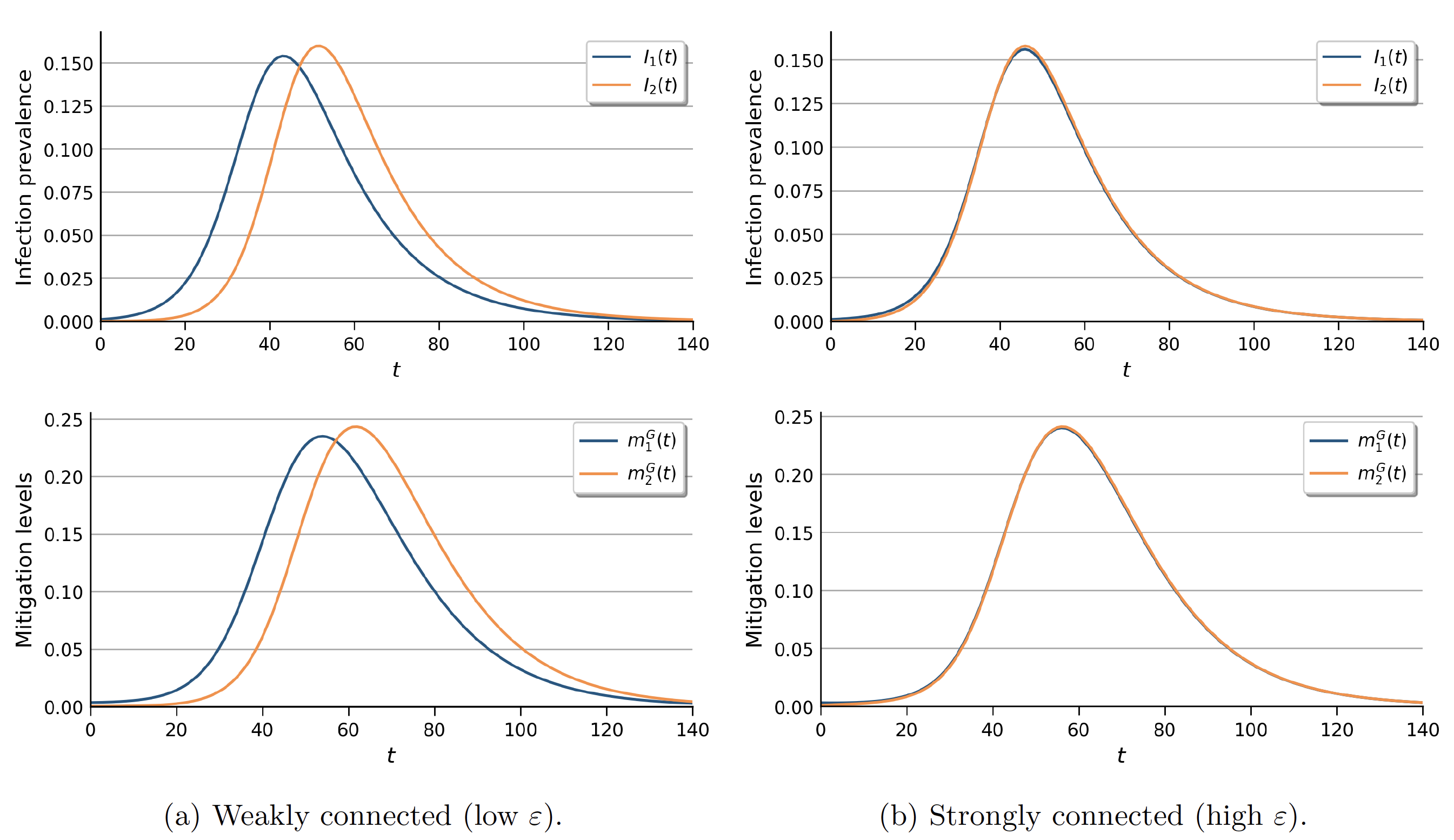
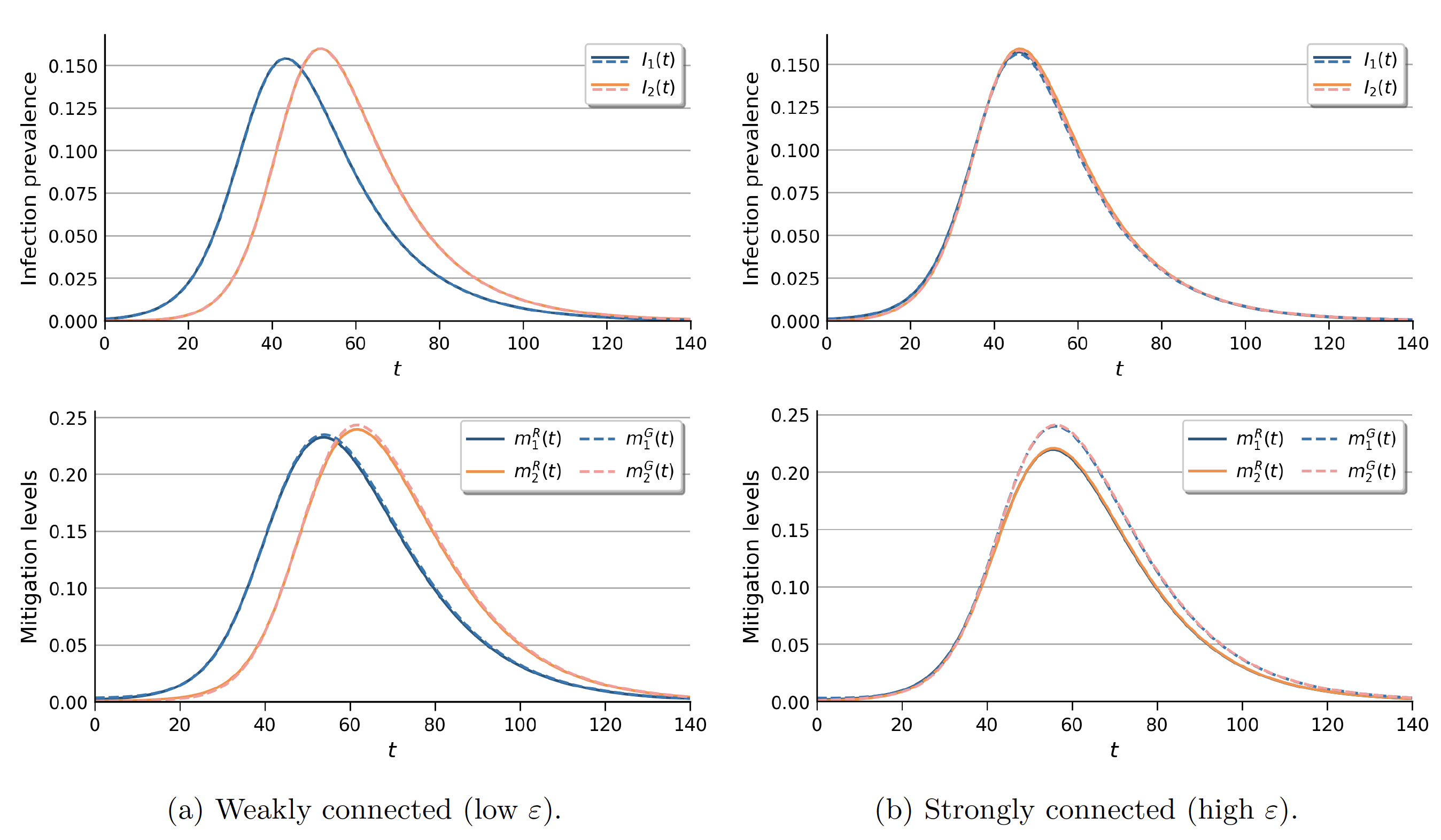
Figure 3 shows infection prevalence and mitigation levels under the socially optimal policy-setting benchmark, in which a global social planner sets targeted mitigation policies. One can see that the course of the epidemic depends on the level of interconnectedness between regions.
Figure 3 Infection prevalence and mitigation levels in the targeted global social planner setting
When regions are weakly connected, it takes time for infections to spread. As a result, differences in the regions’ infection levels persist throughout the epidemic. That is, extensive interactions tend to synchronise disease dynamics.
