Top-down health interventions often fail at the point of delivery, despite improvements in health technology and access. A recent salient example occurred during the Ebola outbreak in West Africa in 2014-2015. There were widespread reports of communities refusing health workers because of mistrust (Neporent 2014). More broadly, vaccination campaigns conducted in many sub-Saharan African countries against diseases such as measles and polio have been unable to reach herd immunity rates due to low demand for the vaccinations (Kindzeka 2015). Thus, even once supply and technological issues have been addressed, health interventions often struggle during this ‘last mile’ of implementation (Dupas 2011, Dupas and Miguel 2017).
In a recent study (Lowes and Montero 2018), we examine one potential barrier to the efficacy of health interventions, namely, mistrust in medicine arising from historical exposure to colonial health campaigns. We focus on medical campaigns to combat sleeping sickness conducted by the French military in Cameroon and former French Equatorial Africa (AEF). These campaigns forced individuals, often at gunpoint, to receive treatment and prophylaxis for sleeping sickness using drugs with serious side effects. We link these campaigns to the success of World Bank health projects, trust in medicine, and health outcomes today.
Description of the campaigns
Between the 1920s and 1950s, the French military undertook extensive medical campaigns in sub-Saharan Africa aimed at managing tropical diseases. In Cameroon and former AEF (present day Central African Republic, Chad, Republic of Congo, and Gabon), the French military organised mobile medical teams to combat a variety of diseases, including sleeping sickness, leprosy, yaws, syphilis, and malaria. The most extensive of these campaigns focused on sleeping sickness, a lethal disease spread by the tsetse fly. Over the course of several decades, millions of individuals were subjected to medical examinations and forced to receive injections of various medications meant to either treat or prevent sleeping sickness. However, these medications had dubious efficacy and serious side effects, including blindness in up to 20% of individuals, gangrene, and death. The sleeping sickness campaigns constituted some of the largest colonial health investments, and for many, these campaigns were their first exposure to modern medicine (Headrick 1994, Pepin 2011, Lachenal 2014).
Measuring campaign exposure
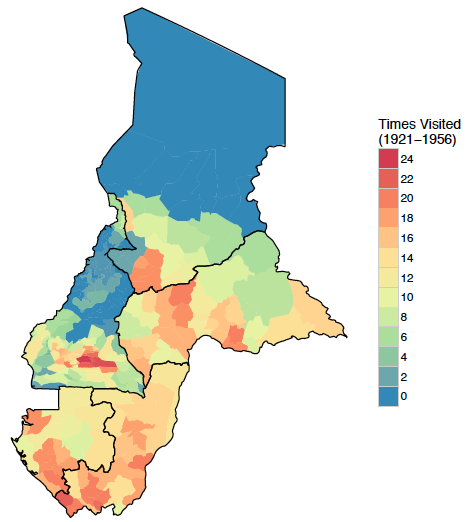
To measure exposure to colonial medical campaigns, we construct a dataset from over 30 years of data from French military archives for five countries. We digitise the data, documenting the locations of sleeping sickness campaign visits at a granular geographic level between 1921 and 1956. We measure exposure to the campaigns as the share of years that a location is visited during the years of the campaigns. See Figure 1 for a map of the distribution of campaign visits.
Figure 1 Map of colonial medical campaign visits between 1921 and 1956
Colonial medical campaigns and World Bank project success
We first examine the relevance of historical medical campaigns for present-day health policy by examining how differential exposure to colonial medical campaigns affects the success of present-day health interventions. We use data on the location of World Bank projects approved between 1995 and 2014 to examine how exposure to medical campaigns affects project success, as rated by the World Bank using data from AidData. The World Bank rates projects on a 6-point scale from “highly unsatisfactory” to “highly satisfactory”. We compare the success of health projects and non-health projects by historical medical campaign intensity.
