The prevalence of child malnutrition has been falling in recent years, but it remains a persistent global problem. Child malnutrition is often proxied by child stunting, i.e. the percentage of children aged 0 to 5 in a population whose height is less than two standard deviations below the WHO child growth standard. Stunting is a key indicator in the Millennium and Sustainable Development Goals.
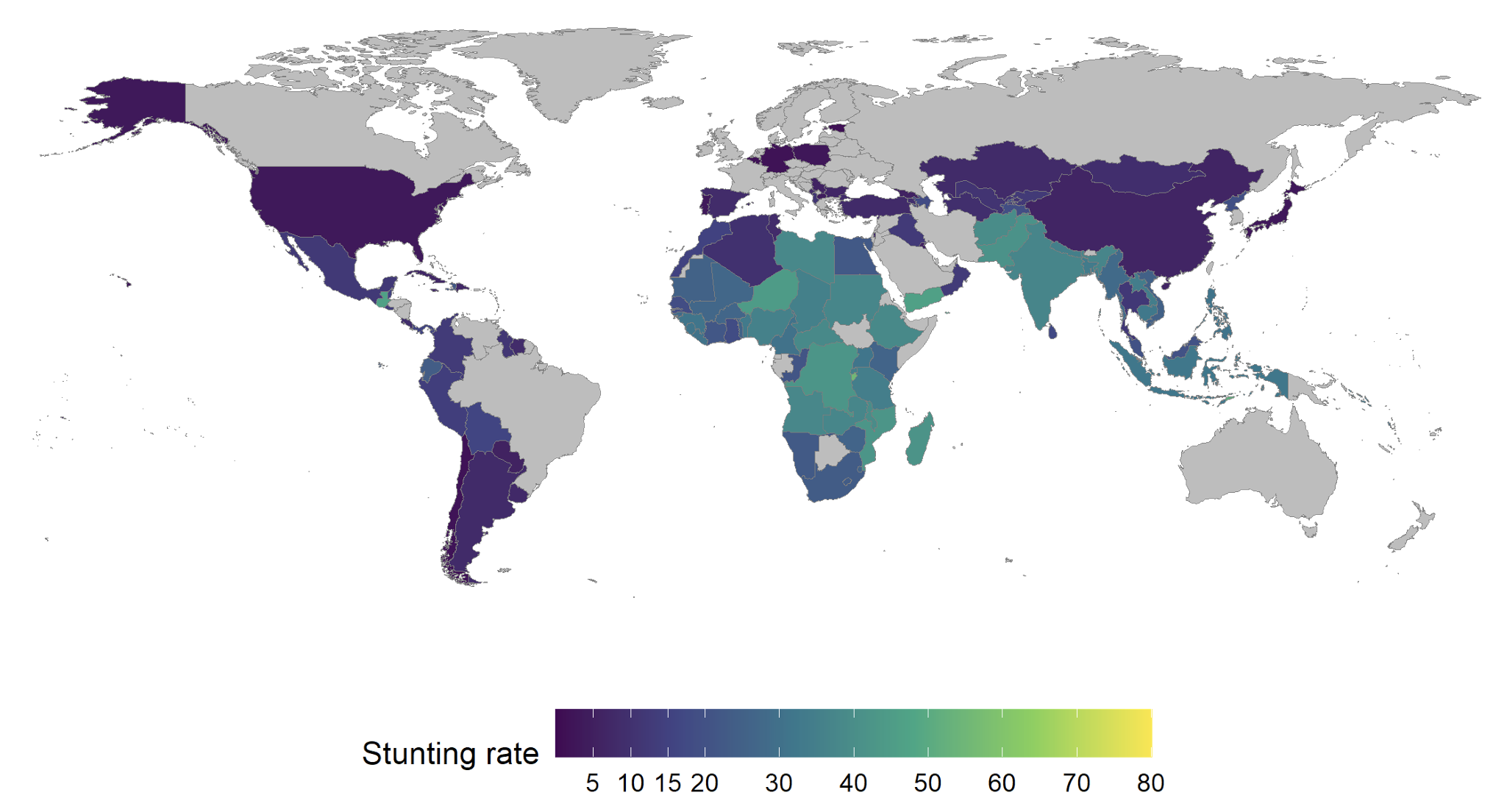
Child stunting is concentrated in South and Southeast Asia and sub-Saharan Africa (Figure 1). Global child stunting has fallen from 33.0% of children in 2000 to 22.3% of children in 2022, but there are still 148.1 million children under age five who are stunted today (UNICEF/WHO/World Bank 2023). Stunted children experience poorer health and human capital outcomes and lower income in later life, making eliminating child stunting a policy priority for many low- and middle-income countries (LMICs) (Currie 2008, Hoddinott et al. 2013).