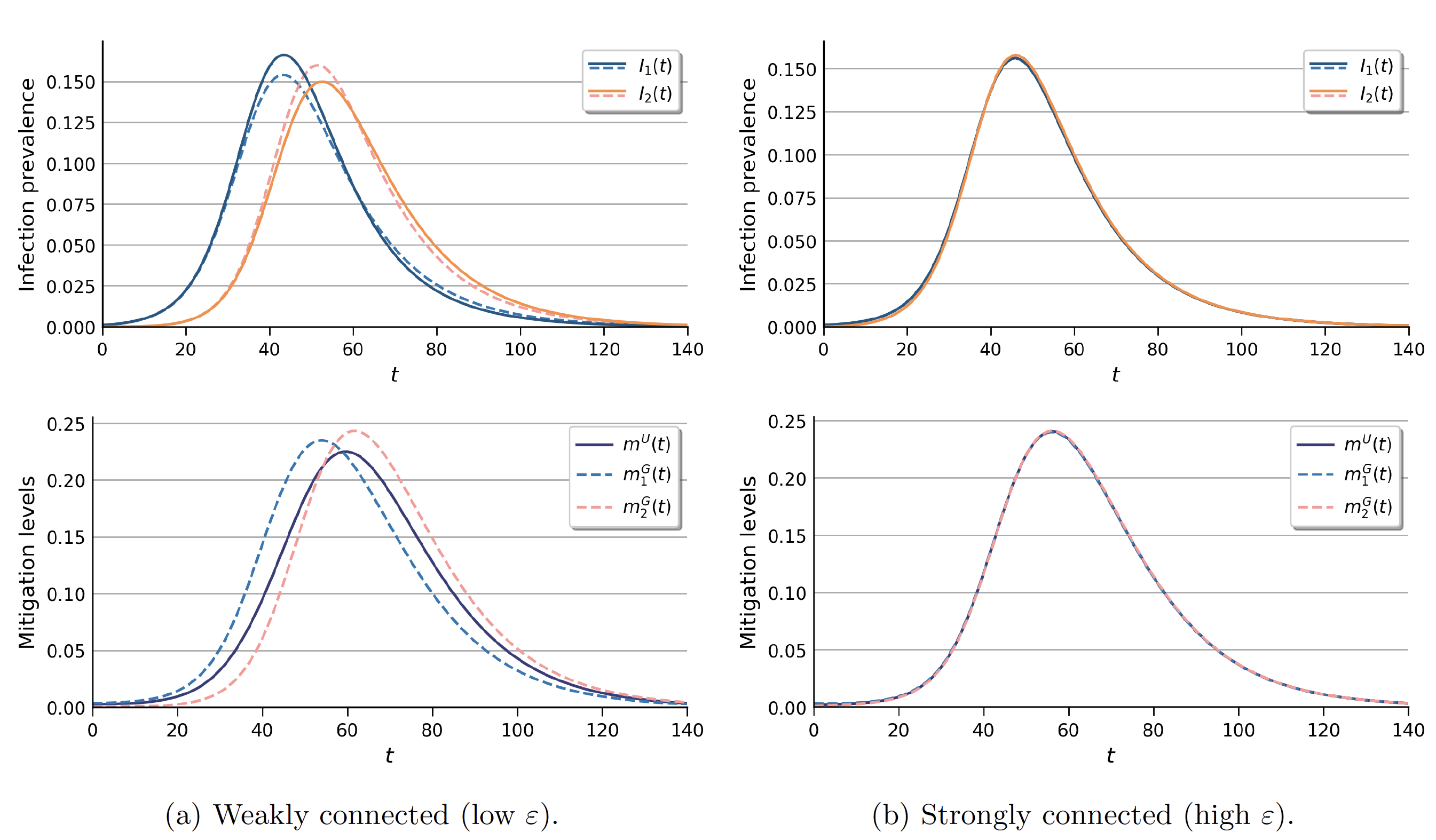
What happens if a social planner is restricted to using uniform policies, in which they set the same mitigation level in both regions? Figure 4 shows that the impact depends on the level of interconnectedness. When the planner is restricted to uniform policies, they have to compromise between the optimal mitigation levels of each region. The larger the difference between the regions, the more the planner will have to deviate from the geographically targeted ideal strategy.
Figure 4 Infection prevalence and mitigation levels in uniform policy setting vs targeted global social planner setting
Notes: Solid lines: uniform policy setting; dashed lines: targeted global social planner setting.
