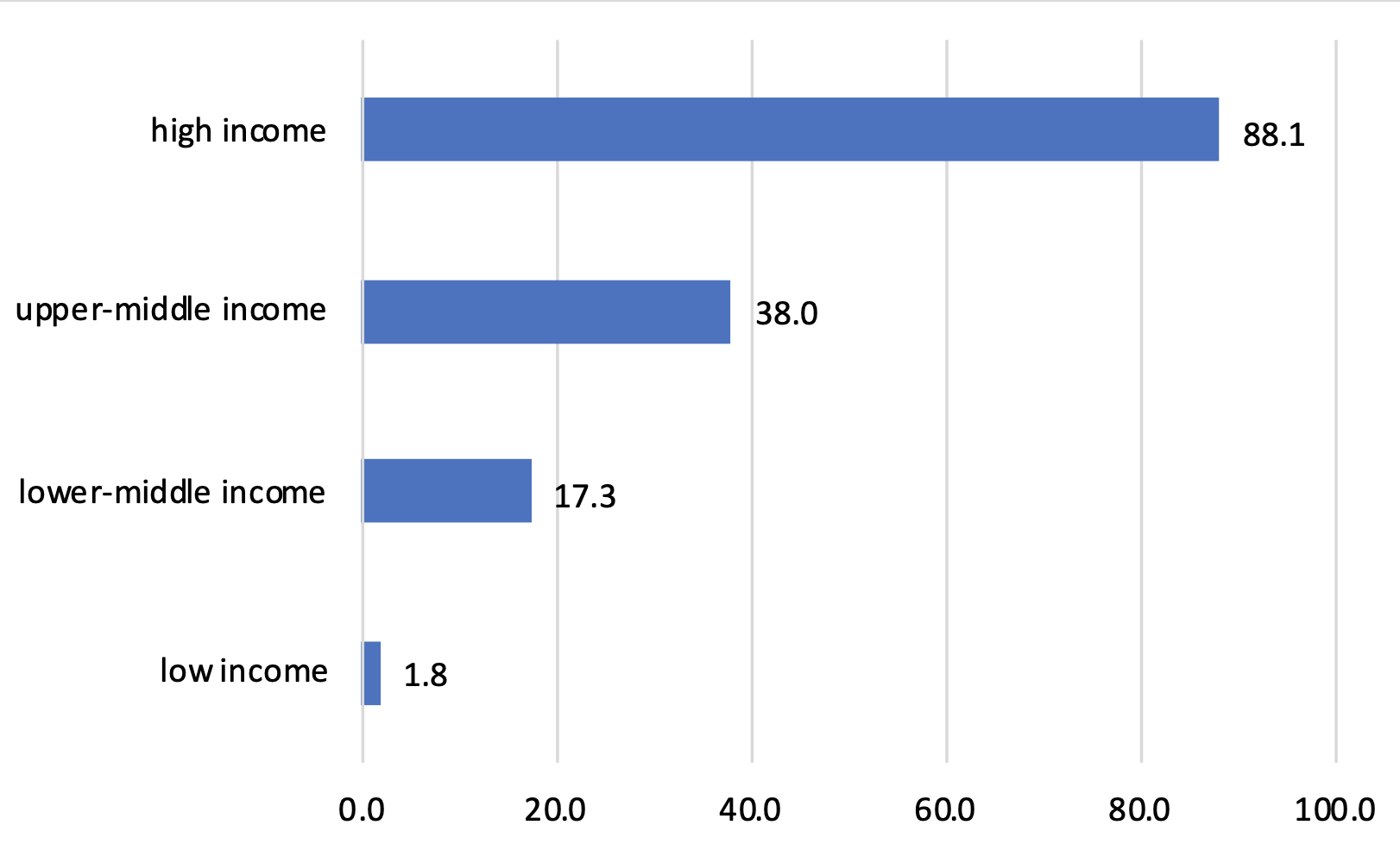
The Covid-19 pandemic has forced governments to make difficult ethical choices. To what extent and for how long should economically costly lockdowns be imposed for the sake of population health? Who should be prioritised in the allocation of vaccines and other scarce medical resources like ventilators or intensive care unit beds? The majority of Covid-19 vaccine shots have been administered to rich countries (Figure 1). Should vaccine doses be equitably shared globally, or should countries first and foremost address the health and economic well-being of their own citizens?
