Since the 1994 Cairo conference on population and development, the reproductive health rights of women have received significant attention. And progress seems to have been made across the globe, judging from the aggregate global statistics on reproductive health (see Ross et al. 2005).
The apparent success seems to have made policy advisers and advocates overconfident that fertility levels and maternal health are no longer a problem. They have shifted to focus almost exclusively on HIV/AIDS, which received only 7% of funding in the 1994 Cairo pact.
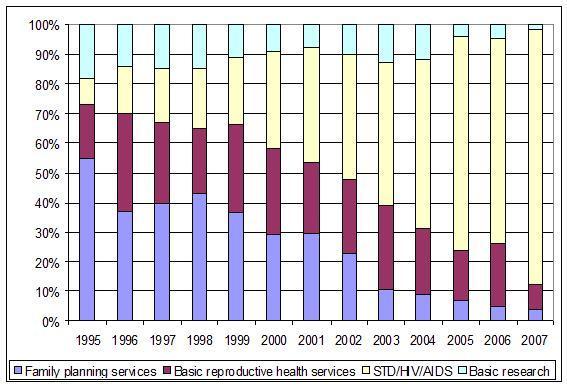
Investment in health should be a delicate balancing act, but Figure 1 makes the present imbalance eminently clear. Virtually all attention and efforts now go to HIV/AIDS. Just after the Cairo conference, the situation was quite the reverse. Donor countries from the OECD allocated 54 percent of their earmarked funds to family planning, 15 percent to reproductive health care, and 10 percent to HIV/AIDS. Investments in maternal health can be traced in large part in the UN system under the headings of reproductive health and family planning.
Figure 1. Donor allocation of population assistance, 1996-2007
Source: UNFPA/UNAIDS/NIDI. Note: 2006 figures are preliminary; 2007 are projections.
Maternal health care at the back of the minds and hearts of donors
HIV/AIDS is almost completely crowding out the funds going to maternal health. In 2005 HIV/AIDS received 72 percent of donors’ aggregate $6.8 billion in funding, and this development does not seem likely to be reversed in the near future. Aid organisations are still enmeshed in the old development aid rhetoric of ”moving the money”. This is also illustrated by the recently held UN 2008 high-level meeting on AIDS. The scenario for universal access by 2010 requires resources between $27 billion and $43 billion in 2010 and $35 to $49 billion in 2015. To close the gap, it is stated, existing international donor commitments must be fulfilled and new ones made.
Of course, much attention and money goes to Sub-Saharan Africa but even here one would like to see a more balanced investment approach. Seventy-three percent of donor aid transferred to Sub-Saharan Africa is allocated to HIV/AIDS (calculated on the basis of UNFPA/UNAIDS/NIDI database). In other words, maternal health care has moved to the back of the minds and hearts of donors.
The main driver behind this unbalanced result is a mixture of:
- real concern for HIV/AIDS,
- the unbalanced treatment of family planning in the Millennium Development Goals,
- the comfortable but naïve idea that fertility will slow down by its own internal dynamics, and
- the overpowering dominance of the United States in pushing its own priorities in global health programs (van Dalen and Reuser, 2006).
Dominance is seldom healthy, in private as it is in public affairs, as religious values keep playing a dominant role in the allocation of donor funds (van Dalen, 2008). In line with donors, domestic governments and NGOs in Sub-Saharan Africa allocated 77 percent of their funds to HIV/AIDS in 2005.
Overemphasising HIV/AIDS undermines African health
There are two main reasons why the crowding out of maternal health investments by HIV/AIDS is worrisome.
1) HIV/AIDS programmes would profit considerably from a more balanced approach, as maternal health and family planning investments go to the heart of the problems of Sub-Saharan countries – high population growth rates keeping numerous countries trapped in poverty (Cleland and Sinding, 2005).
In most countries, the total fertility rate, the expected total number of children per woman, hovers around five, far above the replacement rate of 2.1 children. Judging from the demographic health surveys carried out in developing countries, desired fertility rates fell faster over time than the actual rates. This is reflected in high levels of unmet need and high proportions of births that are ill-timed or unwanted. High fertility leads to rapid population growth rates, exacerbating scarcity in health care, education, land for farmers, and all other public domains of life.
