The US Surgeon General has concluded that no level of second-hand smoke exposure is safe. Exposure is linked to lung cancer, coronary disease, and respiratory symptoms among other health problems (US Department of Health and Human Services 2006). As a result, many states and localities have enacted 100% smoke-free laws to reduce second-hand smoke exposure in non-residential indoor locations such as workplaces, restaurants, and bars.
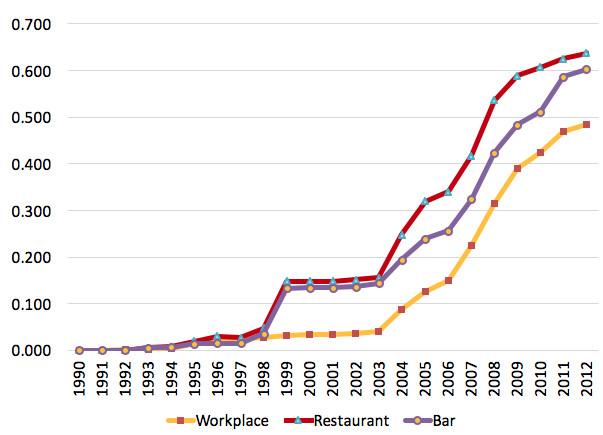
From 1990, when three counties in California enacted the first local 100% smoke-free laws the percentage of the US population living in an area with a 100% smoke-free law has grown substantially. By 2012, more than half of the US population lived in an area where 100% smoke-free legislation applied in at least one major venue (Figure 1).
Figure 1 Percentage of population exposed to 100% smoke-free laws, 1990-2012
Source: Authors’ calculations, based on data from the American Nonsmokers’ Rights Foundation.
The problem of displacement
For adults, evidence suggests that smoking bans make it more likely they will quit smoking (Carton et al. 2016, Levy and Friend 2003, Evans et al. 1999) and have better health outcomes (Shetty et al. 2011, Meyers et al. 2009, Seo and Torabi 2007).
But surprisingly little research has been done on the impact of the bans on infant and child health. Second-hand smoke exposure has been associated with lower birth weight and higher incidence of Sudden Infant Death Syndrome among infants, and to poor respiratory health and ear infections among children. If more adults stop smoking, this could improve health outcomes among children. But if bans displace smoking instead so that some smokers smoke at home instead of outside it, and pregnant women and children are present, it could reduce or eliminate the beneficial effects. If smoking bans lead to more smoking at home, which is the primary site for children’s second-hand exposure (Yousey 2006), the policies may have a negative impact on infant and child health.
There is some evidence of this behaviour. For example, Ho et al. (2010) found higher rates of self-reported second-hand smoke exposure among never-smoking primary school students following a comprehensive smoking ban in Hong Kong. In the US, Adda and Cornaglia (2010) found evidence that smoke-free laws shift time spent in locations where smoking is banned to time spent at home, and were associated with increased cotinine levels in children, a marker for second-hand smoke exposure. They were not able to directly test whether adults were more likely to smoke at home, however. Also, both of these studies focused on second-hand smoke exposure rather than on measures of child health expected to respond to exposure.
Several international studies imply that smoke-free legislation improved birth outcomes (Bhardwaj et al. 2014) or reduced asthma-related hospitalisations among children (Lee et al. 2016, Mackay et al. 2010). But research examining the connection between smoke-free bans and infant and child health in the US has had restricted geographical coverage and mixed results. For example, a Minnesota-based study found significant reduction in asthma-related emergency department visits among both adults and children after the implementation of 100% smoke-free legislation in workplaces, restaurants, and bars (Croghan et al. 2015). On the other hand, the results of one of the most comprehensive studies, which analysed birth outcomes using data for 29 states and New York City, found a limited effect from smoking bans. The study suggested that cigarette excise taxes had a greater impact (Markowitz et al. 2013).
We recently examined the effects of 100% smoke-free laws on infant and child health in the US using comprehensive information on changes to legislation at the state and local levels (McGeary et al. 2017). We used the 1990-2012 US natality files, which contain data for all US births (our sample included 86.3 million births), to analyse infant health outcomes such as birth weight. We also used the 1998-2013 National Health Interview Survey, a nationally representative federal survey, to examine child health outcomes such as respiratory and asthma symptoms. In this case, our sample included 167,328 children. We used changes to smoke-free laws at state and locality level to estimate the impact on infant and child health.
The effect on infant health
Our main estimates compared states and localities that enacted the most stringent laws – 100% bans in worksites, restaurants, and bars – to those that did not have any ban in place. This regression-based difference-in-differences design controlled for state fixed effects to ensure no bias would be introduced by time-invariant state-level characteristics that could increase the propensity to implement smoke-free legislation and affect infant and child health, as well as year fixed effects to account for bias from national trends in infant and child health. We also controlled for the state-level cigarette excise tax, which varied over time during our study period and has been shown to affect both the decision to give up smoking and birth outcomes (Markowitz et al. 2013).
Some of our analyses restricted the sample to infants and children with mothers who attained a high school diploma or GED or less education, because these mothers were more likely to smoke, and to be exposed to second-hand smoke, because of where they lived.
We found that comprehensive smoke-free legislation increased average birth weight and reduced the likelihood of low birthweight (under 2.5 kg) infants, particularly among low-educated mothers. Comparing areas with the most stringent smoke-free legislation to those with the least, infants born to mothers with low education levels weighed about 18 grams more on average (0.6% increase) and were about 0.3 percentage points less likely to have a low birth weight (4.2% decline). We also found evidence that 100% smoke-free laws increased gestational age and birth weight given gestational age.