Figure 1 Vaccination rates by country income level (doses administered per 100 people)
Source: Our World in Data, 19 July 2021, https://ourworldindata.org/covid-vaccinations
All these choices involve health and income trade-offs, and their consequences are often heterogeneously distributed across the population. For example, older adults are at highest risk of severe Covid-19, but the working-age group primarily feels the burden of economic lockdowns, with disproportionate impacts on low socioeconomic-status individuals due to the type and sector of their occupations (e.g. jobs that cannot readily be done at home). In the design of vaccine prioritisation strategies, a trade-off also arises between protecting the health of high-fatality-risk individuals (i.e. older adults and individuals with comorbidities) and the health of high-exposure-risk individuals who perform activities essential for the functioning of society or work in economically critical sectors.
The broad question these examples raise is how to evaluate health-related interventions that can have different health and socioeconomic spillover effects throughout the population.
Traditional evaluation methods, such as cost-effectiveness analysis (CEA) and benefit-cost analysis (BCA), are poorly suited to deal with the complexity of these issues. Cost-effectiveness analysis typically takes a health-centric approach focusing on just two sets of benefits: the changes in mortality and morbidity and the healthcare cost savings. Moreover, it does not allow for differential socioeconomic benefits across different units of health. For example, if health is measured in quality-adjusted life years (QALYs), cost-effectiveness analysis assumes that each additional QALY has equal value regardless of the characteristics of the individual who enjoys that QALY (e.g. age or income).
Benefit-cost analysis, however, evaluates an intervention by converting all its health and non-health benefits into monetary equivalents and summing them up (Hammitt 2020, Greenstone and Nigam 2020). Unlike cost-effectiveness, benefit-cost analysis can handle differential socioeconomic benefits across different units of health through the definition of individual-specific willingness-to-pay measures. However, because willingness to pay depends on ability to pay, benefit-cost analysis tends to inflate the benefits accruing to wealthy individuals relative to similar benefits accruing to their less wealthy counterparts. In addition, because it attaches the same value to dollars paid by the rich and dollars paid by the poor (i.e. benefit-cost analysis takes an unweighted sum of monetary equivalents), the value of an intervention is independent of whether its cost burden falls on wealthy or less well-off individuals.
An alternative approach to policy evaluation is social welfare function (SWF) analysis (Adler 2019). This method measures the joint health and non-health effects of an intervention on individual well-being and then aggregates individual well-being impacts to obtain an overall measure of the value of the intervention. The aggregation is performed through a social welfare function that can incorporate concerns for the distribution of well-being across the population. Like benefit-cost analysis, social welfare function analysis allows for differential socioeconomic benefits across different units of health. Unlike benefit-cost analysis, it does not necessarily inflate the value of health benefits accruing to wealthy individuals relative to those of less well-off individuals (because the metric of evaluation is well-being and not money), and it is sensitive to the distribution of burdens and benefits across the population (Adler et al. 2014). The method can be seen as a generalisation of benefit-cost analysis. In particular, it is operationally equivalent to an equity-weighted benefit-cost analysis, where the form of the weights depends on the specific social welfare function.
