COVID-19 and the emergence of new variants are a grave threat to public health (Yeyati and Filippini 2021). Effective vaccination deployment is essential to mitigate that risk. Yet, despite widespread awareness and availability of COVID-19 vaccines, many high-income countries are struggling to push vaccination rates beyond 70%. At the core of an effective disease containment strategy lie policies that further increase vaccination rates among the hesitant and among people who intend to get vaccinated but do not follow through (Aksoy et al. 2020, Blanchard-Rohner et al. 2021).
Governments and organisations across the globe have started using incentives to encourage vaccination, ranging from payments of $5 in Vancouver, to lotteries in Ohio, to payments of €150 in Greece. Many others are now considering introducing payments for vaccinations. Notably, US President Biden recently urged “[…] state, territorial, and local governments to provide $100 payments for every newly vaccinated American, as an extra incentive to boost vaccination rates, protect communities, and save lives”. Yet, governments and organisations are limited in their ability to properly assess the impact of monetary incentives because they lack control groups that are not exposed to incentives. Causal evidence examining the effectiveness of introducing payments for COVID-19 vaccinations is lacking.
In a recent study (Campos-Mercade et al. 2021a), we conducted the first experiment (randomised controlled trial, RCT) to study the effect of incentives on vaccination against COVID-19. We recruited 8,286 participants aged 18-49 from a representative sample of the Swedish population, to whom we sent an online survey. We recruited participants right as vaccination began for their age group. Some of the participants were assigned to a control condition, where we simply attached a message saying "we encourage you to get vaccinated in the next 30 days." In the incentive condition, we included the same message and in addition offer participants 200 SEK (about €20) if they got vaccinated within the next 30 days.
In addition to incentives, we study whether we can promote vaccination with three behavioural ‘nudges’ (i.e. interventions in which economic incentives are not modified) (Thaler and Sunstein 2008; Patel, Volpp and Asch 2018). Specifically, in one intervention we highlight the importance of vaccination to protect others (social impact) (Campos-Mercade et al. 2021b, Costa-i-Font 2021); in another, we encourage participants to consider arguments in favour of being vaccinated (argument) (Milkman et al. 2021); and in the last one, we provide information on the effectiveness and safety of vaccines (information). In all these conditions (control, incentives, and the three nudges) we sent two reminders – one two weeks and another four weeks after completing the survey. To study if the reminders have any impact, we include a last intervention where we did not send any reminders (no reminders) (Dai et al. 2021).
