Despite the widespread accessibility of free and effective COVID-19 vaccines, many Americans still hesitate or refuse to get one. As of September 2022, the proportion of US individuals who were fully vaccinated was just above two-thirds (67.7%), while those who had received a booster shot were just under one-third (32.9%).
Unvaccinated individuals give various reasons for their reluctance, including health, moral, religious, or scientific motivations. Regardless of the impetus, their unvaccinated status leaves them more vulnerable to infection and at greater risk of spreading the disease to others.
The phenomenon of vaccine hesitancy is not a uniquely American problem, of course, nor is it related only to COVID-19 vaccines; it is a pressing global health challenge. In 2011, SAGE (the WHO’s Strategic Advisory Group of Experts) established the Working Group on Vaccine Hesitancy, and the WHO declared vaccine hesitancy as one of the ten leading threats to global health in 2019 – before COVID-19 had become a global pandemic. Political polarisation, the decline in trust in expertise and authority, and the increased relevance of social media platforms have amplified questioning and reluctance to accept vaccination (Larson et al. 2022).
Both monetary and nonmonetary measures have been proposed to increase COVID-19 vaccine uptake, including lotteries, vaccine mandates, and improved messaging. The relative effectiveness of these measures has been the subject of much debate. Analyses of a conditional cash lottery in Ohio found that its impact on COVID-19 vaccine adoption was minimal at best (Barber and West 2022, Walkey et al. 2021). Financial rewards have been shown to have a small positive impact on vaccination rates. For example, Campos-Mercade et al. (2021) found that a financial incentive of 20 USD increased COVID-19 vaccination rates by roughly 4% in Sweden. However, sometimes they backfire (Chang et al. 2021) because they are perceived as a bribe or as a signal that the vaccine is ineffective or unsafe. Mandatory COVID-19 certification to access public venues, workplaces, and nonessential businesses seem to be more effective at increasing vaccination, but it raises personal freedom concerns (Karaivanov et al. 2021).
Communication, especially from trusted healthcare professionals, is often considered key to combating vaccine hesitancy (Larson et al. 2022), although it can also trigger unexpected negative consequences. For example, see Deiana et al. (2022) on the slow-down of vaccination rates after the Italian National Medicines Agency suspended the AstraZeneca vaccine for four days over worries about an extremely rare thrombotic thrombocytopenia among recipients. Altruistic messaging – defined as protecting the health of people you come in contact with, protecting the health of people in your country, and protecting the economy – seems to result in increasing vaccination rates (Galasso et al. 2022). But, again, there is disagreement on the effectiveness of behavioural nudges (Campos-Mercade et al. 2022).
In a new paper (Bennett et al. 2022), we further investigated the factors underlying COVID-19 vaccine hesitancy in the US and the efficacy of various incentives to expand uptake. We used nationally representative survey data on 3,497 US adults collected online over six weeks starting in September 2021. We examined both monetary incentives (such as gift cards or the chance of winning a lottery) and workplace disincentives (like increased healthcare costs or employers’ vaccine mandates), as well as the disincentive of the emergence of more transmissible and dangerous disease variants.
We divided respondents into three categories: (1) partially or fully vaccinated, (2) hesitant or undecided, and (3) unwilling to get vaccinated. Overall, 67.6% of the sample were partially or fully vaccinated, while 18.3% of our respondents were undecided and 14.1% were unwilling. Only 60.2% of our fully vaccinated respondents reported an intention to get the booster shot. Results from multinomial logistic regression models found that hesitancy and refusal were the greatest among those who expressed a lack of trust either in government or in the vaccine’s efficacy, among people who believed that their health was in God’s hands, and among Black individuals, non-Democrat, and rural residents (the last perhaps in part due to poorer access to healthcare services).
Most notably, hesitancy and refusal were the lowest among those who typically get a flu vaccine. While just 10.5% of those age 25+ who received annual flu shots did not get vaccinated for COVID-19, almost half (48.2%) of those who did not get flu shots were not vaccinated for COVID-19. The relationship between flu vaccine uptake and COVID-19 vaccine uptake merits further investigation and presents the intriguing possibility of establishing a robust public health campaign to build confidence in the safety and efficacy of flu vaccines to normalise and nurture vaccination habits.
