The current policy to combat COVID-19 in the Netherlands aims at reducing the number of infections as much as possible, like in many other OECD countries. The government states as its objective to reduce the number of infected persons from its peak of 10,000 per day around 25 October beyond the current 5,000 per day to much lower numbers. In this column, we question the wisdom of this policy.
When the first wave of COVID-19 hit, policymakers all over the world had to take far-reaching decisions based on limited information, mainly from China. Across the EU, countries have been quite effective in simultaneously containing the spread of the virus with lockdowns, while providing liquidity support to firms and social assistance to workers that were hit hardest by these lockdowns. Since we are now in the middle of the second wave, we have to consider the best way to move forward from our current state, which is entirely different than in East Asia.1
There are essentially three strategies in responses to contain the pandemic (Britton et al. 2020, Acemoglu et al. 2020):
- The first strategy is to attempt to eradicate the virus altogether, as China successfully did in response to 2002-2003 outbreak of SARS. This virus eventually became extinct by strictly isolating all infected persons.
- The second strategy is the exact opposite of the first – let the virus roam freely in the population to achieve herd immunity as quickly as possible and accept the casualties as the inevitable cost. This strategy is used routinely in response to the annual waves of the flu virus.
- The third strategy is to strictly contain the spread of the virus among vulnerable subgroups of the population whose health is severely affected by a COVID-19 infection, thereby avoiding excess casualties and overburdening the healthcare system, while waiting for either a vaccine or herd immunity to end the pandemic.
Since the second strategy is not considered an option by Dutch policy makers for the COVID-19 crisis, we focus on the first and third. Reducing the number of infections is consistent with the first strategy, while it is a waste when pursuing the third. The third strategy limits the number of susceptible persons by achieving herd immunity. As long as vulnerable subgroups can be isolated, infections for the remaining population aren’t a problem. Infections accelerate achieving herd immunity, thereby reducing the time that the vulnerable subgroups are exposed.
The difference in the role of infections in both strategies can be phrased in terms of externalities. In the first strategy, an infected person imposes a negative externality on the rest of the population by being a source of further infections. This negative externality justifies government-imposed lockdown policies to internalise the externality. In the second strategy, an infected person imposes a positive externality on the population, by being immune after infection and hence contributing to a protective wall against further contagion. Counterintuitively, the government may even have to stimulate infections among the less vulnerable subgroups of the population. Ignoring this third strategy of a selective lockdown explains why Alveda et al. (2020) conclude that a strict lockdown is the only way forward for Europe and the US.
Four parameters are critical for the choice between both strategies:
1) The number of infected persons – the higher this number, the further the first strategy gets out of reach
2) The ratio of casualties to infected persons – the lower the infection fatality rate, the lower the number of casualties during the transition-period towards herd immunity
3) Heterogeneity in vulnerability by age and pre-existing medical conditions – the sharper the distinction, the better the prospects of isolating the vulnerable subgroups
4) The likelihood that there will be a working vaccine and the expected time lag until a sufficient supply will be available – the higher the likelihood, the lower the benefits of achieving herd immunity.
A comparison of the first and second wave reveals a strong shift in the first two parameters in favour of the third strategy (see Table 1). The number of positive tests per day is nine times higher at the peak of the second wave, and this increase is heavily concentrated among youth. However, the number of positive tests is a bad proxy for the real spread of the virus, since testing was limited during the first wave. The second line therefore reports the number of people with antibodies against the virus. Though less pronounced than the first line, these data exhibit a similar pattern. In contrast, the number of people in intensive care and the number of casualties is only half as high in the second wave compared to first. Moreover, if anything, the number of casualties has become even more skewed towards the elderly.