When regions are strongly connected, their infection and optimal mitigation levels are nearly identical. Thus, the uniform policy restriction requires little deviation from the optimal policy. On the other hand, when regions are weakly connected, the tension between the optimal mitigation levels requires a large deviation from the social planner’s ideal strategy. This results in a more severe epidemic with a noticeable loss in social welfare.
Last, the social planner may choose to delegate the mitigation decisions to the underlying regional jurisdictions. Doing so maintains an outcome of targeted policies but comes at the cost of a lack of coordination if regional policymakers act primarily in the interest of their local populations.
Figure 5 shows the infection prevalence and mitigation levels in this setting. Unlike in the case of uniform policies, the negative impact of delegation is most prominent when the regions are strongly connected. This is because one region’s mitigation benefits the other. By implementing mitigation measures, the region reduces its infections, which has a knock-on effect of infecting fewer people in the neighbouring region. If there is more cross-regional interaction, then mitigation reduces the rate of cross-regional infection further. The uncoordinated regional planners do not value this cross-regional benefit, which induces them to do less mitigation than is desirable.
Figure 5 Infection prevalence and mitigation levels in delegated policy setting vs targeted global social planner setting
Notes: Solid lines: delegated policy setting; dashed lines targeted global social planner setting.
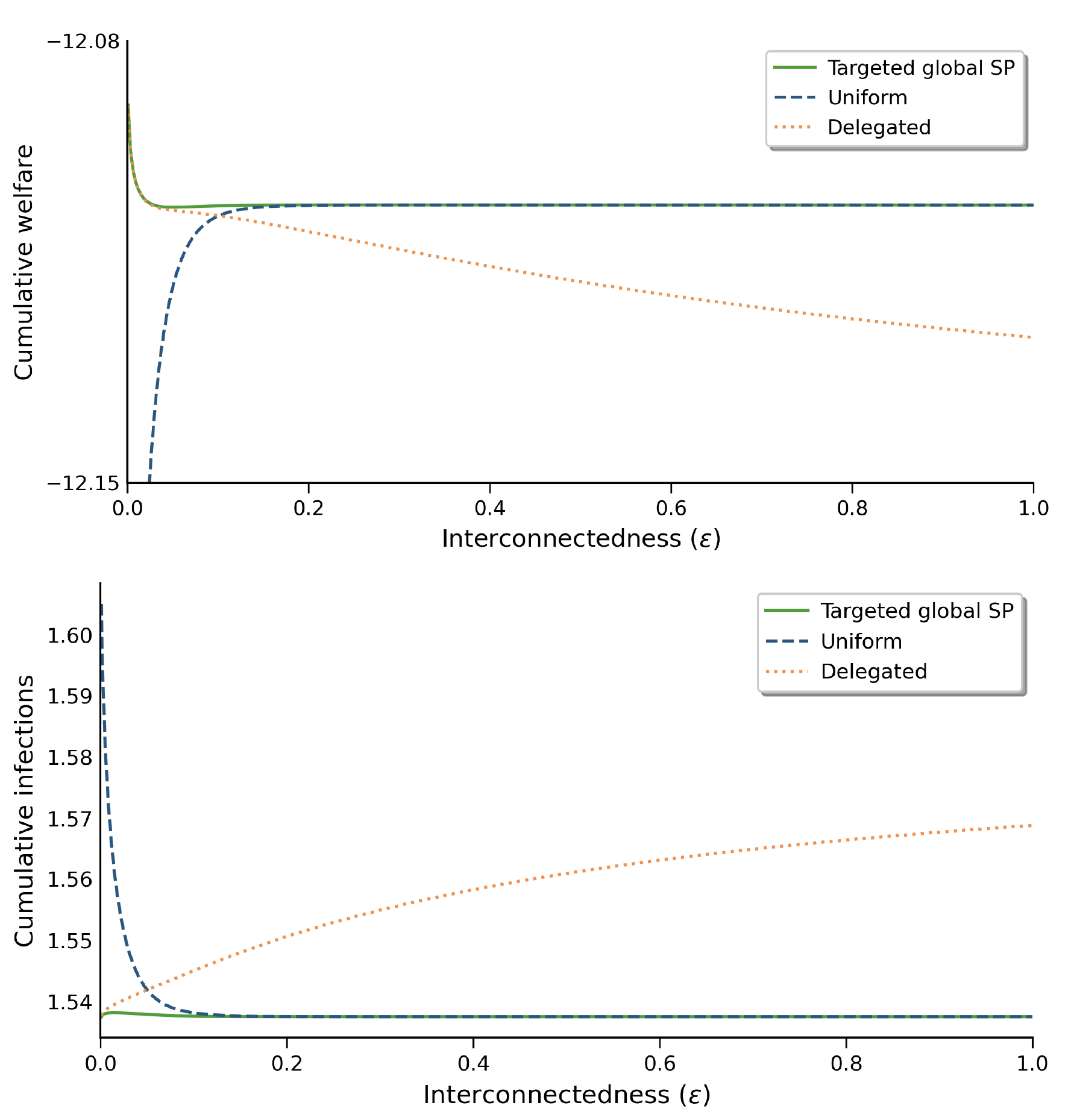
To summarise, we find that the costs associated with non-targeted and delegated disease-mitigation policies largely depend on the interconnectedness of the regions, as illustrated in Figure 6.