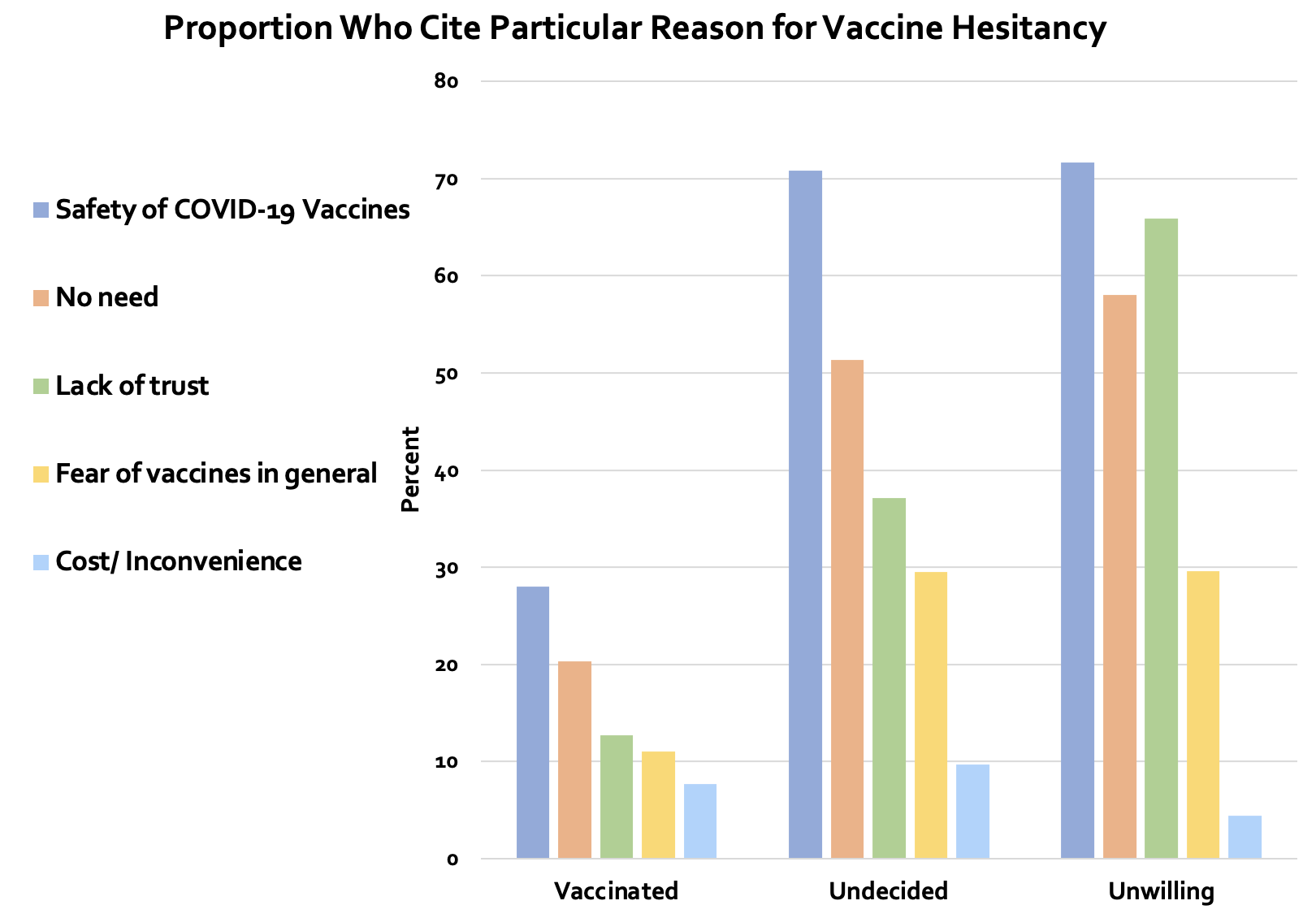
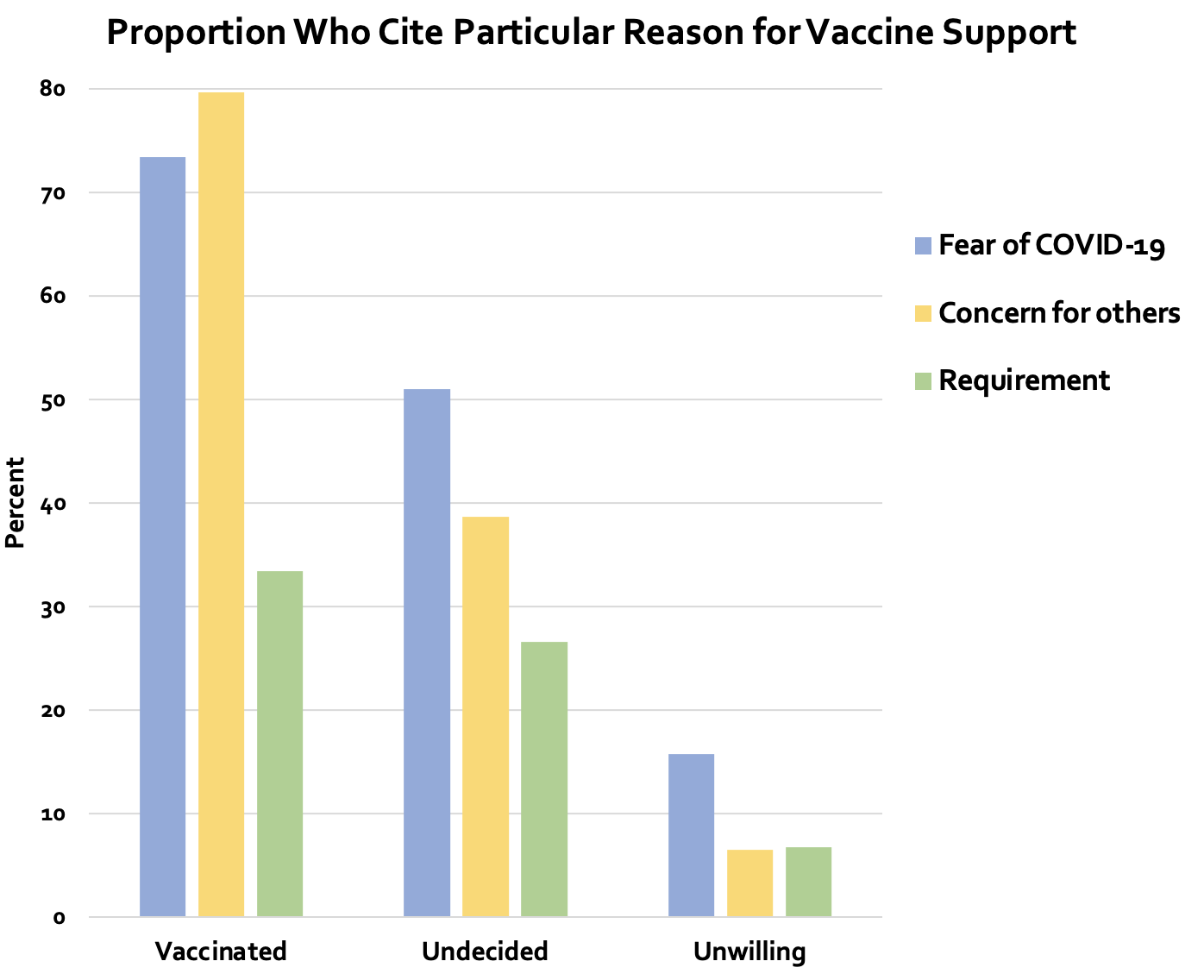
To better understand the reasons underlying vaccine hesitancy and acceptance, we asked respondents why they had or had not been vaccinated (Figure 1). Some unvaccinated people perceived themselves as being at low risk, while others refused because they did not trust the government and/or healthcare system. Among those who were vaccinated, the most cited reason for supporting vaccine uptake was akin to the altruistic messaging found in previous literature (Galasso et al. 2022), namely their concern for others: 79.7% compared with 24.7% of the unvaccinated. Regardless of vaccination status, concern over the safety of COVID-19 vaccines was the most cited reason for hesitancy. About 70% of the unvaccinated cited safety fears of the COVID-19 vaccines as a reason for their status, while roughly 30% were afraid of vaccines in general; almost 40% of those who were uncertain cited a concern for others as a reason to consider getting vaccinated. These findings suggest the potential for improved vaccine uptake and add to the literature that favours enhanced, targeted messaging from government and health officials.