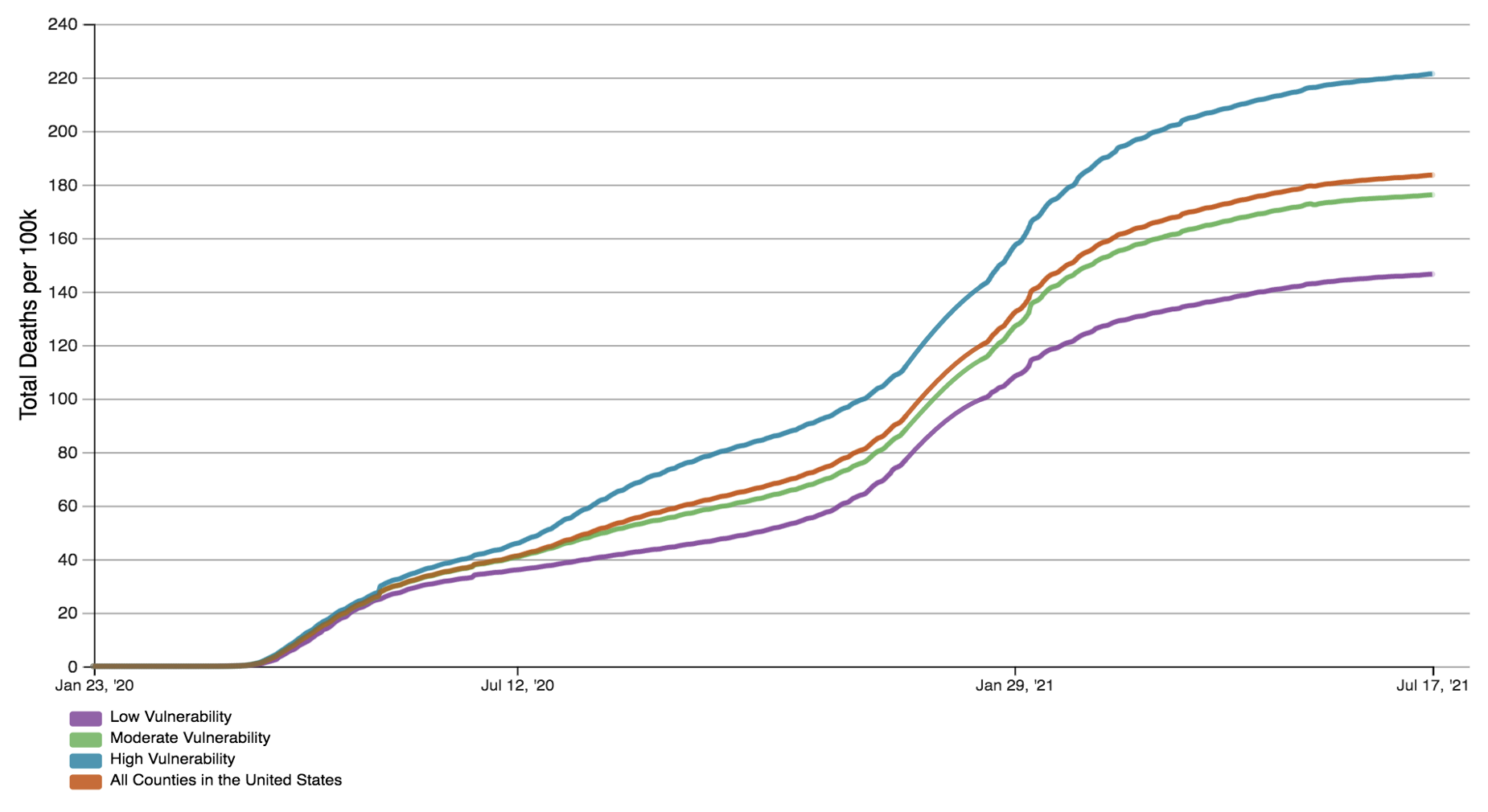
The choice of the value framework for Covid-19 interventions is very consequential (Ferranna et al. 2021). Consider, for instance, the question of whether, how long, and how strictly to impose lockdowns to curb infections. On the one hand, a lax lockdown policy can result in an uncontrolled pandemic. The harms from this tend to be disproportionately borne by the poor and worse off (Figure 2). This may be because their living and working conditions expose them to above average infection risks or because they have less access to quality care when infected. On the other hand, lockdowns themselves impose costs like job and income losses. Such costs tend also to be disproportionately borne by the poor and worse off, who have fewer savings and more limited reemployment prospects, especially in the absence of social safety nets. This is an issue, for instance, in developing countries with lower ability to provide public income support.
Figure 2 Covid-19 cumulative death rate per 100,000 population in the US, by county social vulnerability index value.
Source: CDC, Covid Data Tracker, 19 July 2021. https://covid.cdc.gov/covid-data-tracker/#datatracker-home. The CDC Social Vulnerability Index uses US Census Data to identify communities that are potentially more exposed to the negative effects of external shocks on human health. https://www.atsdr.cdc.gov/placeandhealth/svi/fact_sheet/fact_sheet.html
The optimal stringency and duration of lockdowns then depends on an interaction of empirical and normative issues. A first empirical possibility is that the burdens to the worse off from an uncontrolled pandemic are greater than the burdens to them of a lockdown. In this case, the interests of the worse-off will on net be served by stringent lockdown policy. The second and alternative possibility is that the burdens to the worse-off from a lockdown exceed the burdens to them from an uncontrolled pandemic. In this case, the interests of the worse-off are better served by less stringent lockdowns.
For benefit-cost analysis, the optimal policy is that for which the sum of individual willingness-to-pay (WTP) is highest. Such willingness to pay will reflect both the willingness to avoid the harms of the pandemic itself as well as the willingness to avoid the harms of the policy. But benefit-cost analysis weighs every dollar of willingness to pay equally, even across rich and poor individuals with differential ability to pay. It therefore tends to underweight the interests of the poor and worse off, making it insensitive to the above considerations relative to a social welfare function approach. When the first empirical possibility holds, benefit-cost analysis will suggest a lockdown policy that is too lax in light of equity considerations. And when the second empirical possibility holds, it will suggest a lockdown policy that is too stringent. Across the two empirical possibilities, the worse off fare better under the social welfare function approach than under the benefit-cost analysis approach.