Figure 1 Child stunting in the 2010s
Sources: UNICEF/WHO/World Bank (2023) supplemented with the Worldwide Historical Child Stunting Dataset (Schneider et al. 2023).
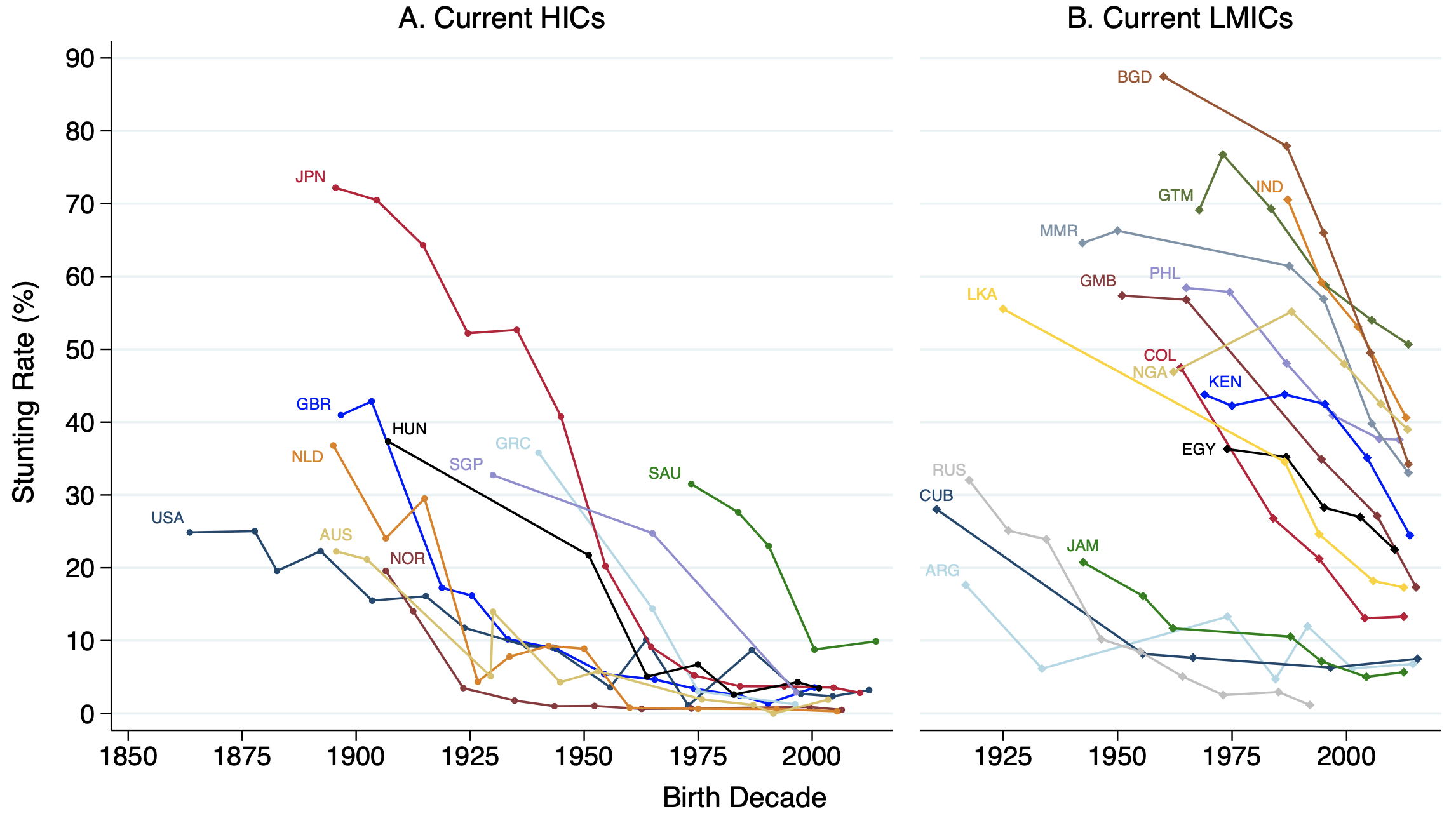
Most existing research on child stunting focuses on the past 40 years, but taking a long-run, global perspective on child stunting helps to clarify the determinants of child stunting (Schneider 2023). In a recent paper (Schneider et al. 2023), my co-authors and I reconstruct child stunting rates for 123 countries since the mid-19th century. Stunting rates for 25 selected countries with reliable data are presented in Figure 2 to give a sense of the historical variation.