Table 1 Ratio of peak second relative to first wave for a number of statistics
Source: https://www.rivm.nl/pienter-corona-studie/resultaten
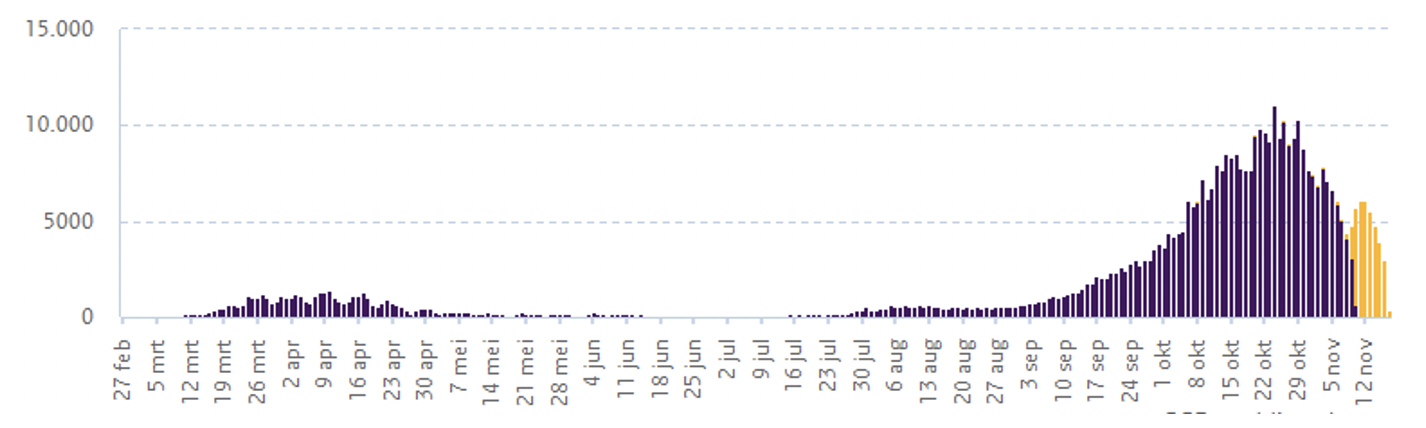
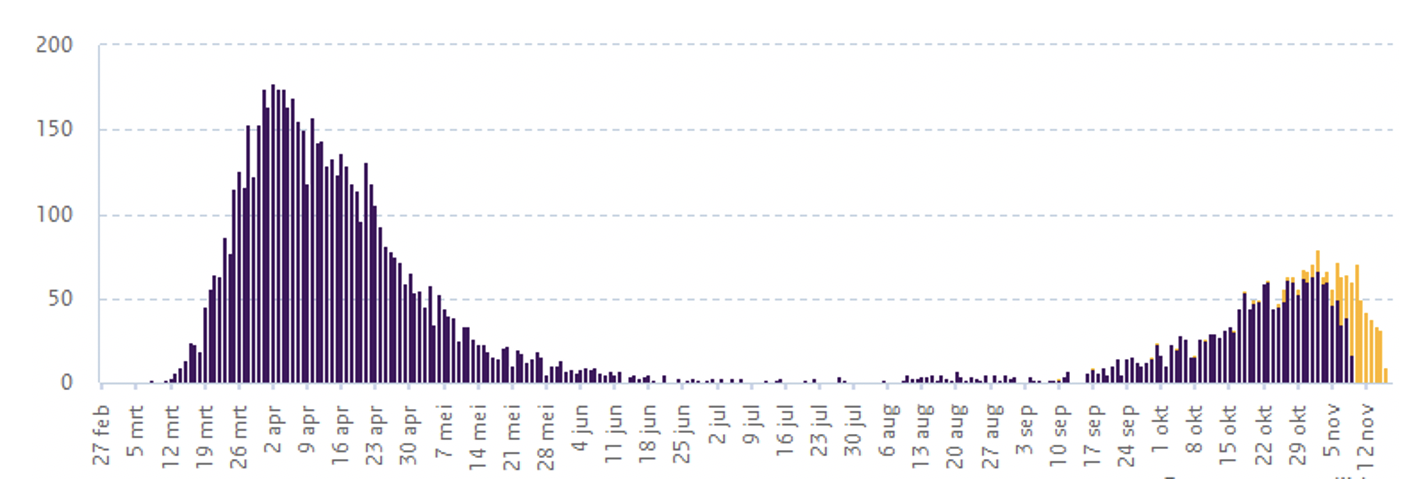
Figure 1 Numbers of positive test, hospitalized patients and casualties from the Dutch National Institute for Public Health and the Environment (RIVM)
a) Positive tests
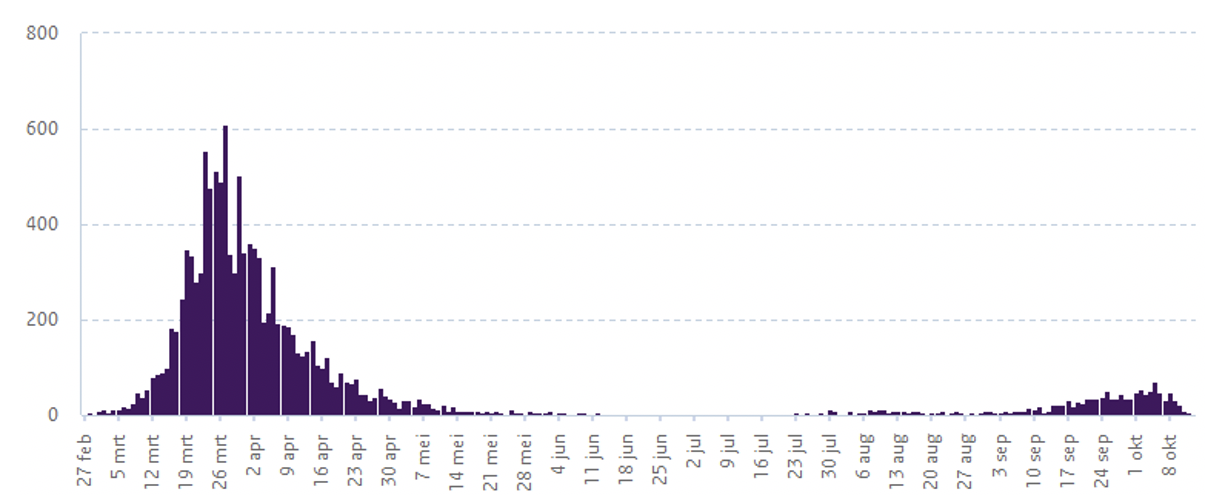
b) Hospitalized patients