Figure 1 Vaccine hesitancy/acceptance by type of reason and vaccination status (%)
Notes: For each vaccination category (partially or fully vaccinated, hesitant or undecided, and unwilling), the height of the bars represents the (weighted) percentage of respondents who select a particular reason.
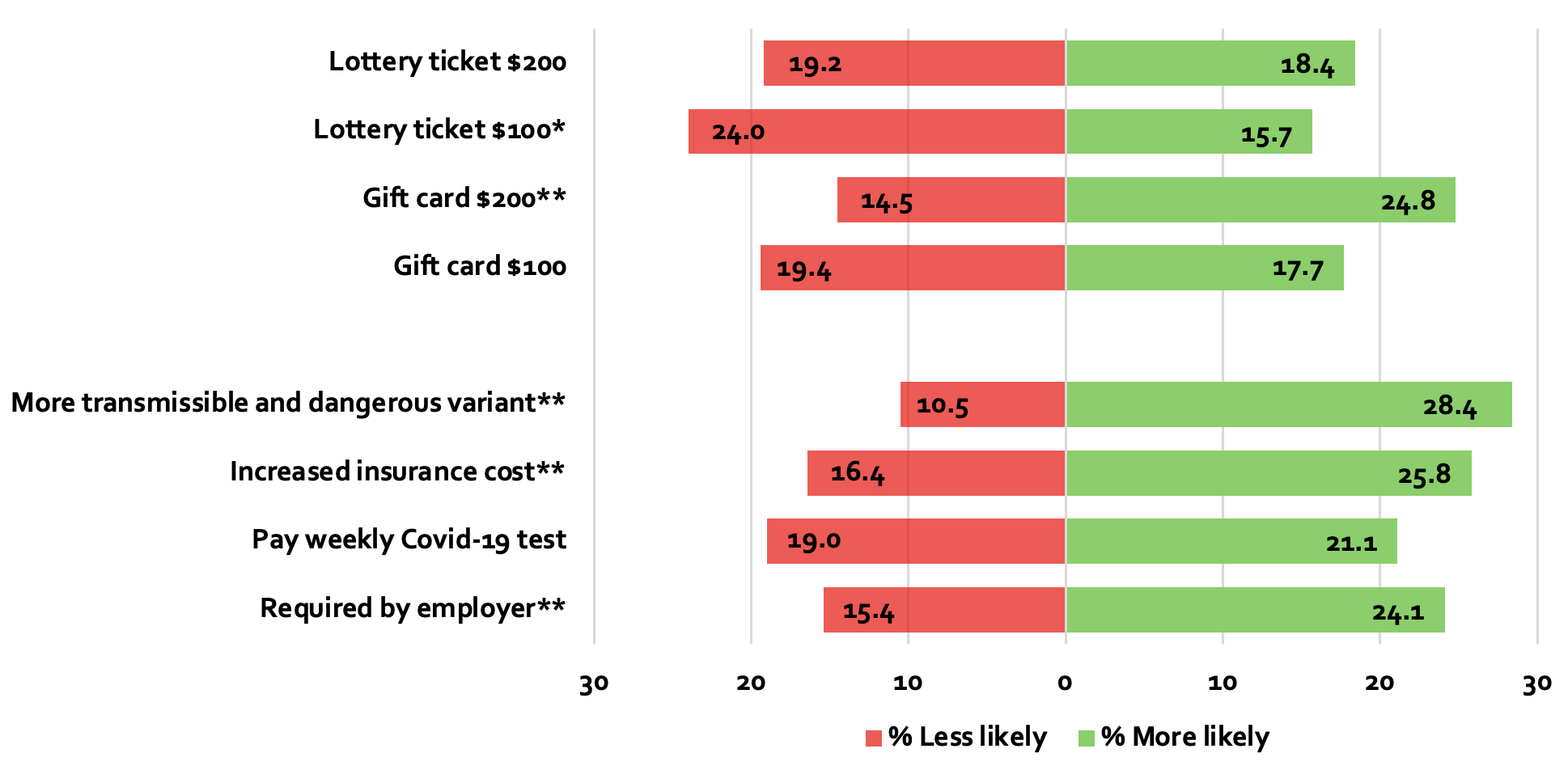
Among the set of incentives to foster vaccination, we found that net movement – the proportion toward vaccination minus the proportion away from vaccination – in response to monetary rewards (i.e. cash lottery and gift cards) was modest (Figure 2). Only the offer of a $200 gift card had a significant net impact on the willingness to vaccinate, though implementing such a measure would introduce practical and moral quandaries. In addition, as some of the literature already stresses, the prospect of winning a lottery has no substantial impact on intentions to get vaccinated. If anything, the chance of winning the lottery might reduce the willingness to get vaccinated (net change with a $100 ticket is -8.3 percentage points).