Figure 6 Cumulative welfare and infections under the different mitigation policy settings
If a government oversees regions of a local scale that typically have high levels of interconnectedness (for example, neighbouring towns and counties), then it should make sure that these regions’ policies are coordinated. Delegating mitigation to the regions’ local governments is likely to result in unnecessary costs and excessive infections.
Alternatively, if the regions have little cross-border interaction (for example, countries and distant states), policymakers should take care to tailor policies to local conditions. Applying a uniform policy across regions may involve a substantial cost to society.
These results highlight how important it is for policymakers to consider the spatial nature of their disease mitigation policies, both in terms of regional targeting and international coordination.
Furthermore, more investigation is needed on the role of travel restrictions in a comprehensive disease-control policy. An analysis covered in our paper suggests that the interaction with mitigation policies may make the benefits of travel restrictions more complex than one would initially expect.
As we look back and evaluate the responses of governments to the COVID-19 pandemic, we should pay special attention to their spatial design. If properly understood, it may help us make better disease-control policies in the future.
References
Burlig, F, G Schlauch and A Sudarshan (2021), “Examining COVID-19 travel restrictions in developing countries”, VoxEU.org, 27 June.
Centers for Disease Control (2020), “History of quarantine”, CDC.gov, 20 July.
Crucini, M, and O O’Flaherty (2021), “State-by-state decisions on shutdowns minimise Covid’s economic impact”, VoxEU.org, 29 May.
Department of Health and Social Care (2020), “Tiering decisions to be made through national command structure”, UK.gov, 26 November.
Deutschland.de (2022), “The Federal Government informs about the corona crisis”, 5 April.
Giannitsarou, C, and F Toxvaerd (2020), “What to do if COVID-19 is here to stay”, VoxEU.org, 12 July.
Hallas, L, A Hatibie, S Majumdar, M Pyarali and T Hale (2020), “Variation in US States’ Responses to COVID-19”, Blavatnik School of Government Working Paper.
Holtz, D, et al. (2020), “Interdependence and the cost of uncoordinated responses to COVID-19”, PNAS 117(33) 19837–43.
Hoover, D, and F Toxvaerd (2022), “Epidemics in space: Control, targeting and delegation”, CEPR Discussion Paper 17480.
Long, J A, M Malekzadeh, B Klar and G Martin (2021), “Do regionally targeted lockdowns alter movement to non-lockdown regions? Evidence from Ontario, Canada”, Health and Place 102668.
Sachs, J D, S S Abdool Karim, L Aknin, J Allen, K Brosbøl, F Colombo et al. (2022), "The Lancet Commission on lessons for the future from the COVID-19 pandemic", Lancet Commissions 400(10359): 1224–80.
Tatlow, H, E Cameron-Blake, S Grewal, T Hale, T Phillips and A Wood (2021), “Variation in the response to COVID-19 across the four nations of the UK”, Blavatnik School of Government Working Paper.
UK Cabinet Office (2020), “Guidance: COVID-19 winter plan”, UK.gov, 2 December.
Wrigley-Field et al. (2021), “Geographically targeted COVID-19 vaccination is more equitable and averts more deaths than age-based thresholds alone”, Science Advances 7(40).