c) Hospitalised patients (alternative series)
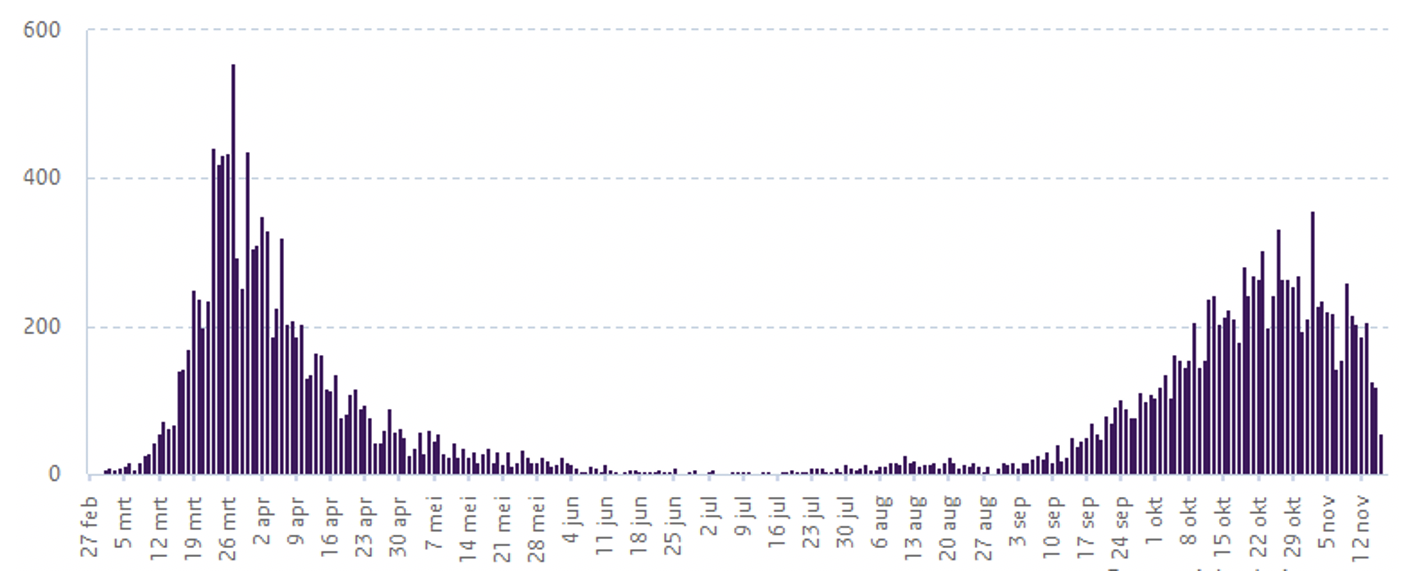
d) Casualties
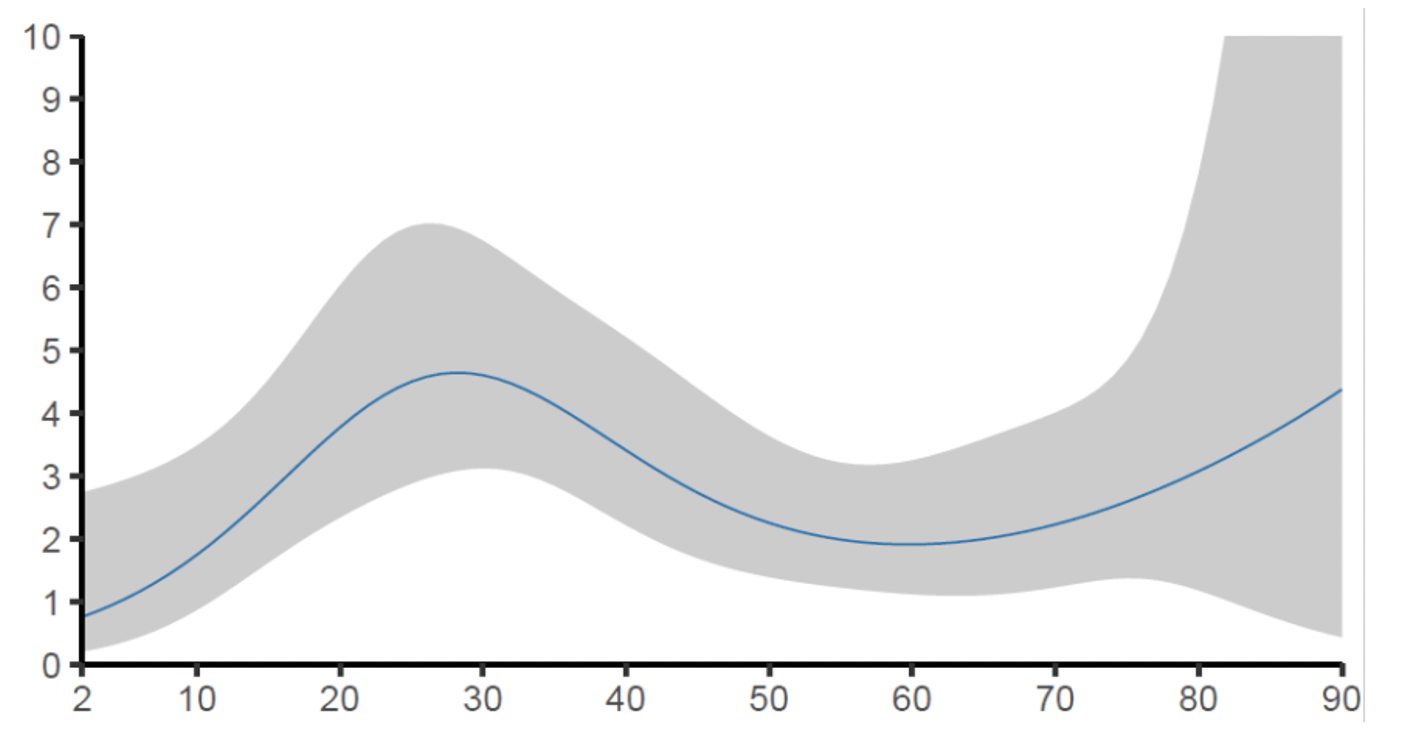
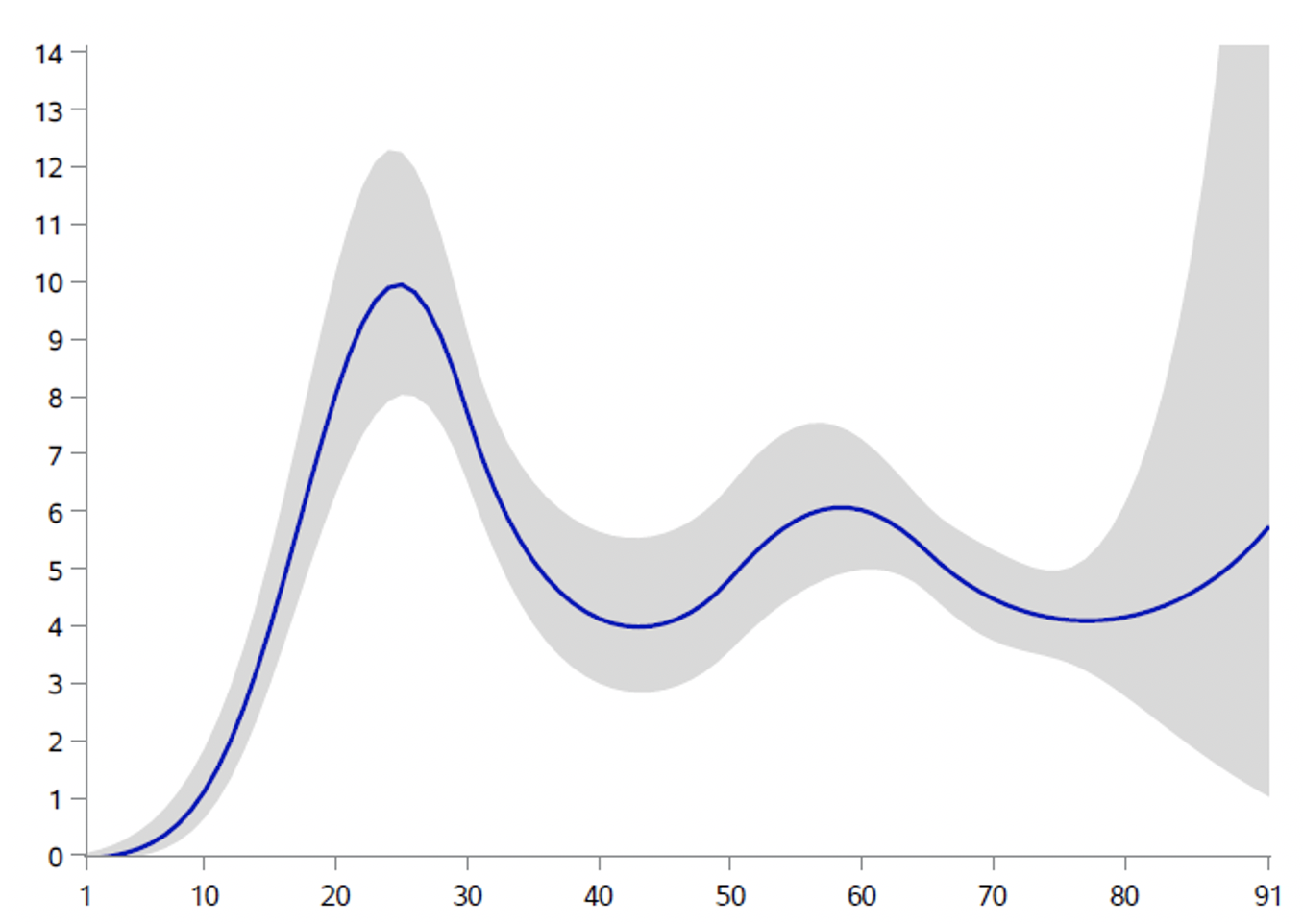
Figure 2 Age distribution of people with corona antibodies
a) As measured in April/May 2020
b) As measured in September/October 2020
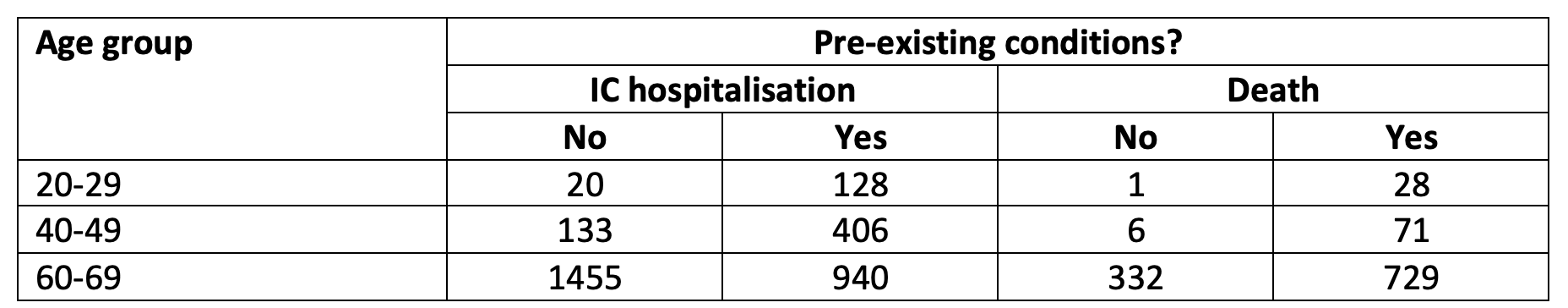
Table 2 provides evidence on the third critical parameter – the degree of heterogeneity in the vulnerability of various subgroups of the population, both in terms of the risk of intensive care (IC) hospitalisation and death. The casualty risk differs by a factor of 700 between young people without pre-existing medical conditions and elderly people with pre-existing conditions.
Table 2 Age-specific risks on intensive care hospitalisation and death (per 100,000 persons)
Source: https://esb.nu/blog/20059630/de-60min-economie-is-beter-dan-de-1-5meter-economie
These numbers are revealing. Apparently, the elderly, who are much more vulnerable, have taken stronger precautionary measures to avoid infections than the youth, with good reason. In the first strategy, one should blame the youth for not taking their social responsibility seriously and ignoring the negative externality they impose on the elderly. In the third strategy it is the opposite, since their immunity after infection helps containing the spread of the virus among elderly.