After each of the interventions, we asked the participants if they intended to get vaccinated within the next 30 days. In addition, after 30 days, we checked with the Public Health Agency of Sweden if each participant had actually got vaccinated. This helps us to study not only whether incentives and other interventions increase vaccination uptake, but also the possibility of using intentions to study the impact of interventions on vaccination.
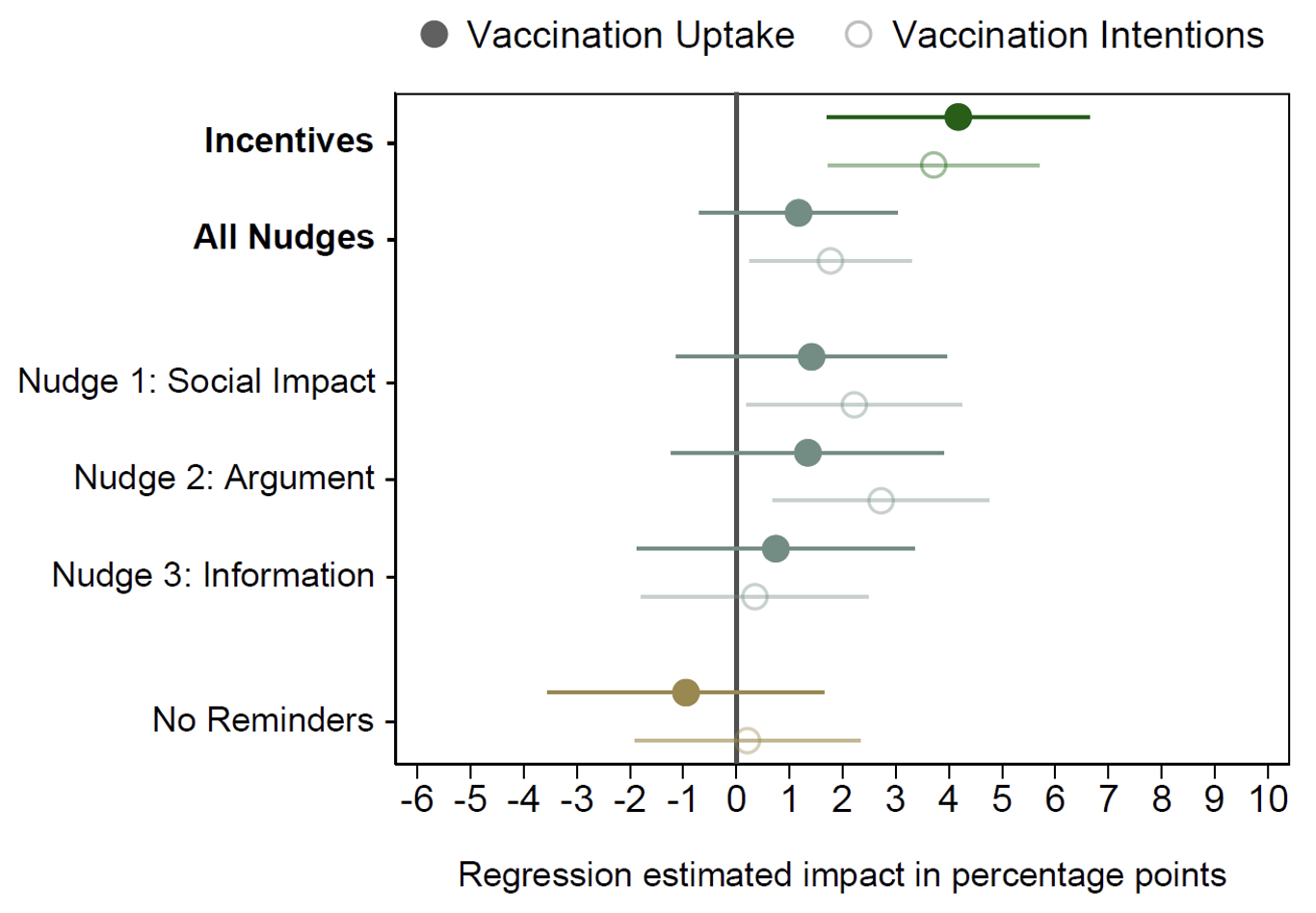
Figure 1 Treatment effects, in percentage points, for each intervention (with its respective 90% confidence interval)
Compared to the control group, the incentive condition increases the proportion of people who vaccinated by approximately 4%. Nudges seem to increase vaccination, but by considerably less than incentives. Reminders (no-reminders Condition) seem to have no effect. Figure 1 shows the estimate of the differences between each intervention and the control condition on both vaccination and the intention to get vaccinated (as specified in the pre-analysis plan). We found that incentives increase the intention to get vaccinated by 3.8% (p = 0.002), and that this increase in intentions translates into an increase in vaccinations of 4.2% (p = 0.005). We found that nudges also seem to increase intentions to get vaccinated (1.8%, p = 0.056), but this does not translate into a significant increase in vaccinations (increase of 1.2%, p = 0.302). In the supplementary materials of our article, we show that we reach the same conclusions by performing the analysis in different ways – for example, analysing other variables (including different sets of controls), correcting for multiple hypothesis tests (including participants who did not complete the survey), and studying vaccination beyond the first 30 days.
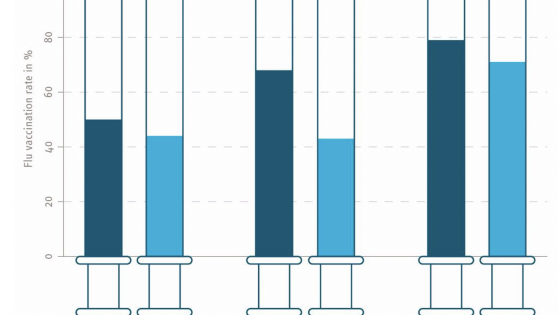
Figure 2 Treatment effects, in percentage points, of incentives for different socioeconomic groups (with their respective 90% confidence interval)
Incentives were the only intervention that resulted in a statistically significant increase in vaccination. In Figure 2, we study whether this increase is different for different sociodemographic groups. It is not – all the sociodemographic groups show very similar increases. This result surprised us since many of these groups have relatively different vaccination rates: 77.8% of people with university studies are vaccinated, while only 66.9% of people without university studies are vaccinated. This finding suggests that incentives can help to increase vaccination in any group, including those socioeconomic groups that are less likely to get vaccinated.