Figure 2 Historical child stunting rates for current high-income countries and low- and middle-income countries
Notes: These data are preliminary, based on ongoing research. Historical stunting estimates are far more common for children over age 2, so children under age 2 are excluded from all stunting estimates in the graphs for consistency. HIC = high-income country; LMIC = low- and middle-income country. Sources: see Figure 1.
Panel A reports the historical stunting experiences of countries currently classified as high-income countries by the World Bank. While stunting rates appear to always have been relatively low in the European settler colonies in the New World and in Scandinavia, European countries had higher levels of child stunting at the beginning of the 20th century than many low- and middle-income countries today. Western European countries experienced a decline in stunting in the first quarter of the 20th century, while Eastern and Southern European countries experienced a later decline. Stunting rates were exceptionally high in Japan at the end of the 19th century, but over the 20th century, Japan saw a complete eradication of child stunting.
Panel B extends the existing data in the Joint Malnutrition Estimates produced by UNICEF, WHO, and the World Bank for countries currently classified as LMICs. Stunting rates have clearly fallen in LMICs since the mid-20th century. South Asian countries appear to have had higher stunting rates than sub-Saharan African countries throughout time. This gap has been termed the ‘Indian enigma’, since child stunting is lower in sub-Saharan Africa than in India despite India’s strong economic performance in recent years. Finally, we see that some low- and middle-income countries have had surprisingly low stunting rates across the 20th century. This particularly applies to Cuba, Jamaica and many other Caribbean countries, which had relatively low stunting rates in the mid-20th century despite their poverty.
So what explains the large heterogeneity in stunting rates across countries and over time? I survey the literature in detail in Schneider (2023), but several of the most important potential determinants are discussed below.
Genetics
Some may look at Figure 2 and wonder whether genetic differences in child growth between populations can explain the differences in stunting rates. While this is difficult to completely rule out, the eradication of child stunting from Japan over the 20th century from a very high level suggests that genetic factors are not preventing the elimination of stunting from India.
Economic growth
Economic growth might reduce child stunting by increasing incomes so that families can buy greater quantities and better-quality diets and spend more on hygiene and healthcare. Richer economies can also invest in public goods like sanitation and clean water that can reduce the burden of chronic disease for young children. However, research on low- and middle-income countries has shown that GDP growth since the 1990s was not associated with population declines in child stunting (Vollmer et al. 2014).
This mirrors findings from 19th-century Europe and North America, where some countries experienced decreases in adult stature during the onset of modern economic growth during industrialisation (Cinnirella 2008, Komlos 1998). This decline in stature was associated with the deterioration of the urban environment and growing inequality during the early stages of industrialisation. However, the association between economic growth and adult stature became positive in the 20th century (Hatton 2014), suggesting that GDP growth could have a less ambiguous role in LMICs in the future, once more of them get past the early stages of development, where the costs to health of economic growth from urbanisation, crowding and pollution outweigh the benefits.
Malnutrition
Although stunting is an indicator of malnutrition, nutrition may be less important for eliminating stunting than one might think. There is substantial evidence that animal sources of food such as milk and eggs can promote child growth (Headey et al. 2018). In the 19th century, countries with greater cattle density had taller populations (Baten and Blum 2014).