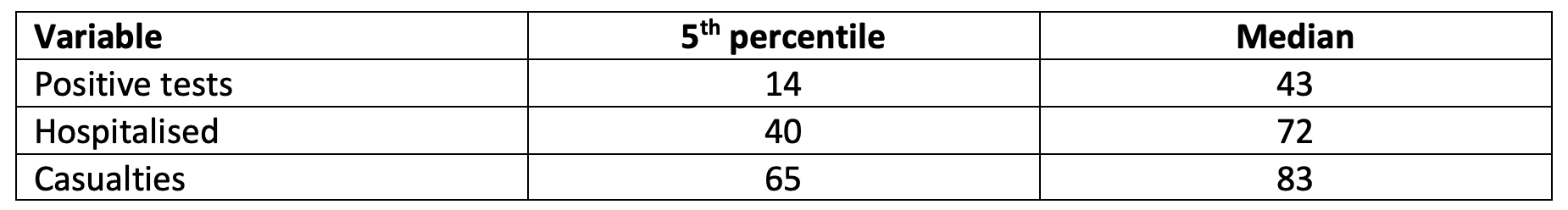
Table 3 provides further evidence on this: the median age of a positively tested person is 43, the median age of hospitalised persons is 72 years, and that of casualties is 83 years. We also calculated the 5th percentile of these age distributions. Few people end up in hospital with a COVID-19-infection below the age of 40, and few die below the age of 65. Age is merely a proxy for pre-existing conditions such as obesity and vascular and lung diseases, which are highly correlated with age. Interestingly, this is not the impression one gets when viewing daily discussions on the COVID-19 outbreak in the Dutch media. There are frequent stories on the severe consequences of COVID-19 infections even for youngsters, also by medical specialists. These cases are exceptional.
Table 3 Age distribution COVID-19 cases on 17 November 2020
Source: https://www.rivm.nl/sites/default/files/2020-11/COVID-19_WebSite_rapport_wekelijks_20201117_1237.pdf
Note: Hospitalised numbers based on the Dutch National Institute for Public Health and the Environment (RIVM) Weekly Report of 20 October. RIVM stopped publishing these numbers in subsequent reports. Numbers on positive tests and casualties are not much different whether calculated from the Weekly Reports of 17 November or 20 October 20. We suspect that the numbers for hospitalised patients aren’t much different either.
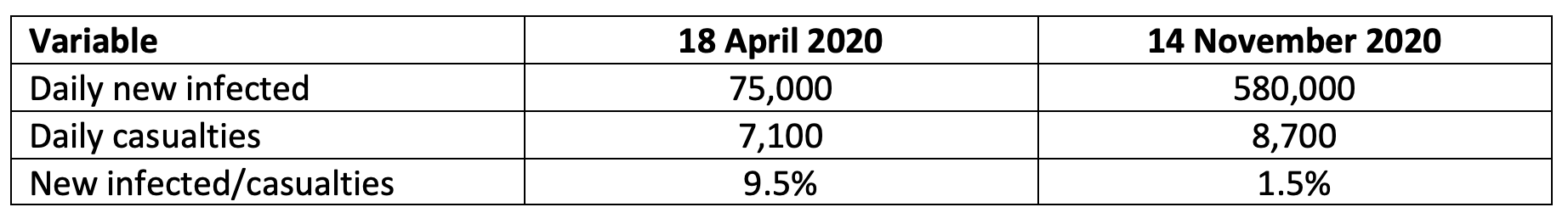
Table 4 shows that worldwide statistics exhibit a similar pattern. The worldwide peak of the first wave was reached around 18 April. The world as a whole hasn’t reached the peak of the second wave, so we use the most recent numbers. Again, the daily number of newly infected people has skyrocketed; the number of casualties hasn’t increased much.
Table 4 Worldwide statistics
Source: https://www.worldometers.info/coronavirus/
The current experience suggests that it is becoming increasingly difficult to contain the number of new infections. A new package of restrictions (closing down bars and restaurants and tighter constraints on group sizes at family events) announced in the Netherlands in mid-October have reduced the number of new infections from 10,000 to fewer than 5,000 per day by mid-November. However, in the meantime, the number of infections is rising again. If the current policy of containing the number of infections is continued, stricter measures will be required.
The rise in infections is partly due to policy fatigue among the population. However, it is also an endogenous response, since infection rates among subgroups are heterogeneous. Initially, the majority of COVID-19-infections came from a broad middle group with moderate infection rates. Mild policy measures have reduced their infection rate such that their reproduction rate R got below one. However, as time goes by, infections in subgroups with high infection rates, which are less likely to strictly follow lockdown restrictions (for example, due to language barriers or because they don’t follow the news), start dominating the total number of infections if the exponential growth rate of infections in these subgroups outpaces that in the broad middle group. It requires increasingly costly measures to bring the R of these high infection-rate groups below unity. Therefore, heterogeneity in infection rates provide another argument to strive for herd immunity. Indeed, Britton et al. (2020) show that herd immunity might even be reached when just 40% of the population is immune to the virus due to this heterogeneity.
This evidence casts serious doubts on the efficacy of the Dutch government’s current policy. The government states as its objective that it wants to reduce the number of infections from its peak of 10,000 persons per day around 25 October 25, beyond its current value of 5,000 persons per day, to much lower numbers.2 The question is: what goal is served by this policy objective? On the one hand, the soaring number of infections and the relatively mild impact on the number of casualties suggest that herd immunity can be achieved within a reasonable amount of time. On the other hand, the increasing difficulty in keeping the number of new infections down by further restrictions suggests that there is no alternative to herd immunity until a vaccine becomes available in sufficiently large numbers.