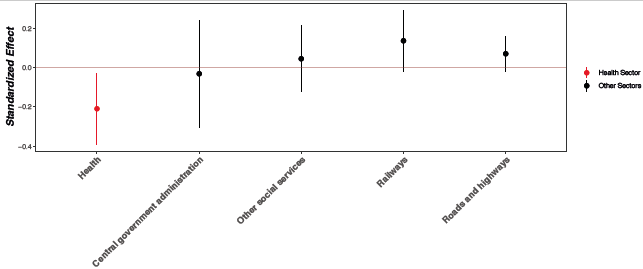
We find that greater exposure to the campaigns is correlated with less successful health projects, but does not negatively affect the success of projects in other domains. The effect size of historical medical campaigns for health project ratings is equivalent to changing the rating from "moderately satisfactory" to "moderately unsatisfactory” for an area with the average number of colonial medicine campaign visits. These results highlight the importance of the colonial medical campaigns for understanding the efficacy of present day health policies, and more broadly, how historical experiences can affect policy.
Figure 2 Estimated effect of colonial medical campaign exposure on World Bank project success by sector
Medical campaigns and mistrust in medicine
We then explore a potential mechanism to explain why historical exposure to colonial medical campaigns affects the success of World Bank health projects. We examine whether the colonial medical campaigns affect trust in modern medicine. This is motivated by work from anthropology and history that links colonial medical campaigns against sleeping sickness and mistrust in medicine. Regarding tetanus campaigns in Cameroon in the 1990s, Feldman-Savelsberg et al.(2000) note, “[The tetanus campaigns] awakened negative collective memories of French colonial medical efforts to wipe out sleeping sickness” (p. 162). Similarly, in CAR, anthropologist Giles-Vernick (2002) reports of rumours of injections that brought death. Additionally, the Etonethnic group in Central Cameroon has a song describing the injections as painful and administered under coercion (Lachenal 2014). Thequalitative evidence from historians and anthropologists suggest that the campaigns may have affected trust in medicine because villagers were forced to receive injections, many of the medications had serious negative side effects, and the medications were ineffective.
Measuring trust in medicine
There are no self-reported measures of trust in medicine available for our area of interest. Therefore, we measure trust in medicine by whether an individual consented to a free and non-invasive blood test for either anaemia or HIV in the Demographic and Health Surveys (DHS). We consider consent to the blood tests to be a revealed preference measure of trust.
Blood test refusals and historical campaign exposure
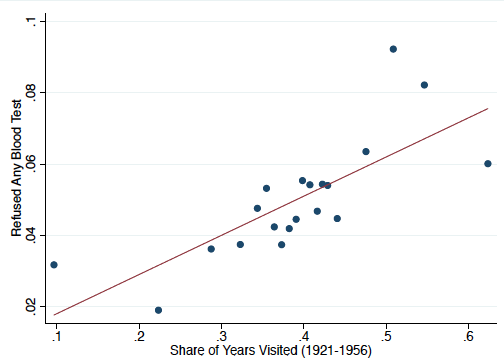
We find that increased exposure to colonial medical campaigns is associated with lower levels of trust in medicine today. Approximately 4.7% of the sample refused the blood tests. Being visited by the colonial medical campaigns for 15 years, the average number of years an area is visited, increased refusals by 5.1%. Note that these levels of refusals for a vaccination campaign would prevent the achievement of herd immunity rates for many diseases. The results are robust to a variety of geographic, colonial, pre-colonial, and individual level controls. The strong correlation remains when we examine anaemia blood test refusals or HIV blood test refusals separately.