Figure 2 Change in willingness to be vaccinated compared with the baseline (%) among unvaccinated individuals
Notes: Each bar denotes the percentage of unvaccinated individuals who are more or less likely to get vaccinated in the incentive scenario compared with the baseline. To avoid response randomness, we excluded unvaccinated individuals who were in the bottom 10% and in the top 10% of the distribution of time to take the survey. That is, we excluded those who may not have taken the survey seriously enough (short duration) or who may have suffered from survey fatigue (long duration). Number of observations = 773. The values of the lottery ticket and of the gift card were randomly assigned across the respondents (although respondents were exposed to the same amount in the lottery question as in the gift card one). Number of observations with $100 gift card/lottery ticket = 385; number of observations with $200 gift card/lottery ticket = 388. Weighted results. Table 8 in S1 shows the figures. Table 9 in S1 shows the results of t-tests that assess whether net movement (i.e., the proportion toward vaccination minus the proportion away from vaccination) differs significantly from zero. ** The significance test is accepted at the 1% level. * The significant test is accepted at the 5% level.
We did find, however, that the stick is more effective than the carrot: the threats of potential harm resulted in a significant net increase in willingness to get vaccinated. The prospect of a more transmissible and dangerous variant increased willingness to get vaccinated by 17.9%; an employer vaccine mandate, which could imply job loss for noncompliance, led to a net increase in the probability of vaccine uptake of 8.7%; and a hypothetical $200 per month increase in health insurance premium increased the willingness by 9.4%.
Our analysis finds that among those who currently are hesitant or refuse to vaccinate, a core exists who will not be swayed, regardless of incentives or disincentives. However, a significant proportion of unvaccinated individuals can, in fact, be motivated to vaccinate, particularly if workplace disincentives are in place, namely the prospect of job loss or increased health insurance premiums for those who choose to remain unvaccinated. Further, our data hints at the possibility that efforts to increase acceptance of flu vaccination may prove a gateway to increased COVID vaccination. If it is indeed too late for this link to manifest for this pandemic, then it is worthwhile to explore such an effort to curb hospitalisation and death in the next one.
References
Barber A and J West (2022), “Conditional cash lotteries increase COVID-19 vaccination rates”, Journal of Health Economics 81:102578.
Bennett N G, D E Bloom and M Ferranna (2022), “Factors underlying COVID-19 vaccine and booster hesitancy and refusal, and incentivizing vaccine adoption”, PLOS One 17(9): e0274529.
Campos-Mercade P, AN Meier, S Meier, D Pope, FH Schneider and Wengström E (2021), “Monetary incentives increase COVID-19 vaccinations, nudges do not”, VoxEU.org, 19 Nov.
Chang T, M Jacobson, M Shah, R Pramanik and S Shah (2021), “Financial Incentives and Other Nudges Do Not Increase COVID-19 Vaccinations among the Vaccine Hesitant”, NBER Working Paper No. 29403.
Deiana C, A Geraci, G Mazzarella and F Sabatini (2022), “Perceived risk and vaccine hesitancy”, VoxEU.org, 23 Apr.
Galasso V, V Pons, P Profeta, M Becher, S Brouard and M Foucault (2022), “From anti-vax intentions to vaccination: panel and experimental evidence from nine countries”, NBER Working Paper No. 29741.
Karaivanov A, D Kim, SE Lu and H Shigeoka (2022), “COVID-19 Vaccination Mandates and Vaccine Uptake.” Nat Hum Behav: 1-10.
Larson H, E Gakidou and C Murray (2022), “The vaccine-hesitant moment,” New England Journal of Medicine 387: 58-65.
Walkey AJ, A Law and NA Bosch (2021), “Lottery-Based Incentive in Ohio and COVID-19 Vaccination Rates”, JAMA 326(8):766.