Our ambition is not to provide a full-fledged social cost-benefit analysis. Such an analysis would require a proper, well-defined baseline scenario for what would have happened without policy interventions. We simply have no realistic way of addressing this question.3 Instead, we provide some numbers to put the cost of the current policy strategy into perspective.
First, the impact of COVID-19 on life expectancy is small. For the age group between 75 and 85, whose life expectancy has been most affected, the effect on the life expectancy at birth is only one to two weeks.4 The secular increase in our life expectancy at birth, enabled by the unprecedented improvement in our prosperity since WWII, is about five weeks per year. COVID-19 costs the most severely affected generations therefore one third of the annual improvement in life expectancy.
Second, the risk of prolonged recessions due to a second or even third wave of lockdown policies is substantial. The cost of such recessions can be large and long lasting (De Long and Summers 2012). Moreover, recessions also generate substantial long-term health costs. Sullivan and Von Wachter (2009) and Schwandt et al. (2020) have shown this for the US. For example, people who entered the labour market during the deep recession in 1982 were less likely to marry and to have children and more likely to divorce. They suffer from ‘illnesses of despair’ – lung cancer, liver disease, and drug addiction. Their life expectancy was negatively affected by between six and nine months, much larger than the effect of COVID-19 for the age group between 75 and 85. One might presume that these costs are smaller in the EU than in the US, due to the more extensive European welfare state. However, these number are instructive to put the cost of COVID-19 into perspective. COVID-19 turns out to yield a similar cost in terms of lost life years as a recession with an increase in the unemployment rate of between 1.5 and 2% percentage points.5
Third, the importance of education for almost all aspects in life – wellbeing, life expectancy, earnings capacity, crime, social behaviour – has been well documented. The cost of interruptions in the education process are therefore substantial. Paechter et al. (2015) have shown that a nine-week holiday has measurable negative effects on test scores (see also Stewart et al. 2018). Engzell et al. (2020) document that the 8-week closure of Dutch schools during the first wave cost the average student 20% of a year’s worth of learning. The suggested lockdown policy to prolong the Christmas holiday by one week is therefore costly.
Fourth, the healthcare system is currently operating under severe stress. One wonders what the most important explanation for this stress is – COVID-19 itself or the lockdown policies to counter it? Since the number of casualties at the peak of second wave was about half that of the first wave (see Table 1), casualties alone can hardly offer a full explanation for the stress on the system. There is substantial sick-leave among nurses and doctors due to the lockdown restrictions and isolation rules. The economic costs of the lockdown are measured not only in lost profit, but also in a lower capacity of the healthcare system.
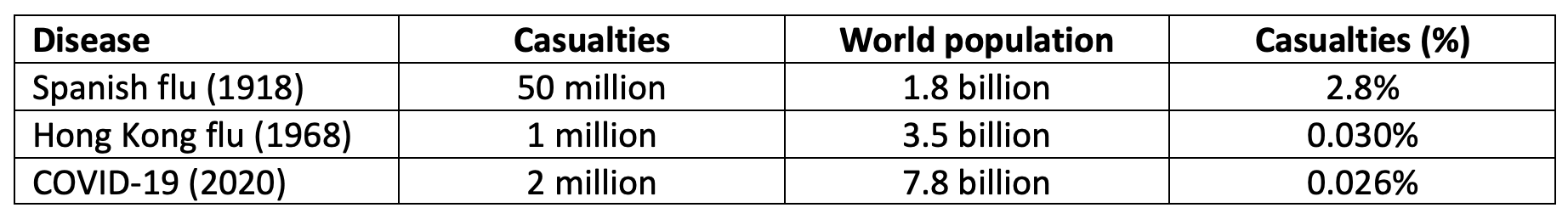
Finally, Table 5 compares the worldwide number of casualties, both in absolute numbers and relative to total population, of the COVID-19 pandemic, the Spanish flu pandemic in 1918 and the Hong Kong flu in 1968. The numbers for COVID-19 are comparable to the Hong Kong flu, but much lower than the Spanish flu. Nevertheless, the policy response to the latest pandemic has been unprecedented.
Table 5 Casualties of Spanish flu (1918), Hong Kong flu (1968) and COVID-19 pandemics (2020)
Source: https://www.cdc.gov/flu/pandemic-resources/1918-pandemic-h1n1.html#:~:text=It%20is%20estimated%20that%20about,occurring%20in%20the%20United%20States
As a final note, government policy should be evaluated not only on its direct impact, but also on the broader effect of government communication of COVID-19-policy. One lesson of the Great Recession was that austerity was not expansionary and that announcements of more austerity did not inspire confidence, but rather destroyed it. Although exaggerating the dangers of an uncontrolled pandemic might help to raise the social acceptance of lockdowns and to improve the following of regulations, creating an atmosphere of imminent doom may do severe harm to consumer and business confidence and thereby kill economic activity in the long run.