Beyond showing that incentives can help mitigate the risks of the pandemic, our findings are also relevant in the debate over whether monetary incentives can help promote healthier behaviours in general. While monetary incentives have been shown to sometimes encourage healthier behaviour, incentives can often be ineffective or even counterproductive (Gneezy and Rustichini, 2000). Based on this evidence, many argue that paying people to get their COVID-19 vaccinations may signal that vaccination is undesirable or even dangerous, or that it could crowd out peoples’ motivation to get vaccinated to protect others, leading to a decrease in vaccination uptake. In contrast, our results highlight that modest monetary incentives can increase vaccination rates. However, it is important to note that our findings do not imply that we ought to pay people; our paper does not speak to the normative question of whether paying for vaccination is ethically permissible (Jecker 2021).
Our study has several limitations. First, we only tested one size of monetary incentive; our results do not provide any evidence on whether smaller or larger incentives would be more effective. Second, while during the summer of 2021, Sweden had a vaccination rate similar to the EU average, countries differ greatly in the proportion of the population vaccinated, and the effect of incentives could vary according to vaccination rates. Third, monetary incentives could potentially crowd out willingness to get vaccinated in the future (for example, with third doses) without being paid. Finally, people might react differently based on who provides monetary incentives and corresponding trust in receiving the promised payments. In our case, researchers provided incentives, but the effects could differ if incentives were offered by governments or companies.
Despite these limitations, our pre-registered trial yields a clear result: guaranteed incentives can increase COVID-19 vaccinations. As the COVID-19 pandemic continues, incentives could be an effective tool to reduce COVID-19 spread and fatalities.
References
Aksoy, C G, B Eichengreen, O Saka (2020), "Vaccine challenges", VoxEU.org, 16 November.
Blanchard-Rohner, G, B Caprettini, D Rohner, H-J Voth (2021), “From tragedy to hesitancy: How public health failures boosted COVID-19 vaccine scepticism”, VoxEU.org, 01 June.
Campos-Mercade, P, A N Meier, F H Schneider, D Pope, S Meier and E Wengström (2021), “Monetary incentives increase COVID-19 vaccinations”, Science 374(6569): 879-882.
Campos-Mercade, P, A N Meier, F H Schneider, E Wengström (2021b), “Prosociality predicts health behaviors during the COVID-19 pandemic”, Journal of Public Economics 195, 104367.
Costa-i-Font, J (2021), “Social value and incentives for vaccine uptake”, VoxEU.org, 29 June.
Dai, H, S Saccardo, M A Han, L Roh, N Raja, S Vangala, H Modi, S Pandya, M Sloyan, D M Croymans (2021), “Behavioural nudges increase COVID-19 vaccinations", Nature 597: 404–409.
Gneezy, U and A Rustichini (2000), "Pay enough or don’t pay at all", Quarterly Journal of Econmics 115: 791–810.
Jecker, N (2021), “Cash incentives, ethics, and COVID-19 vaccination”, Science 374(6569): 819-820.
Milkman, K L et al. (2021), "A megastudy of text-based nudges encouraging patients to get vaccinated at an upcoming doctor’s appointment", PNAS 118, e2101165118.
Patel, M S, K G Volpp and D A Asch (2018), "Nudge units to improve the delivery of health care", New Engand Journal of Medicine 378: 214–216.
Thaler, R and C Sunstein (2008), Nudge: improving decisions about health, wealth, and happiness, Penguin Books.
Yeyati, E L and F Filippini (2021), “Pandemic divergence: The social and economic costs of Covid-19”, VoxEU.org, 12 May.