Figure 3 Correlation plot between share of years visited and blood test refusal
Trust in other people or institutions
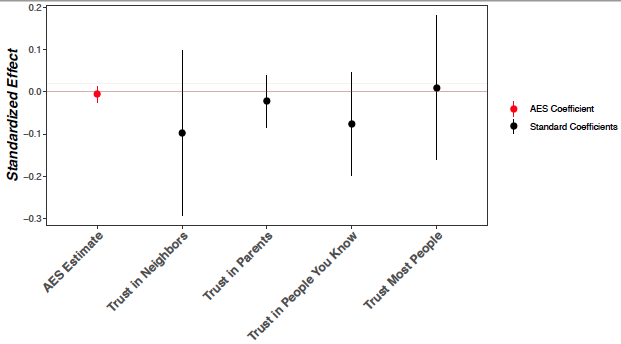
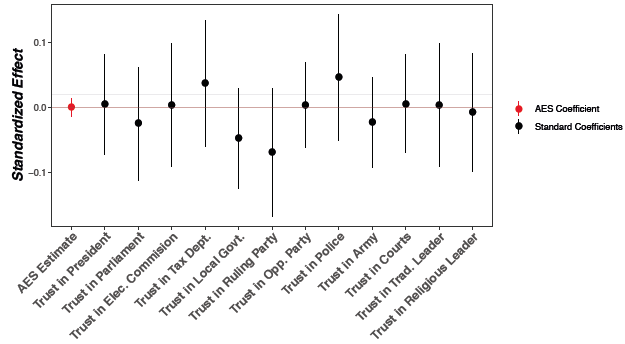
We also explore whether the observed mistrust is specific to trust in medicine or can be generalised to trust in other people or institutions. We use Afrobarometer data from Cameroon and Gabon on trust in a variety of other people and institutions – e.g. neighbours, people you know, local government, police, traditional leaders – to test whether exposure to medical campaigns affects other forms of trust. We find that there is no effect of exposure to the medical campaigns on trust in these non-medical individuals and institutions. These results highlight that the effect of exposure to medical campaigns is specific to the medical domain.
Figure 4 Estimated effect – trust questions in the Afrobarometer round 5 for Cameroon
Figure 5 Estimated effect – trust questions in the Afrobarometer round 6 for Cameroon and Gabon
Effects on anaemia, HIV, and childhood vaccinations
Given that the health campaigns predict measures of trust in medicine, it is important to examine the implications for health outcomes. First, we examine the outcomes for the two blood tests administered in the DHS, with the caveat that our previous analysis shows selection into who consents to take the blood test. We find evidence of worse health outcomes in areas with greater exposure to the campaigns – individuals are more likely to have anaemia (lower haemoglobin levels). Additionally, we find some evidence of higher HIV prevalence in areas with greater exposure to the medical campaign.
Finally, we construct an index of childhood vaccination completion. In areas with greater exposure to the campaigns children have lower levels of vaccination rates. A one standard deviation increase in colonial medical campaign visits reduces vaccination rates of children by 0.064 standard deviations. Our results provide evidence that the history of colonial medical campaigns is associated with worse health outcomes in both the biomarker data and in terms of vaccination rates for children.
Conclusion
The historical medical campaigns provide several important lessons for present-day development policy. First, top-down aid that is implemented poorly and without local consent and involvement can have long lasting unintended consequences. Second, the success of present-day health interventions or policies may depend on the historical experiences of the target populations. Finally, building and maintaining trust in medicine should remain a priority for modern health interventions.
This article has been reposted on VoxDev, our partner website which focuses on research in development economics.
References
Dupas, P (2011), “Health Behavior in Developing Countries,” Annual Review of Economics, 3, 425–449.
Dupas, P, and E Miguel (2017), “Impacts and Determinants of Health Levels in Low-Income Countries,” in E Duflo and A Banerjee (eds.), Handbook of Field Experiments, Vol. 2, North Holland.
Feldman-Savelsberg, P, F T Ndonko, and B Schmidt-Ehry (2000), “Sterilizing Vaccines or the Politics of the Womb: Retrospective Study of a Rumor in Cameroon,” Medical Anthropology Quarterly 14 (2), 159–179.
Headrick, R (1994), Colonialism, Health and Illness in French Equatorial Africa, 1885-1935, African Studies Association Press.
Kindzeka, M E(2015), “Cameroon Finds Resistance to Polio Vaccination Campaign,” Voice of America News, 27 September.
Lachenal, G (2014), Le Médicament qui Devait Sauver l’Afrique (The Hidden Story of the Medicine Meant to Save Africa), La Découverte.
Lowes, S, and E Montero(2018), “The Legacy of Colonial Medicine in Central Africa,” working paper.
Neporent, L(2014), “Doctors Battling Ebola Are Met with Fear, Mistrust,” ABC News, 28 July.
Pépin, J (2011), The Origins of AIDS, Cambridge University Press.