In our work, we study the example of lockdowns whose burdens are disproportionately borne by the worse off and find that, in the US, benefit-cost analysis might support policies that completely eliminate the spread of the infection even if they cause a 30% GDP loss. Social welfare function analysis would find these policies unacceptable if low-income groups pay a disproportionate amount of the net costs. In this scenario, applying plausible levels of inequality aversion, it would recommend only policies that cost at most 10–15% of GDP; the larger the aversion to inequality displayed by the decisionmaker, the lower the support for strict lockdown policies when their costs are regressive.
Vaccine prioritisation is another example highlighting the differences between traditional evaluation methods and social welfare function analysis. Modelling efforts to study the best allocation of vaccines (e.g. Bubar et al. 2021) are usually based solely on epidemiological outcomes (e.g. deaths, years of life lost, or numbers of infections) and, potentially, on the costs of delivering those outcomes. This method neglects issues related to structural inequities (e.g. the recommendation to concentrate vaccinations in socially vulnerable areas), potential economic benefits of alternative vaccination rules (e.g. the link between vaccination and relaxing nonpharmaceutical interventions), and the role of other background characteristics (e.g. the age of the individual). In contrast, a social welfare approach can accommodate concerns for social equity and for the socioeconomic impacts of alternative vaccine allocation strategies.
Suppose, for instance, that the risk of severe Covid-19 outcomes increases with age and decreases with the socioeconomic status of the individuals, e.g. because wealthy people are, on average, better able to shield themselves from the risk of infection or are more likely to get better treatments. Older adults in low socioeconomic groups are the most exposed to the risk of severe outcomes. Let us further assume that the vaccine is very good at protecting the vaccinated individual, but it is not very effective at reducing the risk of transmission. In such a context, if the policy goal is to reduce the number of severe cases, the vaccine would be given first to older adults in low socioeconomic groups and then to older adults in high socioeconomic groups. If the policy goal is to maximise social welfare, older adults in low socioeconomic groups would still be prioritised because of the large risk they face. However, if the social evaluator is sufficiently concerned with social equity, younger adults in low socioeconomic groups would come next rather than older wealthy adults because the former are in a less privileged position from a socioeconomic perspective and because they are relatively younger (i.e. they have not had the chance to live a full life yet) (Adler et al. 2021).
Compared with more traditional methods, the social welfare approach is more data intensive because it requires information on the distribution of different attributes across the population and on the correlations among those attributes, in addition to the distributional effects of the policy on the attributes. Moreover, because social welfare analysis takes a consequentialist perspective, it does not fully capture other ethically relevant issues, such as respect for human rights, the role of individual responsibility versus luck, or the restitution principle. Nevertheless, because the approach accounts for the distribution of policy impacts across the population and the correlation with background inequalities, it is more attractive than traditional methods such as benefit-cost analysis and cost-effectiveness analysis and more consistent with the idea that equity and justice matter in policy evaluation.
References
Adler, M D (2019), Measuring Social Welfare: An Introduction, Oxford University Press.
Adler, M D, J K Hammitt and N Treich (2014), “The Social Value of Mortality Risk Reduction: VSL Versus the Social Welfare Function Approach”, Journal of Health Economics 35: 82-93.
Adler, M D, M Ferranna, J K Hammitt and N Treich (2021), “Fair Innings? The Utilitarian and Prioritarian Value of Risk Reduction Over a Whole Lifetime”, Journal of Health Economics 102412.
Bubar, K M, K Reinholt, S M Kissler, M Lipsitch, S Cobey, Y H Grad and D B Larremore (2021), “Model-Informed COVID-19 Vaccine Prioritization Strategies by Age and Serostatus”, Science 371(6532): 916-921.
Ferranna, M, JP Sevilla and D E Bloom (2021), “Addressing the COVID-19 Pandemic: Comparing Alternative Value Frameworks”, CEPR Working Paper DP15904; fforthcoming in M D Adler and O F Norheim (eds.), Prioritarianism in Practice, Cambridge University Press.
Greenstone, M and V Nigam (2020), “Does Social Distancing Matter?”, BFI Working Paper 2020-26.
Hammitt, J K (2020), “Valuing Mortality Risk in the Time of COVID-19”, Journal of Risk and Uncertainty 11: 1-26.