However, trends in stunting do not seem to be correlated with trends in nutrition. Calorie and protein consumption per capita fell in India between 1985 and 2009 even as there were modest improvements in stunting (Deaton and Dréze 2009). Likewise, Britain had reached adequate levels of calories and protein by the early 20th century, before its decline in child stunting (Gao and Schneider 2021). Nutritional interventions in current low- and middle-income countries have also not been as successful in eradicating stunting as one might hope (Bhutta et al. 2013). Thus, the most important drivers of stunting decline may not be related to nutrition.
Water, sanitation, and hygiene (WASH)
Unclean water and poor sanitation and hygiene affect child growth by increasing the prevalence of diarrhoeal diseases, which prevent children from absorbing the nutrients they consume. Spears (2020) argues that the greater prevalence of open defecation in India can account for the Indian enigma. WASH may also explain the low stunting rates in Jamaica in the mid-20th century. The Rockefeller Foundation launched an anti-hookworm campaign in Jamaica in the 1920s that built improved latrines, significantly reducing the prevalence of open defecation and the diarrhoeal mortality rate (Riley 2005).
However, WASH interventions have not been particularly successful in reducing child stunting (Pickering et al. 2019) in part because they require sustained individual-, household- and community-level behaviour change. Economic historians have also shown that the introduction of clean water and sewerage had a relatively small effect on infant diarrhoeal mortality rates (Anderson et al. 2020), raising doubts about whether WASH interventions can explain the decline in stunting in high-income countries in the early 20th century.
Gender bias
Systematic discrimination in the allocation of household resources against girls may also contribute to child stunting. Pande and Jayachandran (2015) argue that preference for first-born sons in India leads to poorer stunting outcomes for other children, explaining half the stunting gap between India and sub-Saharan Africa. The evidence for similar gender discrimination in Europe historically is mixed, although there is evidence that parents reinforced health endowments for girls following the 1923 Great Kanto earthquake in Japan (Ogasawara 2022). However, since household allocation simply steals from one child in favour of her siblings, it is unlikely to explain the dramatic reductions in child stunting over time.
Poor maternal health
Poor maternal health may be another cause of child stunting, since poor health conditions in utero lead children to be small at birth. Coffey (2015) showed that 42.2% of women at risk of pregnancy in India are underweight compared to 16.5% in sub-Saharan Africa. Both figures are substantially higher than underweight estimates for working-class women in Britain and the US in the 19th century (Carson 2018, Meredith and Oxley 2015). These differences may explain some of the variation in mean birth weights around the world.
While mean birth weights have been persistently high since the late 19th century in Europe and North America (Schneider 2017), birth weights are substantially lower in LMICs but have shown improvements in recent years (Blencowe et al. 2019). These contrasts in maternal health and birth weight may be the largest difference between the experience of stunting decline in historical high-income countries and current LMICs.
The variety of factors affecting stunting highlighted in this column suggests that there is no silver bullet to eradicate child stunting. The causes of stunting are multifaceted and therefore a context-sensitive approach to reduce stunting is needed in each country (Nisbett et al. 2023).
Two factors have been relatively overlooked in existing research. The first is people’s attitudes toward health, hygiene and sanitation. WASH interventions require people to fundamentally change their most closely held habits and health behaviours. This change in perspective took place in countries that eliminated stunting.
The second factor is generalised development, where over time people have more resources and human and social capital to expend on cleaning their living space, learning about and adopting new hygiene technologies, moving to less crowded and more hygienic homes and neighbourhoods and demanding better public health provision from governments. The interconnections between income, housing quality, neighbourhood amenities and governance make it difficult to separate these factors econometrically, but these less measurable factors likely mattered a great deal.
References
Anderson, D M, D I Rees, and T Wang (2020), “The phenomenon of summer diarrhea and its waning, 1910–1930”, Explorations in Economic History 78: 1–11.
Baten, J, and M Blum (2014), “Why are you tall while others are short? Agricultural production and other proximate determinants of global heights”, European Review of Economic History 18(2): 144–165.
Bhutta, Z A, J K Das, A Rizvi, M F Gaffey, N Walker, S Horton, P Webb, A Lartey, R E Black, and the Maternal and Child Nutrition Study Group (2013), “Evidence-based interventions for improvement of maternal and child nutrition: What can be done and at what cost?”, The Lancet 382(9890): 452–77.
