Many of the characteristics or environments associated with modern daily work life may encourage the transmission of viruses, including seasonal influenza (the flu) and the novel coronavirus (SARS-CoV-2), the cause of Covid-19. These characteristics include commuting via public transportation, working in climate controlled indoor offices, sharing workspaces, and placing young children in daycare. If the features of the working environment promote the spread of the flu and other viruses, then being out of the labour force and away from these environments could help reduce the spread of diseases. This is the premise behind the current public health policies of closing down public places and requiring social distancing.
Early evidence suggests that these social distancing measures may be reducing the spread of SARS-CoV-2 (e.g. Dave et al. 2020, Friedson et al. 2020, Courtemanche et al. 2020, Baldwin and Weder di Mauro 2020). However, because the COVID-19 pandemic is so recent, much of this evidence is based on only a few months of data. More evidence surrounding the effects of social distancing on the spread of SARS-CoV-2 could be gathered by studying the spread of similar viruses, namely the flu.
Evidence that high levels of employment are associated with high rates of seasonal flu
In a recently published article (Markowitz et al. 2019), we examine the relationship between economic activity, as measured by employment levels, and the spread of the flu in the US. We use state-level monthly employment rates from the Bureau of Labor Statistics and state-level monthly estimates of flu activity from the Centers for Disease Control and Prevention, spanning the 2010-2011 flu season up to the 2016-2017 flu season.
Our basic empirical strategy is to predict flu activity in a state and month as a function of the state’s employment levels in the previous month, as well as temperature and precipitation, and the previous month’s flu rate.
If our hypothesis is correct, we should expect that increases in employment in jobs with higher levels of interpersonal contact should be more related to the spread of the flu. Thus, we construct a measure of interpersonal contact levels for each industry sector using data from O*Net and construct employment measures at the industry level using data from the BLS Current Employment Statistics (CES) data set. We find that the two sectors with the highest levels of interpersonal contact are the retail and healthcare sectors, while the sectors with the lowest level of interpersonal contact are the construction and manufacturing sectors.
Results
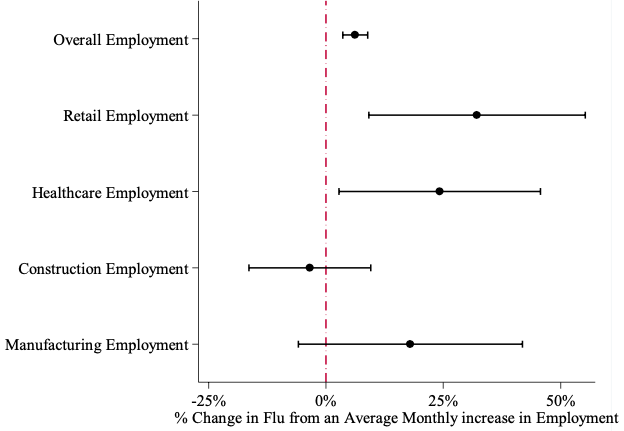
Figure 1 summarise the results from our regression models. We plot the increases in flu prevalence from an average monthly increase in overall employment and employment in sectors with high and low measures of interpersonal contact.
We find a strong positive association between employment and the spread of the flu, and the results suggest that an average monthly change in overall employment (about 0.33 percentage points) increases flu prevalence by about 6%. We find that employment changes in the retail and healthcare sectors, the two sectors with the highest levels of interpersonal contact, drive the aggregate results. The same average monthly increase in retail employment and healthcare employment would lead to much larger expected increases in flu prevalence of between 20% and 30%, respectively. Moreover, we find that employment changes in the construction sector, one of the sectors with the lowest level of interpersonal contact, is not associated with statistically significant changes in flu prevalence. Interestingly, changes in manufacturing employment lead to a large, but extremely imprecisely measured, increase in flu prevalence. This may be due to underlying heterogeneity in how different types of manufacturing employment either aid or are not related to the spread of the flu. We believe this remains an interesting question for future research.
Figure 1 Percent changes in flu prevalence from an average monthly increase in employment
These results are relevant for several reasons. First, barring major economic shocks, employment conditions can be forecast, to a fairly accurate degree, several months in advance. This information could be used by the public health community to plan for the severity of an upcoming flu season. For example, the 2017-2018 flu season was particularly severe. Hospitals found themselves unprepared and struggling to keep up with the influx of patients. As we have recently learned, the ability to predict the potential severity of future communicable diseases is vital information for hospitals and public health officials. In general, if the economy is on an upswing, the public health community should plan for an above normal increase in such diseases. The reverse will hold as well. This same logic can reasonably be applied to other droplet-spread, respiratory diseases, like COVID-19.
Furthermore, our results imply that employment in service industries – particularly retail and healthcare – is a particularly strong mechanism for flu spread. If our economy continues to shift to more service-oriented employment, the results presented here suggest there is greater potential for virus spread in the future. The statistically insignificant findings for industries such as construction with relatively low levels of interpersonal contact support the continuation of construction and infrastructure projects during periods of social distancing. Likewise, restrictions on retail business and non-essential medical visits are prudent considerations, as our results suggest activity in these industries is a significant source of viral infection. Lastly, employers should consider differences in the lost productivity from many employees becoming infected with viruses versus the lost productivity from a few infected individuals taking sick leave. Workers concerned about missing pay or losing their jobs as the result of staying home from work due to illness will be less likely to heed early signs of influenza or other viral infections and stay home. Since a person may be infectious while experiencing mild symptoms, this greatly increases the probability that the virus will spread to other workers in the firm. This implies that firms should consider more generous ‘sick day’ policies, particularly during the flu season. A recent working paper (Pichler et al. 2020) and a corresponding VoxEU column (Pichler and Ziebarth 2020), provide direct evidence of this hypothesis using variation in state-level mandated sick leave policies.
References
Baldwin, R, and B Weder di Mauro (2020), Economics in the Time of COVID-19, A VoxEU.org Book, CEPR Press.
Courtemanche, C J, J Garuccio, A Le, J C Pinkston, and A Yelowitz (2020), "Did Social-Distancing Measures in Kentucky Help to Flatten the COVID-19 Curve?" Working Paper:1-23.
Dave, D M, A I Friedson, K Matsuzawa, and J J Sabia (2020), "When Do Shelter-In-Place Orders Fight COVID-19 Best? Policy Heterogeneity across States and Adoption Time", NBER Working Paper:1-65.
Friedson, A I, D McNichols, J J Sabia, and D Dave (2020), "Did California’s Shelter-in-Place Order Work? Early Coronavirus-Related Public Health Effects." NBER Working Paper:1-86.
Markowitz, S, E Nesson, and J J Robinson (2019), "The effects of employment on influenza rates." Economics & Human Biology 34:286-295.
Pichler, S, K Wen, and N R Ziebarth (2020), "Positive Health Externalities of Mandating Paid Sick Leave." Working Paper.
Pichler, S, and N R Ziebarth (2020), "The pros and cons of sick pay schemes: Contagious presenteeism and noncontagious absenteeism behaviour." VoxEU.org, 12 May.