Two main mechanisms could explain these findings, although they are difficult to disentangle:
- Mothers give up cigarettes. Smoking bans may make it more likely that a pregnant woman stops smoking.
- Less exposure to smoke. Bans may reduce a pregnant woman’s second-hand exposure.
Our analysis suggests that most of the effect can be attributed to the second mechanism.
The effect on child health
Our analysis of the National Health Interview Survey suggested improvements in child health following implementation of the most stringent smoke-free laws. We found that 100% smoke-free laws reduced the likelihood of a recent asthma attack, of visiting the ER for any reason, and of having three or more ear infections in the past year.
As before, effects were greatest among children whose mothers had a low level of education. For example, we found a nearly 5 percentage point reduction in the likelihood of an ER visit for any reason among this group, representing a 25% reduction relative to the sample mean. Effects were also larger among children with asthma, who are especially vulnerable to the effects of second-hand smoke exposure. We found a more than 5 percentage point reduction in the likelihood of a recent asthma attack among these children, representing about a 13% reduction relative to the sample mean.
Since children’s exposure to second-hand smoke is unlikely to occur in, or near, worksites and bars, the positive effect of 100% smoke-free laws on child health suggests that these laws may reduce children’s exposure outside of banned locations. To investigate this prospect directly, we examined whether 100% smoke-free laws affected the likelihood that an adult smoked one or more days per week in a home in which children were present. We found some evidence that the most stringent bans were associated with a reduction in smoking inside the home, relative to having no ban in place. As before, effects appeared to be more concentrated among households where at least one adult resident had a high school diploma or GED or less education.
None of our estimates suggest a positive impact on smoking inside the home that is statistically or economically significant. On this evidence, 100% smoke-free laws do not displace smoking from banned locations to the home.
Concluding remarks
Our results suggest that implementing bans on smoking in worksites, restaurants, and bars improves infant and child health, mainly by reducing second-hand smoke exposure among both pregnant women and children.
Though it was not the focus of our study, we also examined limited and partial smoking bans. We found that they were not nearly as effective as 100% smoke-free bans. While 41 states had enacted some form of 100% smoke-free legislation as of July 2016, only 25 states, representing about 58% of the US population, had enacted 100% smoke-free bans in all major public venues.
On this evidence, there are additional benefits to complete bans beyond smoking cessation among current smokers and improvements in adult health. These benefits should be considered when states and localities debate smoke-free legislation.
References
Adda J and F Cornaglia (2010), “The Effects of Bans and Taxes on Passive Smoking”, American Economic Journal: Applied Economics 2(1): 1-32.
Bharadwaj, P, J V Johnsen, and K V Løken (2014), "Smoking bans, maternal smoking and birth outcomes", Journal of Public Economics 115: 72-93.
Carton, T W, M Darden, J Levendis, S H Lee and I Ricket (2016), “Comprehensive Indoor Smoking Bans and Smoking Prevalence: Evidence from BRFSS”, American Journal of Health Economics 2(4): 535-556.
Croghan I T, J O Ebbert, J T Hays, D R Schroeder, A M Chamberlain, V L Roger, and R D Hurt (2015), “Impact of a county-wide smoke-free workplace law on emergency department visits for respiratory diseases: a retrospective cohort study”, BMC Pulmonary Medicine 15: 1-8.
Evans, W, M C Farrelly, and E Montgomery (1999), “Do Workplace Smoking Bans Reduce Smoking?” American Economic Review 89(4): 728-747.
Ho S Y, M P Wang, W S Lo, K K Mak, H K Lai, G N Thomas, and TH Lam (2010), “Comprehensive smokefree legislation and displacement of smoking into the homes of young children in Hong Kong,” Tobacco Control 19: 129-33.
Lee S L, W H Wong, and Y L Lau (2016), “Smoke-free legislation reduces hospital admissions for childhood lower respiratory tract infection”, Tobacco Control 25: e90-94.
Levy D T and K B Friend (2003), “The effects of clean indoor air laws: what do we know and what do we need to know?” Health Education Research 18(5): 592-609.
Mackay D, S Haw, J G Ayres, C Fischbacher, and J P Pell (2010), “Smoke-free legislation and hospitalizations for childhood asthma,” New England Journal of Medicine 363: 1139-1145.
Markowitz S, E K Adams, P M Dietz, V Kannan, and V Tong (2013), “Tobacco control policies, birth outcomes, and maternal human capital”, Journal of Human Capital 7: 130–60.
McGeary K A, D M Dave, B J Lipton, and T Roeper (2017), “Impact of comprehensive smoking bans on the health of infants and children”, NBER Working Paper no. 23995.
Meyers D G, J S Neuberger, and J He (2009), “Cardiovascular Effect of Bans on Smoking in Public Places: A Systematic Review and Meta-Analysis”, Journal of the American College of Cardiology 54: 1249- 1255.
Seo D and M Torabi (2007), “Reduced Admissions for Acute Myocardial Infarction Associated with a Public Smoking Ban: Matched Controlled Study”, Journal of Drug Education 37(3) :217-226.
Shetty K D, D Thomas, C White, J Bhattacharya (2011), “Changes in US hospitalization and mortality rates following smoking bans”, Journal of Policy Analysis and Management 30(1): 6-28.
US Department of Health and Human Services (2006), The Health Consequences of Involuntary Exposure to Tobacco Smoke: A Report of the Surgeon General, Atlanta: National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health.
Yousey, Y K (2006), “Household Characteristics, Smoking Bans and Passive Smoke Exposure in Children”, Journal of Pediatric Health Care 20(2): 98-105.