Family planning might alleviate some of these problems. But apparently it is no longer the ”hot” subject it was for such a long time at many a population conference. Insiders to these negotiations claim that family planning seems even to have become ”morally suspect” again (Blanc and Tsui, 2005).
This is particularly unfortunate because there is little evidence of progress in maternal health and investment is very much needed. The lifetime risk of maternal death in developing countries is still as high as ever: 1 in 61 women die in developing countries from pregnancy-related causes, and the numbers are even worse for Sub-Saharan Africa (1 in 16 women die), whereas in the developed world the risk is 1 in 2800.
2) The unprecedented rise of HIV/AIDS funds is disrupting fiscal policy and local health care systems whereas a more balanced investment in reproductive health and HIV/AIDS would make use of the existing infrastructure.
Vertical programs like HIV/AIDS erode the primary health care systems in developing nations. The new HIV/AIDS funds are swamping public health budgets, in some cases exceeding 150 percent of the government’s total allocation to health care (Lewis, 2006).
Too much money must be spent in too short a time. Such a situation, particularly in the conditions of extreme poverty and poor governance prevalent in Sub-Saharan Africa, easily results in “poaching” of health care workers and bureaucrats from other worthy public projects.
Large “white elephant” investment projects signal to donors that money is being spent, but unfortunately it is not spent wisely. When public governance systems are weak, these large but volatile sums of ”easy money” promote corruption, moonlighting, and absenteeism in delivering health care (World Bank, 2004).
Conclusion
Foreign aid not contingent on good governance may be severely damaging to political institutions. Donors and international agencies should abide by the Hippocratic oath: do no harm.
The history of foreign aid in sub-Saharan Africa is not a happy one: collective action is an intricate and delicate balancing act. Spending large aid budgets on HIV/AIDS is a delicate cocktail, and an unbalanced mixture may do more harm than donors imagine. Foreign aid ought to be guided not by fleeting opinion and charity but by evidence and true engagement, aiming at long-term sustainable solutions.
References
Blanc, A., and A. Tsui, 2005, The Dilemma of Past Success: Insiders’ View on the Future of the International Family Planning Movement, Studies in Family Planning; 36: 263-276.
Cleland, J., and S. Sinding, 2005, What would Malthus say about AIDS in Africa?, The Lancet.
Lewis, M., 2005, Addressing the Challenges of HIV/AIDS: Macroeconomic, Fiscal and Institutional Issues, Working Paper, no. 58, Center for Global Development.
Ross, J., J. Stover, and D. Adelaja, 2005, Profiles for Family Planning and Reproductive Health Programs, 2nd edition, Futures Group, Glastonbury.
H.P. van Dalen, 2008, Designing Global Collective Action in Population and HIV/AIDS Programs, 1983-2002: Has Anything Changed?, World Development, 36(3): 362-382.
H.P. van Dalen, and M. Reuser, 2006, What Drives Donor Funding in Population Assistance Programs? Evidence from OECD Countries, Studies in Family Planning, 37: 141-154.
World Bank, World Development Report – Making Services Work for Poor People, Oxford University Press, Oxford, 2004.
Addendum
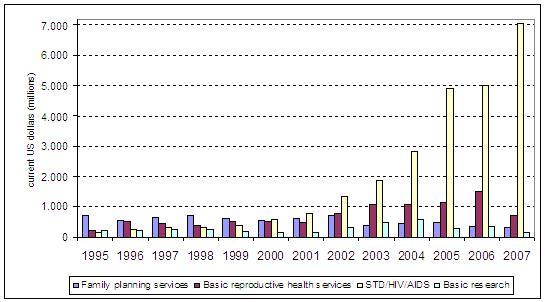
The corresponding dollar figures of Figure 1 are presented in Figure 2. The absolute amount of donor aid allocated to HIV/AIDS is not only dominant in relative terms but also absolute terms. The allocations to the other categories are far below the promised Cairo targets from the start and show little development over time. Family planning is crowded out by the donor allocations to HIV/AIDS.
Figure 2 Donor allocation of population assistance in dollars, 1996-2007 (current US dollars, in millions)