Blencowe, H, J Krasevec, M de Onis, R E Black, X An, G A Stevens et al. (2019), “National, regional, and worldwide estimates of low birthweight in 2015, with trends from 2000: A systematic analysis”, The Lancet Global Health 7(7): e849–e860.
Carson, S A (2018), “Black and white female body mass index values in the developing late 19th and early 20th century US”, Journal of Bioeconomics 20(3): 309–30.
Cinnirella, F (2008), “Optimists or pessimists? A reconsideration of nutritional status in Britain, 1740–1865”, European Review of Economic History 12(3): 325–54.
Coffey, D (2015), “Prepregnancy body mass and weight gain during pregnancy in India and sub-Saharan Africa”, Proceedings of the National Academy of Sciences 112(11): 3302–7.
Currie, J (2008), “Child health and the intergenerational transmission of human capital”, VoxEU.org, 19 July.
Deaton, A, and J Dréze (2009), “Food and nutrition in India: Facts and interpretations”, Economic and Political Weekly 44(7): 42–65.
Gao, P, and E B Schneider (2021), “The growth pattern of British children, 1850–1975”, The Economic History Review 74(2): 341–71.
Hatton, T J (2014), “How have Europeans grown so tall?”, Oxford Economic Papers 66(2): 349–72.
Headey, D, K Hirvonen, and J Hoddinott (2018), “Animal sourced foods and child stunting”, American Journal of Agricultural Economics 100(5): 1302–19.
Hoddinott, J, J R Behrman, J A Maluccio, P Melgar, A R Quisumbing, M Ramirez-Zea, A D Stein, K M Yount, and R Martorell (2013), “Adult consequences of growth failure in early childhood”, American Journal of Clinical Nutrition 98(5): 1170–78.
Komlos, J (1998), “Shrinking in a growing economy? The mystery of physical stature during the Industrial Revolution”, The Journal of Economic History 58(3): 779–802.
Meredith, D, and D Oxley (2015), “Blood and bone: Body mass, gender and health inequality in nineteenth-century British families”, The History of the Family 20(2): 204–30.
Nisbett, N, J Harris, D Headey, M van den Bold, S Gillespie, N-L Aberman et al. (2023), “Stories of change in nutrition: Lessons from a new generation of studies from Africa, Asia and Europe”, Food Security 15(1): 133–49.
Ogasawara, K (2022), “Persistence of natural disasters on children’s health: Evidence from the Great Kantō Earthquake of 1923”, The Economic History Review 75(4): 1054–82.
Pande, R and S Jayachandran (2015), “Son preference drives India’s high child malnutrition rates”, VoxEU.org, 5 May.
Pickering, A J, C Null, P J Winch, G Mangwadu, B F Arnold, A J Prendergast, S M Njenga, M Rahman, R Ntozini, J Benjamin-Chung, C P Stewart, T M N Huda, L H Moulton, J M Colford, S P Luby, and J H Humphrey (2019), “The WASH Benefits and SHINE trials: Interpretation of WASH intervention effects on linear growth and diarrhoea”, The Lancet Global Health 7(8): e1139–e1146.
Riley, J C (2005), Poverty and life expectancy: The Jamaica paradox, New York: Cambridge University Press.
Schneider, E B (2017), “Fetal health stagnation: Have health conditions in utero improved in the US and Western and Northern Europe over the past 150 years?”, Social Science and Medicine 179: 18–26.
Schneider, E B (2023), “The determinants of child stunting and shifts in the growth pattern of children: A long-run, global review”, CEPR Discussion Paper 18367.
Schneider, E B, J Jaramillo Echeverri et al. (2023), “Worldwide child stunting since the mid-nineteenth century”.
Spears, D (2020), “Exposure to open defecation can account for the Indian enigma of child height”, Journal of Development Economics 146: 102277.
UNICEF, WHO, and World Bank Group (2023), Levels and trends in child malnutrition: Key findings of the 2023 edition, Geneva.
Vollmer, S, K Harttgen, M A Subramanyam, J Finlay, S Klasen, and S V Subramanian (2014), “Association between economic growth and early childhood undernutrition: Evidence from 121 demographic and health surveys from 36 low-income and middle-income countries”, The Lancet Global Health 2(4): e225–e234.