In conclusion, since COVID-19 has spread widely across Europe and the US, we no longer have any chance to eradicate it; we shall have to live with it. The good news is that recent data have shown that we can handle a much larger number of infections without excessive social cost. Dutch COVID-19 policy should therefore move away from controlling infections towards creating herd immunity by letting the COVID-19-virus roam freely among the non-vulnerable groups, while strictly protecting the vulnerable groups. Currently, a daily number of infections of 8,000 (about 0.05% of the population) would seem to strike a proper balance between keeping the cost of lockdown policies manageable and speeding up the process of achieving herd immunity.
References
Acemoglu, D, V Chernozhukov, I Werning and M D Whinston (2020), “A multi-risk SIR model with optimally targeted lockdown”, NBER Working Paper No. w27102.
Cooper, H et al (1996), "The effects of summer vacation on achievement test scores: A narrative and meta-analytic review", Review of Educational Research 66(3): 227-268.
Alvelda, P, T Ferguson and J C. Mallery (2020), “To Save the Economy, Save People First”, Inet blog.
Britton, T, F Ball, and P Trapman (2020), "A mathematical model reveals the influence of population heterogeneity on herd immunity to SARS-CoV-2”, Science 369(6505): 846-849.
https://science.sciencemag.org/content/369/6505/846
DeLong, J B, and L H Summers (2012), “Fiscal Policy in a Depressed Economy”, Brookings Papers on Economic Activity, 233-97.
Engzell, P, A Frey, and M D. Verhagen (2020), “The Collateral Damage to Children’s Education During Lockdown”, VoxEU.org, 9 November.
Fransman, R, X Koolman, E-J Vlieger and A Sipkema (2020), “De 60min-econom leidt tot betere resultaten dan de anderhalvemetereconomie”, ESB, 27 May.
Paechter, M et al. (2015), “The effects of nine-week summer vacation: losses in mathematics and gains in reading", Eurasia Journal of Mathematics, Science and Technology Education 11(6): 1399-1413.
Schwandt, H and T M von Wachter (2020), “Socioeconomic decline and death: Midlife impacts of graduating in a recession”, NBER Working Paper No. w26638.
Stewart, H, N Watson, and M Campbell (2018), "The cost of school holidays for children from low income families", Childhood 25(4): 516-529.
Sullivan, D, and T Von Wachter (2009), "Job displacement and mortality: An analysis using administrative data", The Quarterly Journal of Economics 124(3): 1265-1306.
Endnotes
1 The numbers in Germany have also been exceptional, but recently this exceptionalism has faded away, as German numbers seems to adapt to the common pattern in Europe and the US.
2 The cabinet is not exactly clear about its target. Early on, a target of 1,200 infections per day was quoted, but more recently the cabinet mentioned a target of 3,600.
3 Two recent studies published in the Dutch economics journal ESB quoted zero and 450,000 casualties, respectively. Both numbers seem to be highly unrealistic.
4 The share of this group among casualties (35%) x the estimated eventual total number of casualties (20,000) x the remaining life expectancy (5 years). The latter number is obtained by observing that roughly 50% of the casualties are among people living in elderly homes (see https://atosborne.nl/artikel/ontwikkeling-verblijfsduur-verpleeghuizen/). The unconditional life expectancy at age 83 (the median age among casualties) is 7.5 years, the life expectancy conditional on living in an elderly home is 2.5 years. Dividing by the total population born between 1935 and 1945 (the birth years of the age group 75-85; 1.9 million) yields 1.7 week.
5 Lost life years for 1%-point additional unemployment:
For entrants: effect on life expectancy of entrants during the 1982 recession (8 months) / excess unemployment in 1982 (4%) / length career (40 years) = 0.25 week for the workforce as a whole (Schwandt et al., 2020).
For layoffs: layoff as a share of unemployment (25%, see BLS data) x effect on life expectancy (1 year) x excess unemployment 1% = 0.1 week (Sullivan et al. 2009) (see https://www.bls.gov/news.release/empsit.t11.htm).
Cost of 1% additional unemployment: 0.35 week x labour supply (9.2 million) = 3.2 million weeks
Cost of COVID-19: 1.7 week x born between 1935 and 1945 = 3.2 million weeks.
Weeks below 75 and above 85 = 3.0 million weeks.
The final line adds the loss of life expectancy for casualties below 75 (10% x 10 years) and above 90 (50% x 2 years). Formally, the cost of future lower life expectancy should be discounted, in particular for the cost of recession, which falls for a large part in the far future. We ignore discounting.